Emergency Department Readmission in Elderly Patients After Acute Rhythm or Rate Control Treatment for Atrial Fibrillation
Bonora Antonio1, Turcato Gianni2, Franchi Elena3, Dilda Alice1, Taioli Gabriele2, Serafini Valentina2, Sivero Valentina2, Zannoni Massimo1, Ricci Giorgio1, Olivieri Oliviero4
1Emergency and Intensive Care Department, Azienda Ospedaliera Universitaria Integrata, Verona, Italy.2Emergency and Intensive Care Department, Azienda Ospedaliera Universitaria Integrata, Verona, Italy, Postgraduate School of Emergency Medicine, University of Verona, Italy.3Department of Cardiology, Azienda Ospedaliera Universitaria Integrata,Verona, Italy.4Professor of Internal Medicine, Department of Internal Medicine, Azienda Ospedaliera Universitaria Integrata,Verona, Italy, Chief of Postgraduate School of Emergency Medicine, University of Verona, Italy.
Atrial fibrillation (AF) is an age-related increasing disease, characterized by a high number of relapses frequently leading the patients to Emergency Department (ED). Despite AF relapses may be clinically heterogeneous, a proper management requires either a fast and effective restore of the sinus rhythm or a satisfactory control of the ventricular rate. Whether the strategy adopted in the ED could affect the course of disease is still debated.
Therefore, the aim of our study was to evaluate the number of ED readmission for AF related symptoms and the event-free period in patients older than 70 years previously treated in ED for an AF recurrence, in order to assess a possible relationship with the acute strategy.
An overall number of 302 recurrences of AF were drawn randomly, regarding 102 patients (mean age 78 years). We found that 206 cases (68.2%) were treated with rhythm restoration strategy (RR) whereas 96 (31.8%) with rate control strategy (RC). The median following event-free period was 118.6 +/- 15.5 and 212.9 +/- 37.1 days (p < 0.05) for RR and RC strategy, respectively. Within 6 months, 124 (60.1%) out of RR group patients and only 44 (45.8%) out of RC group patients had to be readmitted to ED for AF related symptoms (whether a recurrence or inefficient rate control symptoms) (p< 0.05). This advantage was substantially confirmed (79.1% vs 65.6% respectively, p < 0.05) after a 12 months follow-up. Our results indicate that acute treatment of AF may affect the long-term outcome of the disease and the ED readmission rate of the patient. Ventricular rate control seems to be associated with a longer event-free period if compared to the rhythm control strategy in the elderly patients. This suggests an age-based work-up of patients admitted to the ED, preferentially using ventricular rate control in elderly subjects.
Key Words : Atrial Fibrillation, Rate Control, Rhythm Control, Recurrences.
Correspondence to: Bonora Antonio, UOC Pronto Soccorso Policlinico G.B. Rossi, Borgo Roma – AOUI Verona – P.le Scuro, Scuro 10, 37134 – Verona, Italy.
Atrial fibrillation (AF) is the most frequent arrhythmic disorder in Western countries and may occur in more than 1% of general population,1,2 its incidence raising up 18% in over 80 years people.3,4 Ageing process in the general population will reasonably increase such prevalence, so that about 18 millions of European people are estimated to be affected by AF within the next 4-5 decades.5,6,7
The natural course of AF is often characterized by a sequence of relapses leading to a final condition of established chronic arrhythmia.8 Moreover, the clinical manifestations of AF relapses very often force patients to refer themselves to Emergency Department (ED), thus representing a common clinical issue for emergency physicians. Notably, the relapse rate after the first episode of AF is about 10% in the first 12 months and 5% in the following years.9
Currently, AF relapses overall account for 3% of the ED readmissions, but it is easy to suppose that this feature will be substantially increased in the next few years as well the economic burden linked to the management of this disease.10,11,12
Despite clinical presentation of AF is heterogeneous and ranges from the isolated recognition of abnormal heart rhythm up to severe life-threatening conditions, all patients admitted to ED require a fast effective reversal of the arrhythmic disorder or, at least, the control of ventricular rate aimed to reassure satisfactory functional status and quality of life. For this reason, essential tasks for the Emergency Physician are
-
safe and effective management of the acute arrhythmia in order to obtain the recovery of the previous steady-state in relatively short time,
-
starting of adequate treatment able to prevent future AF related readmission to the ED.13
Currently, two approaches are available to achieve such goals: the first strategy is aimed to restore sinus rhythm (SR) either by electrical or pharmacological intervention; the second one is limited to gain a good ventricular rate control leaving the patient in chronic stable AF. The lack of reports comparing the different approaches and the several outcomes examined makes the best choice still uncertain.14 Particularly, whether the number of AF relapses and the disease-free period could depend on the strategy adopted in ED still remains an unsolved question.15,16
Therefore, we reviewed of all AF recurrences treated in our ED in the last five years in order to assess a possible relationship between the different strategy, rhythm or rate control, and the following relapses. In this report, we present the preliminary results obtained on a small subset of recurrences drawn randomly (n = 302). The aim of this preliminary study is to evaluate whether the rhythm or rate control strategies could influence the number of AF relapses in ED and then the event-free period.
“Index Events” and Inclusion Criteria
In this preliminary study we retrospectively evaluated 302 AF recurrences randomly drawn from all episodes of AF observed in the Emergency Department (ED) of General Hospital of Verona (Italy) from January 2010 to December 2014. We considered as “index event” any AF recurrence with a clearly inferable recent onset of the arrhythmia (< 96 hours).
The inclusion criteria were the following:
-
age > 70 years;
-
clinical history of previous AF episode already treated in our ED, in order to surely exclude a first diagnosed AF;
-
evidence of stable sinus rhythm (SR) before the present AF recurrence (index event);
-
well proven and datable ED readmission after the “index event” for AF-related symptoms, due either to symptomatic recurrence or unsatisfying rate control (relapse event).
We excluded from the analysis all patients with a permanent pace-maker or previously submitted to percutaneous transcatheter ablation procedures (Fig. 1).
Figure 1. Schematic summary of the study protocol
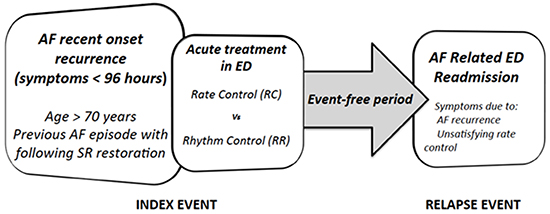
Statistical analysis was performed on all index events included in the dataset (n= 302).
Clinical reports of the AF recurrence (index event) of each patient enrolled in the study were examined. We collected data regarding previous clinical history and chronic therapy, the well-defined onset of symptoms, the electrocardiogram registered both at admission and discharge time and the treatment administered in ED.
All recorded index events were divided into two groups according to ED treatment:
-
strategy aimed at restoring the normal sinus rhythm (Rhythm control group – RR group);
-
strategy only aimed at controlling the ventricular rate without restoration of sinus rhythm (Rate control group – RC group).
All patients were treated with anticoagulant drugs.
Thereafter in each considered index event we verified:
-
the heart rhythm registered within a week from admittance;
-
following ED readmission either due to a new AF recurrence or symptoms related to an unsatisfying ventricular control (relapse event).
The time interval between the index event and the relapse event was defined as “event-free period” and considered as the outcome of this preliminary study.
Statistical analysis was performed using SPSS 22.0 (IBM Inc., Chicago, Illinois, USA). Quantitative values were compared by Student’s t-test for unpaired data, and expressed as means ± standard deviation or 95% interval confidence (95% CI); when necessary, logarithmic transformation was applied to obtain normal distribution and variability of the data was expressed as 95% confidence interval. Categorical variables were compared by chi squared test or Wilcoxon-Mann-Whitman test.
Comparison between the event-free time of the different treatments was performed by using Kaplan-Maier and Long Rank Test (statistical significance when p < 0.05). Relapses and ED readmission rates were compared by Fisher’s exact test.
According to the preliminary study protocol and the inclusion and exclusion criteria, an overall number of 302 clinical folders regarding ED admissions for AF datable recurrence were finally evaluated. The study population consisted of 102 patients (mean age 78 years, range 70-93), with a median of 2 events for patient (range 1-9).
In 144 (47.7%) out of these events, the onset of symptoms lasted within three hours, in 120 (39.7%) between 3 and 24 hours, and in 39 (12.6%) between 48 and 72 hours. The main clinical features including details of the previous home therapy of these patients are reported in Table 1 and 2.
Table 1. Associated diseases
|
RR (n = 206)% |
RC (n = 96)% |
p-value |
| Sex |
|
|
0.802 |
| Male |
84 (40.8) |
41 (42.7) |
|
| Female |
122 (59.2) |
55 (57.3) |
|
| Age |
78 (74 – 82) |
78 (75 – 83) |
1.000 |
| Onset |
|
|
0.034 |
| < 12 h |
167 (81.1) |
42 (43.8) |
|
| 12 – 24 h |
18 (8.7) |
10 (10.4) |
|
| 24 – 48 h |
20 (9.7) |
7 (7.3) |
|
| 48 – 96 h |
1 (0.5) |
37 (38.5) |
|
| Onset symptoms |
|
|
|
| Dyspnoea |
9 (4.4) |
8 (8.3) |
0.184 |
| Fatigue |
25 (12.1) |
34 (35.5) |
0.001 |
| Chest pain |
14 (6.8) |
5 (5.2) |
0.800 |
| Hypertension |
187 (90.8) |
88 (91.7) |
1.000 |
| Cronic Heart Failure |
14 (6.8) |
5 (5.2) |
0.800 |
| Ischemic heart disease |
38 (18.4) |
13 (13.5) |
0.326 |
| Cardiomyopathy |
2 (1.0) |
2 (2.1) |
0.594 |
| Valvular heart disease |
44 (21.4) |
21 (21.9) |
1.000 |
| Diabetes |
13 (13.5) |
20 (9.7) |
0.327 |
| Dyslipidemia |
49 (23.8) |
27 (28.1) |
0.477 |
As regards the therapeutic strategy adopted, in 206 (68.2%) out of 302 recurrence it was aimed to restore SR by means of either electrical or pharmacological interventions (RR), whereas in the remaining 96 (31.8%) ED treatment strategy was limited to heart rate control (RC).
Table 2. Drug history
|
RR (n = 206) |
RC (n = 96) |
p |
| Beta blocker |
71 (34.5) |
48 (50.0) |
0.012 |
| Ca-Antagonist |
38 (18.4) |
24 (25.3) |
0.220 |
| ACE inhibitors / ARBs |
143 (69.4) |
65 (67.7) |
0.894 |
| Antiarrhythmic |
114 (55.3) |
33 (34.4) |
0.001 |
| Digital |
2 (1.0) |
3 (3.2) |
0.168 |
| Diuretics |
97 (47.1) |
48 (50.5) |
0.620 |
| ASA |
78 (37.9) |
46 (48.4) |
0.101 |
| Anticoagulant |
70 (34.0) |
28 (29.5) |
0.509 |
A stable restoration of normal sinus rhythm before discharge was obtained in 181 recurrences out of 302 (59.9%), 151 of which in the RR group and 30 in the RC group (p < 0.05).
At one week evaluation from discharge SR was reported in 191 of 206 (92.7%) in the RR group and 65 of 96 (67.4%) in RC group (p < 0.05).
Notably, all the 12 early relapses (< 7 days) occurred in subjects treated according to the RR strategy.
As regards the following ED readmission for any AF related symptoms (either AF recurrence or unsatisfactory rate control) the median event–free period without AF related ED admission was 212.9 +/- 37.1 days for RC and 118.6 +/- 15.5 days for RR strategy (p < 0.05). In the Fig. 2 are shown the Kaplan-Meier time curves for both these strategies.
Figure 2. Atrial Fibrillation related event-free period (months) after an AF recurrence
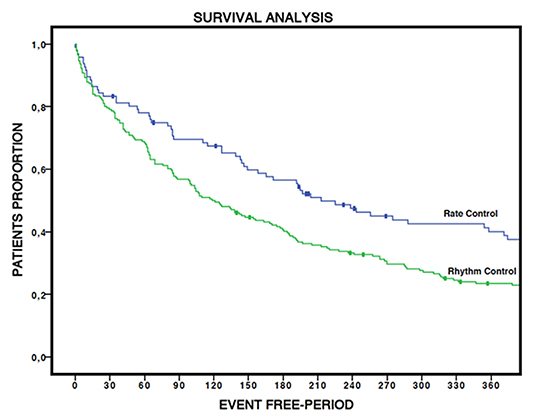
There were no substantial differences in terms of ED readmission between RC and RR strategies during the first month (16.7% vs 20.9% respectively, p > 0.05), as shown in Fig. 2, but we found a significant difference after 6 and 12 months (Table 3): particularly, 6 months later, the 60.1 % of the patients in RR group whereas only the 45.8% of those in RC group had to be readmitted to ED due to AF (p < 0.05). Within a 12 months follow-up period, this trend was substantially confirmed (79.1% vs 65.6% respectively, p < 0.05).
Table 3. Recurrence rate
| Recurrence rate |
RR (n = 206) |
RC (n = 96) |
p |
| Recurrences 1 month |
43 (20.9) |
16 (16.7) |
0.438 |
| Recurrences 3 months |
90 (43.7) |
31 (32.3) |
0.077 |
| Recurrences 6 months |
123 (60.1) |
44 (45.8) |
0.025 |
| Recurrences 12 months |
143 (79.1) |
63 (65.6) |
0.015 |
In the subgroup of patients who experienced restoration of the sinus rhythm either during the ED stay or within the following week (as verified by means of a Cardiologist visit), the median period of well-being was 103.4 days +/-14.5 for RR group and 165.3 days +/- 30.1 for RC group (p < 0.05).
Our preliminary results suggested that in over 70 years-old patients the rate control management of AF recurrences in ED could lead to a wider event-free period.
In a recent long-term follow-up study AF is reported to have a slow progression from an isolated form (“lone AF”) to a sustained ones, since many years could lapse within the first and the second episode.8 However, when the underlying structural disease has worsened, AF episodes occur as a cluster of more or less near recurrences, forcing the patients to several admittances in ED.2,8
Therefore we though convenient to exclude all the first episodes of AF and to consider the recurrences only. A better understanding of the natural history of AF could improve the management of recurrences and reduce the need for acute treatment.
Our study is retrospective and moreover preliminary, being carried out on a small number of patients, and thus the apparent larger effectiveness of rate-control strategy in reducing AF relapses in elder population has to be confirmed in a wider series.
However, to the best of our knowledge, this is one of the first study evaluating in elder patients observed in Emergency Department (ED), a setting where a fast therapeutic response is needed, the long-term results of rhythm control versus rate control strategy, not only in terms of AF recurrences but also of symptoms related to an inadequate ventricular rate control.
Moreover, for the very first time the event-free period has been considered as an outcome in the acute management of AF recurrences. This could represent a novel key to assess the best treatment for AF in elder patients, where the requirement of stable circulatory performance is often a priority in comparison with the need for restoring sinus rhythm.
Main international trials, like AFFIRM,17 STAF,18 and RACE,19 that compared rate to rhythm control in AF management, considered patients clinically stable and followed-up by a cardiologist in settings other than the ED. Instead, AF recurrence develop within hours, can be heavily symptomatic and therefore require the rapid intervention of the emergency physician.20 Our study focused on patients managed in the ED for a “ recent onset” recurrence of AF. Most of the enrolled patients (87.4%) were admitted to ED within 24 hours from the onset of symptoms and over 47% of them within 3 hours. On the contrary, the AFFIRM trial mostly enrolled patients with AF lasting more than 48 hours (69.2%), and other studies like PIAF, RACE, STAF, HOTCAFE’ only patients suffering from persistent AF (> 7 days).17,18,19,20,21,22 The elder age is another distinctive feature of the patients considered in our study. As matter of fact, AF represents an age-related disease and in the ”real word” mean age of the affected individuals has been continuously increasing. This epidemiological observation made us to focuse our attention to older people, aged at least 70 years (mean age 78 years), thus drawing a further difference from above mentioned international trials where a younger population was studied, generally in the sixth decade of life.
Also the endpoint considered in the present study was quite different from previous trials. AFFIRM considered the overall mortality,17 AF-CHF cardiovascular mortality21 and PIAF symptoms improvement. Other studies like RACE, STAF, J-RHYTM22 had different composite endpoints. Our main endpoint was the event-free period, defined as the period ranging from the acute treatment in ED for an AF recurrence to the following relapse of any symptom associated with not (or poorly) controlled underlying arrhythmia.
The primary outcome of the present study resulted to be clearly applicable since the patients undergoing rate control strategy showed an event-free period significantly longer than those treated with rhythm control strategy (212.9 vs 118,6 days respectively, p < 0.05). Moreover, the former is burdened by lower hospitalization rates if compared to the latter group.
Our findings appeared to be consistent with the results achieved by Chatterjee et al.23,24 Similarly, Shariff et al.25 reported that in population aged > 70 years the rate control is superior to the rhythm control in terms of mortality and hospitalization, suggesting that an adequately stable ventricular rate may allow a better quality of life in elderly patients and probably reduce the related health care costs.
For long time, rhythm control with fast restoration of sinus rhythm was considered the strategy of choice,26,27 in order to delay the evolution toward a permanent AF.28,29,30 This assumption, probably correct in younger patients, seems disputable in older individuals because of pre-existing structural heart alterations and subsequent relative ineffectiveness of antiarrhythmic drugs.31
For these reasons, a longer well-being state in the elderly population may not necessarily require the restoration of sinus rhythm, being a controlled ventricular rate sufficient for this purpose. On the contrary, the sequential changes of rhythm by itself or the use of specific preventive drugs could paradoxically facilitate the AF relapses and thus consequent hospitalizations.
Although these hypothesis are speculative and need to be demonstrated, the results in the event-free period within ED readmissions is of main importance, mainly from the emergency physicians point of view.
However, this study is burdened by some remarkable limitations.
Firstly, this is a retrospective study with several difficulties common to such type of investigations and so the relevance of the present conclusions has to be carefully confirmed by appropriate, prospective, well controlled studies.
Secondly, the adherence to the home therapy in the event-free periods was far to be fully evaluated and possible drug changes or interferences (for example by “pill-in-the-pocket” approach) cannot be ruled out.
Finally, it has also been reported that recurrent episodes occur in approximately 90% of AF patients but many of these remain asymptomatic;32 we were unable to record such episodes that nevertheless did not appear to have any substantial or evident impact on the quality of life of the patients.
In spite of all these limitations, the study shows a picture of the “real world” ED population and the main end-point represents an outcome of objective importance for its related clinical and economical implications.
As matter of fact, if confirmed, these findings suggest an age-based stratification and work-up for the patients admitted to the ED for AF relapse, preferably addressing elderly people to rate control strategy while reserving the most challenging protocols of sinus rhythm restoration to the younger patients. Such approach should result more effective not only in terms of patient health but also in saving time and costs for the Emergency Department.
In a context of progressive ageing of the general population, AF relapses in elderly people probably will lead to an exponential increase of the number of ED admissions and a consequent increasingly economic burden for the public Health System in the next future. Thus, emergency physicians should be able to rapidly and safely manage acute AF symptoms and to restore the previous steady state of the patient.
Our preliminary study indicates that the acute treatment started by the emergency physician will probably affect the long-term outcome of the disease and the following hospital readmission rate of the patient. Ventricular rate control seems to be associated with a longer event-free and well-being period for the elderly patients if compared to the rhythm control strategy. This suggests an age-based work-up of the patients admitted to the ED, with a preferential choice of controlling the ventricular rate in elderly subjects, while reserving the most challenging protocols of cardiac synchronization to the younger patients.
Further prospective studies will be needed to definitely confirm possible advantages of such approach in the acute setting.