Diagnostic and Management Difficulties of Complete Atrioventricular Block In Children in Marrakech: A Report of Three Cases With a Review of the Literature
Mounia Khramaz, MD1, Salwa Elkarimi1, Dounia Benzerroual1, Mustapha Elhattaoui1, Fahd Aboutofail2, Drissi Boumzebra2, Rachid Elhaouati2
1Departement of Cardiology, Cadi Ayyad University, Lab. PCIM, Mohammed the 6th University Hospital, Marrakech, Morocco.2Departement of Cardiovascular Surgery, Cadi Ayyad University, Lab. PCIM, Mohammed the 6th University Hospital, Marrakech, Morocco.
Complete atrioventricular (AV) block is a rare affection in children. It is the consequence of abnormal conduction tissue within a cardiac malformation or it is due to cardiac injury.
Yet the etiology of late complete atrioventricular block in child remains mostly unknown. The treatment of children's Complete atrioventricular block is the implantation of a pacemaker with immediate results satisfactory in the absence of associated cardiomyopathy. In this observation we will treat three cases.
Key Words : Complete Atrioventricular Block, Children, Pacing, Myocarditis.
Correspondence to: Mounia Khramaz, Dar saada, imm 129, 4éme étage, N°3 Marrakech, Morocco.
A 11-year-old boy was admitted to the hospital following a syncopal episode. He denied chest pain, palpitations, or dyspnea. No story of fever, emesis, diarrhea, rhinorrhea, or sore throat. He had no history of significant medical illnesses prior to this event and no family history of heart disease or sudden death.
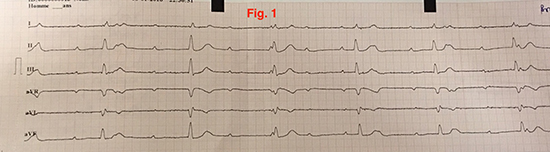
An initial EKG performed in the field showed a high-degree atrioventricular (AV) block with a ventricular rate of 33 bpm (Fig.1). He was afebrile, and his blood pressure was 100/60 mmHg, with normal respiratory rates oxygen saturation. He was awake and responsive, and no abnormalities were detected upon complete physical examination.
Figure 1. The electrocardiogram demonstrates the complete atrio-ventricular block with ventricular escape beat rate 31 beats/min on the day of admission. The flat P waves in lead I and negative P waves in lead aVL suggested left atrial rhythm which may be related to myocarditis
Laboratory studies were unremarkable for a troponin level of 2.64 μg/L, a white blood cell count of 7,400 μL with 48% lymphocytes, mildly elevated aspartate aminotransferase of 53 U/L, and normal C-reactive protein at 3.3 mg/L. Serum electrolytes and brain natriuretic peptide levels were within normal limits. A chest x-ray showed an appropriate cardiac size and silhouette. Echocardiogram demonstrated normal anatomy and function. Multiple laboratory studies were ordered (for the child and his mom), but a causative pathogen was not identified. her Holter monitor confirmed the diagnosis of persistent CAVB. Permanent pacemaker placement was required.
The second, was a 9-year-old girl, presented with history of recurrent lower respiratory tract infections since the age of 2 months. Physical examination was normal. Baseline 12-lead electrocardiogram (EKG) showed normal sinus rhythm with no conduction delays. Transthoracic echocardiography showed a 16 mm ostium secundum ASD with dilated right atrium. Pulmonary arterial pressure was normal. She underwent a total repair of the ASD. EKG monitoring during the procedure was within normal limits. Post procedure 2D echocardiography showed no residual shunt. EKG monitoring at 12 h showed complete heart block (CHB) with a ventricular rate of 61 beats per minute. The patient was asymptomatic and hemodynamically stable. temporary pacing was required. She was started on a course of oral prednisolone at 2 mg/kg/day to decrease the inflammation and edema around the AV node thought to cause the conduction problems. Her rhythm was checked at 12-h intervals by shortly turning off the pacemaker and recording the patient’s ECG. On day 16, patient reverted to normal sinus rhythm with no conduction delays or blocks. No permanent pacemaker placement was required and patient was discharged to home with frequent visit for follow up. She continues to remain asymptomatic and in normal sinus rhythm with no recurrence of heart block.
The third patient is a 7-year-old girl was brought to the emergency department (ED) after a 3 episodes of syncope within the past 2 days without palpitations or prodromal symptoms. The patient had no significant medical or family history without any complaints of dizziness, dyspnea, palpitations, or chest pain. She had recent symptoms (fever, rhinorrhea, and sore throat) suggestive of a viral illness. She was taking Paracetamol for her fever and Amoxicillin for 5 days. The patient was awake and oriented, with a normal blood pressure of 110/60 mm Hg, heart rate of 75 beats per minute, respiration rate of 20 breaths per minute, and temperature of 38.4ºC.
Results of laboratory tests, including serum electrolyte levels, complete blood cell counts, were normal. Serum cardiac markers were abnormal: creatine phosphokinase, 1064 U/L (normal, 150 U/L); troponin T, 61.2 mg/L (normal, less than 0.05 ng/mL), CRP, 52mg /L; VS, 110 in the first hour. A chest film showed no cardiomegaly or pulmonary congestion, and transthoracic echocardiography showed pericardiac effusion with no other abnormalities.
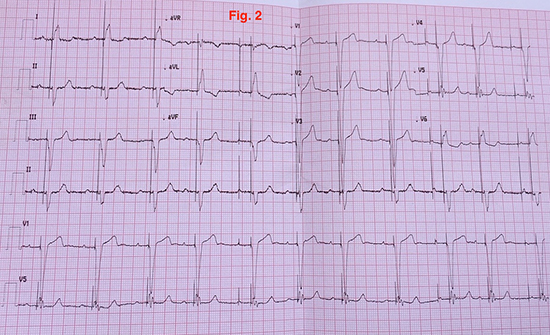
The parents refused MRI with gadolinium contrast and endomyocardial biopsy. The child was treated with prednisone. Permanent pacemaker was necessary for persistent bradycardia. Follow up showed a normal heart function on echocardiography (Fig. 2).
Figure 2. ECG after pacing with beat rate 62/min
The aim of permanent pacing therapy in patients with complete AV block is to restore heart rhythm and rate, relieve the patient from bradycardia-related symptoms, provide haemodynamic stability, and thereby improve patient well-being and clinical outcome.1 Selecting a pulse generator and pacing lead for a child who needs life-long pacing for complete AV block depends on several important factors.2 The psychological impact of pacemaker implantation in a child must be taken into account. This is especially true of the adolescent who may have to significantly alter his or her lifestyle as a result of this intervention.3
The CAVC is a cause of postoperative cardiac morbidity following repair of congenital heart disease, Current practice dictates implantation of permanent pacemaker (PPM) when post-op CAVB persists > 9 days.2
Congenital complete atrioventricular block (CCAVB) has described by Morquio in 1901, it has been of interest in the past primarily because of the risk of sudden cardiac death This complication may be the initial manifestation of congenital AV block, even in previously asymptomatic patients3 In this case, there are specific indications for implantation of a pacemaker. Some observations support the hypothesis that late progression to CAVB can be the result of an immune-mediated pathogenetic mechanism during foetal life. An autoantibody-associated diagnosis after the neonatal period is therefore possible, and testing of maternal serology at the time of diagnosis is recommended.4
Myocarditis complicated with complete atrioventricular block (CAVB) is rare in children. The clinical symptoms of acquired CAVB related to myocarditis are often characterized by acute onset of symptoms of low cardiac output due to a slow ventricular rate that may even lead to hypotension or Stokes-Adams seizures.5 The cardiac enzyme may be abnormal. At disease onset, patients may report various specific or non-specific symptoms, such as fever, general malaise, dyspnea, chest pain, abdominal pain, nausea or vomiting. The development of CAVB probably followed the severe acute inflammation of the bundle branches.6 The severity of the pathological changes of the AV conduction system may reflect the extent of reversibility of the CAVB.
Previous pediatric reports regarding the clinical course of CAVB after myocarditis were mostly case reports or small case series, some review tried to summarize them (Mei-Hwan Wu) but stile non suffisent to optimize the outcome.7
In general, AV block refers to a conduction delay or interruption of the impulses generated in the atrium before they reach the ventricles. AV block may be transient or permanent, and the anatomic level at which it occurs varies. These features determine the clinical significance of this condition, which may range from minimal to severely symptomatic, including syncope, congestive heart failure, or sudden death.