Patient Specific Induced Pluripotent Stem Cell-Derived Cardiomyocytes for Drug Development and Screening In Catecholaminergic Polymorphic Ventricular Tachycardia
Ronen Ben Jehuda1,2,3,4, Lili Barad1,2,3
1Department of Physiology, Biophysics and Systems Biology.2The Rappaport Institute.3Ruth and Bruce Rappaport Faculty of Medicine.4Department of Biotechnology, Technion, Haifa, Israel.
Catecholaminergic polymorphic ventricular tachycardia (CPVT), an inherited arrhythmia often leading to sudden cardiac death in children and young adults, is characterized by polymorphic/bidirectional ventricular tachycardia induced by adrenergic stimulation associated with emotionally stress or physical exercise. There are two forms of CPVT:
-
CPVT1 is caused by mutations in the RYR2 gene, encoding for ryanodine receptor type 2. CPVT1 is the most common form of CPVT in the population, and is inherited by a dominant mechanism.
-
CPVT2 is caused by mutations in the CASQ2 gene, encoding for cardiac calsequestrin 2 and is inherited by recessive mechanism.
Patient-specific induced Pluripotent Stem Cells (iPSC) have the ability to differentiate into cardiomyocytes carrying the patient's genome including CPVT-linked mutations and expressing the disease phenotype in vitro at the cellular level. The potency for in vitro modeling using iPSC-derived cardiomyocytes (iPSC-CMs) has been exploited to investigate a variety of inherited diseases including cardiac arrhythmias such as CPVT.
In this review we attempted to cover the majority of CPVT patient specific iPSC research studies previously published. CPVT patient-specific iPSC model enables the in vitro investigation of the molecular and cellular disease-mechanisms by the means of electrophysiologycal and Ca+2 imaging methodologies. Furthermore, this in vitro model allows the screening of various antiarrhythmic drugs, specifically for each patient, also known as "personalized medicine".
Key Words : Induced Pluripotent Stem Cell, Cardiomyocytes, Catecholaminergic Polymorphic Ventricular Tachycardia (CPVT), Personalized Medicine, Arrhythmia.
Correspondence to: Lili Barad, Department of Physiology, Biophysics and Systems Biology, Rappaport Faculty of Medicine, 1st Efron Street, POB 9649, Haifa, 31096 Israel.
Catecholaminergic polymorphic ventricular tachycardia (CPVT) is an inherited arrhythmia which may lead to syncope and sudden cardiac death in children and young adults. The arrhythmia is characterized by polymorphic/bidirectional ventricular tachycardia induced by adrenergic stimulation associated with emotional stress or physical exercise.1-4 CPVT is manifested in one of two forms depending on the mutated gene.
-
CPVT1 is caused by mutations in the RYR2 gene encoding the ryanodine receptor type 2, it is inherited by a dominant mechanism and constitutes 70% of the CPVT cases.
-
CPVT2 is caused by mutations in the CASQ2 gene encoding for cardiac calsequestrin 2,5-8 it is inherited by a dominant mechanism.
There are residual cases of CPVT that are caused by mutations either in TRDN, encoding for triadin or by mutations in CALM1, encoding for calmodulin; these residual CPVT cases are inherited by a recessive/dominant mechanism, respectively.10,11 RYR2, a homotetramer comprised of 4 pore-forming monomers, regulates Ca2+-induced Ca2+ release process (CICR) during excitation-contraction (EC) coupling by acting as a Ca2+ channel in the sarcoplasmic reticulum (SR) membrane.9,12,13 CASQ2 also regulates SR Ca2+ release by acting as a buffering factor with a high-capacity low-affinity Ca2+ binding function.5,8,9,12,13 RYR2 and CASQ2 are both involved in the EC coupling, operating as regulators of the Ca2+ handling machinery in cardiomyocytes.6,14,15 In both CPVT1 and CPVT2, the mutations cause spontaneous SR Ca2+ release leading to intracellular Ca2+ overload, which in turn can generate delayed afterdepolarizations (DADs). If these spontaneous oscillatory depolarizations reach the activation threshold, triggered arrhythmia occur, and can culminate into lethal ventricular fibrillation.6 High intracellular Ca2+ level which may result in triggered activity is triggered by one of two mechanisms:
-
RYR2 mutations resulting in a gain-of-function cause increased Ca2+ sensitivity of RYR2, and thus leads to increased probability and duration of the open state of ryanodine receptor channel, which in turn leads to SR Ca2+ leak.
-
CASQ2 mutations decrease the binding efficiency of CASQ2 to SR Ca2+, thus leading to SR Ca2+ leak from to the cytoplasm.1,8,16-20
There are two mechanisms by which high intracellular Ca2+ levels are reduced: (1) sarcoplasmic endoplasmic reticulum calcium (SERCA) pumps Ca2+ back into the SR. (2) Activation of sodium–calcium exchanger (NCX) that extrudes Ca2+ to the extracellular space and generates a net inward current (so called transient inward current) leading to membrane depolarization and DADs.
Modeling CPVT in a Dish with Induced Pluripotent Stem Cells (iPSCs)
Despite tremendously high mortality rate in CPVT patients (about 35%) the mechanisms of action are not completely clear and the current treatments are limited. Regardless of their mutation, CPVT patients are treated with insufficient efficiency, mostly with β-blockers; hence, patients still experience life-threatening episodes which may require implantable cardioverter defibrillators (ICD).6,22,23 Therefore, research models for drug screening of new therapeutic agents are encouraged. The recent technology of iPSC offers an innovative approach to study the molecular mechanism of CPVT and to test specific drug targets.
Embryonic stem cells (ESC) derived from the inner cell mass of a blastocyst, are pluripotent stem cells carrying the ability of self-renewal and differentiation into each one of the three germ layers. In 2006, Yamanaka and Takahashi have discovered a series of essential embryonic genes (OCT4, SOX2, KLF4, c-MYC) that if introduced into a mature fully-differentiated somatic cell, reboot a reprogramming process resulting in the generation of iPSCs. Several research groups have exploited this emerged technology to generate iPSCs for the investigation of inherited diseases such as neurodegenerative, metabolic and cardiac syndromes.24,25 Particularly, in the field of inherited arrhythmias several groups5,6,33,39 have demonstrated the ability of mutated iPSC-CMs to recapitulate the clinical symptoms, and to serve as a superb in vitro cell model for testing effective antiarrhythmic drugs. Additionally, the iPSC technology has been successfully employed to investigate dilated cardiomyopathy,34,35 hypertrophic cardiomyopathy34,36,37 and other channelopathies such as long QT syndrome as well as CPVT.1,5,6,16,33,34,38-40
CPVT patient-specific iPSCs carry the ability of differentiating into cardiomyocytes while holding the patient's genome, including CPVT-linked mutation, thereby CPVT-iPSC-CMs express the disease phenotype in vitro at cellular levels.24-30 CPVT patients carry different mutations in RYR2 or in CASQ2 genes that lead to different impaired protein-activities while causing for resembling clinical phenotypes. Despite the resembling phenotype in CPVT patients, the involved mechanism in each patient requires unique treatment for each specific mutation. iPSC-CMs benefit as in vitro model for investigation of each mechanism and allows the patient-specific personalized drug screening.
This review paper aims to cover most of the published investigations in the field of iPSC-CMs associated with CVPT by shedding light on the known mechanisms of CPVT, and on the explored pharmacological modalities that are suitable for patients carrying various CPVT mutations.
Cell Origin and Reprogramming Method
Different methods have been employed by research groups for cell origin production and reprogramming. While most research groups have used fibroblasts for the infection of pluripotent markers in order to generate iPSCs, Binah’s group was the first to produce CPVT-iPSCs from patient’s hair keratinocytes. Whereas most (9/11) have harnessed Yamanaka’s 4 pluripotent factors: OCT4, SOX2, KLF4 and c-MYC or a reduced combination (OCT4, SOX2 and KLF4), Priori’s group has reprogrammed somatic cells using an altered factor-set: OCT4, SOX2, NANOG and LIN-28 as described before by Yu et al.41 Despite the different methods used for reprogramming, all groups reported that the CPVT iPSC-CM recapitulated the disease specific phenotype.
Cardiomyocytes Differentiation
To date, there are several known differentiation methods towards the cardiac linage. In the described scientific investigations 2 major methods can be found:
-
Embryoid body (EB) – spontaneous differentiation.
-
Differentiation on murine visceral endoderm-like cell line (END2).
The EB spontaneous differentiation method includes detachment of iPSCs colonies by Collagenase type IV and suspension growth for a period of 7 days prior to gelatin coated plating as described before;42 in contrast, differentiation with END2 cell line requires 3 weeks of co-culture before separation. There is a time difference for cardiac differentiation in each method affecting the cardiomyocytes maturity and thus may create electrophysiological variability. With respect to CPVT research, the new standard of cardiac directed differentiation method was not yet introduced. In the directed method, the differentiation is achieved either by small molecules modulating the activity of GSK-3β and Wnt signaling pathway or by inducible β-catenin shRNA.43 The directed differentiation does not only provide a more uniform cardiac population, but also affects the cardiomyocytes maturity. As shown before, iPSC-CMs have a more developed SR while achieved by directed compared to spontaneous differentiation;44,45 accordingly affecting age range selection for electrophysiological/EC-coupling experiments. It will be of great interest to observe CPVT results from iPSC-CMs differentiated by a directed method that is calibrated to generate mature and enriched cardiac population.
CPVT-iPSC-CMs Recapitulate Disease Specific Phenotypes
Several groups have explored CPVT phenotypes in patient-specific iPSC-CMs by the following commonly used electrophysiology and Ca+2-contraction imaging methods:
Action potential recordings, by whole cell patch clamp configuration, have shown that CPVT-iPSC-CMs present DADs, early afterdepolarizations (EADs – during phase 2,3), oscillatory prepotentials and triggered arrhythmia (TA). Arrhythmias have been catecholaminergic-linked and increased during exposure to isoproterenol (a β-adrenergic agonist). While in control-cells, isoproterenol had caused positive chronotropic effect; in CPVT-CMs, it led to negative chronotropic effect and to the appearance of DADs and TA (Fig. 1). 5,16,38,39,46 Most groups have reported on similar electrical features (Maximum diastolic potential, action potential amplitude and maximal rate of depolarization (dV/dtmax)) between CPVT-CMs and control-cells.5,6,16,39 DADs and TA have been also generated by exposure of CPVT-iPSC-CMs to forskolin (an adenylyl cyclase activator) and by the end of a pacing-train, immediately after the last pulse. Thapsigargin – SERCA inhibitor, which causes for depletion of intracellular Ca2+ stores, has reduced the appearance of DADs post pacing or during the exposure to forskolin. This phenomenon suggests for another involved mechanism in the generation of DADs: store-overload-induced Ca2+ release (SOICR). SOICR manifests the necessity to reach a certain threshold of the SR over-load for spontaneous release via RYR2 through depolarization-independent SR release.39 It was also demonstrated that DADs may prevent the next emerging action potential, thus decreasing the cardiomyocytes beating rate, or may reach action potential threshold and initiate triggered activity. In addition to DADs, oscillatory pre-potentials were observed during action potential recordings. Unlike DADs, oscillatory pre-potentials appear during late diastolic depolarization, last for longer period and its amplitude grow progressively until reaching the action potential threshold.5,47,48
Figure 1. Isoproterenol induced DADs in CPVT1 and CPVT2 iPSC-CM. Representative action potentials recordings from healthy control (A), CPVT1 (B) and CPVT2 (C) iPSC-CM before and after exposure to 1µM isoproterenol with 0.5 Hz external pacing. Red arrows indicate on isoproterenol-induced DADs in CPVT iPSC-CMs
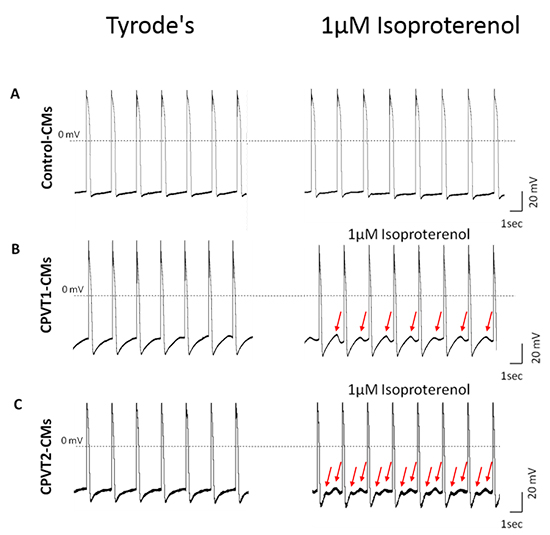
Calcium Handling Measurements
CICR mechanism is the key regulator of Ca2+ handling in cardiac muscle and is responsible for the EC coupling process. Researchers in this field measure Ca2+ transients either by Fura-2 or Flou-4; regardless the transient-recording method, all experiments have reported on a deranged Ca2+ handling machinery seen in CPVT-iPSC-CMs: multiple peaks, oscillations, varying amplitude and local Ca2+ release events interspersed within beats.1,5,38,46 Abnormalities have been manifested in base line of CPVT-iPSC-CMs Ca2+ measurements, and increased in response to adrenergic stimulation, such as isoproterenol exposure. Ca2+ handling abnormalities may cause arrhythmias, expressed as electrophysiological abnormalities such as DADs, EADs or oscillatory prepotentials that eventually lead to dissimilar beat-to-beat intervals and TA; these electrophysiological abnormalities are mirrored and explained by Ca2+ and contraction measurements.34 It was also indicated that Ca2+ handling abnormalities increase in exposure to isoproterenol or forskolin and could be reversed by addition of a beta-blocker (propranolol or metoprolol).5,39,46 Studies have shown that in caffeine-induced calcium release experiments, mutated cells had lower SR Ca2+ load in base line and during adrenergic stimulation; these results represent the enhanced average open period of mutated RYR2.16,38,40,46 Specifically in CPVT2, CASQ2-mutated cells exhibit marked diastolic [Ca2+]i rise in response to adrenergic stimulation, likely to be due to decreased binding efficiency of Ca2+ by CASQ2.5 Screening for antiarrhythmic treatments in CPVT-iPSC-CMs could be well studied by combining Ca2+ transient measurement, contraction and electrophysiological investigation.
Antiarrhythmic Pharmacological Candidates for CPVT Treatment
Studies suggested different antiarrhythmic agents for CPVT treatment, depending on the specific point mutations in RYR2 or CASQ2 and on its location. RYR2 is comprised of more than 100 exons and contains about 5000 amino acids, leading to a variety of mutations that can be found in this gene, including point mutations and deletions with varying locations from the C-terminal to the N-terminal of ryanodine receptor. It is clearly understood that mutations in different locations have dissimilar effects on protein dysfunction, resulting in the necessity of different agents to interact with different parts of RYR2 in order to compensate for function loss. The emerging field of personalized medicine acknowledges the importance of patient-specific drug screening and could be thoroughly employed using iPSC-CMs as in vitro model, as demonstrated in Fig. 2. Some progress has been done with few drug candidates linked to specific RYR2 mutations, as proof of concept, presenting the feasibility of this approach.
Figure 2. Representation of the personalized medicine concept in CPVT investigation. The process begins with obtaining skin or hair follicles biopsy from patient followed by reprograming procedure to generate iPSC cell-line holding the ability of differentiating into functional cardiomyocytes. To evaluate the effect of different anti-arrhythmic drugs on patient specific iPSC-CMs the scheme continues with electrophysiology and calcium-contraction study, involving external β-adrenergic stimulation resulting in arrhythmia represented as DADs. Subsequently the model allows the assessment of different anti-arrhythmic drugs for elimination of in vitro arrhythmias. Prominent agents should be tested for their effect within the patient
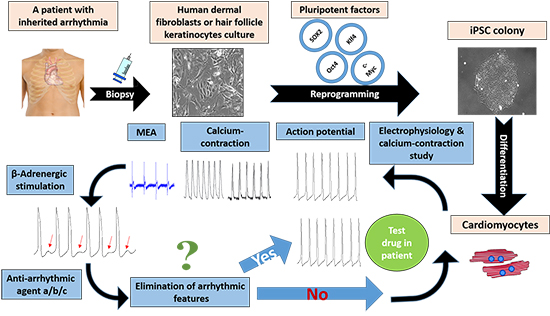
Dantrolene, a muscle relaxant is used as a treatment for malignant hyperthermia, caused by skeletal ryanodine receptor (RYR1) mutations.49 Datrolene stabilizes the closed state of RYR1 and hence its therapeutic effect; it has also been demonstrated to interact with RYR2.50 In order to explore its therapeutic effects on CPVT phenotype caused by RYR2 mutation, researchers have generated iPSC-CMs from CPVT1 patient with an autosomal dominant missense RYR2 mutation: S406L. RYR2 dislocation due to its mutation has been excluded by comparing immunefluorescent stainings of CPVT1 and healthy control iPSC-CMs. As expected, increased diastolic Ca2+ levels have been induced by isoproterenol in CPVT-iPSC-CMs, but not in control cells. Furthermore, SR Ca2+ load has been increased in response to isoproterenol in control iPSC-CMs, but not in mutated iPSC-CMs. The investigators have concluded that during chatecholamine stimulation, the increased luminal Ca2+ caused by S406L mutation is due to diastolic Ca2+ leak from the SR. It has been proposed that S406L increases Ca2+ sensitivity of RYR2 and produces diastolic spontaneous activity due to a lower threshold. Ca2+ leak by hyperactive RYR2 under catecholaminergic stress elevated diastolic Ca2+ and decreased SR Ca2+ load in CPVT-iPSC-CMs. Diastolic Ca2+ leak can generate arrhythmia by NCX activation, causing for depolarizing currents, represented as DADs.51 DADs and TA have been observed in 89% of mutated cells in comparison to 34% in control cells. Stress-induced diastolic Ca2+ leak from the SR via RYR2 could be explained by one of 2 mechanisms:
-
RYR2 mutations destroy essential inter-domain interactions that stabilize the closed state.52,53
-
RYR2 mutations abolish significant interactions with its modulating proteins.
It has been shown that S406L mutation is located in an inter-domain position, hence the validity of the first mechanism for this RYR2 mutation. Binding of dantrolene to the N-terminal end of skeletal and cardiac RYRs has restored normal Ca2+ handling in CPVT-iPSC-CMs during basal and chatecholamine-stimulation conditions. Furthermore, dantrolene has eliminated the appearance of DADs and TA, and has reestablished the wild-type phenotype, supporting the hypothesis that abnormal inter domain interactions are involved in this RYR2 mutation. Dantrolene has been proved as effective for S406L mutation; probably by restoring essential inter domain interactions within RYR2. To determine its effect on different mutations, the process should be repeated for each unique mutation. In a clinical study for dantrolene-treatment in CPVT1 patients, it markedly reduced arrhythmias in a subgroup of patients, depending on the mutation site within the RYR2 protein.1 Dantrolene has antiarrhythmic effect only on patients with mutations in the N-terminal or in the central region of the protein; however, it has no antiarrhythmic effect on CPVT-iPSC-CMs with mutations in the trans-membrane region. The researchers disclaimed that exceptional cases have been observed and that the antiarrhythmic effect of dantrolene could not be well determined by the mutation location solely, illustrating the significance of patient-specific drug screening model for CPVT.1 Furthermore, the results of this research on human subjects, alongside with patient-specific iPSC-CMs, indicate on similar dantrolene effect both in the clinical setting and in the corresponding in vitro model; these findings support the feasibility of in vitro drug screening while avoiding unnecessary side effects in the patient. Dantrolene binding site is a part of the domain switch region, implying for the involved mechanism in restoring defective unzipping and in stabilizing inter-domain interactions, eventually leading to inhibition of Ca2+ leak.1,5,14,38,54,55
Flecainide is categorized as class Ic antiarrhythmic drug and may contribute to the most common yet insufficient CPVT beta-blocker treatments. Its contributing effect originates, probably, from the reduction in the availability of membrane sodium channels and the increase of TA threshold16,38,56,57 or from the blockade of RYR2 in the SR membrane, which decreasing its opening probability.16,38,58-60 It eliminated DADs and TA in CPVT-iPSC-CMs.16
A side from commonly used β-blockers and the regarding in vitro studies (such as: metoprolol and bisoprolol), the development of new modalities and the patient-specific in vitro screening of existing antiarrhythmic drugs is encouraged before it could be introduced to a CPVT patient. VK-II-86, a synthetic analog of carvedilol, acts as β-blockers and had prevented stress-induced arrhythmia in CPVT mice model, yet has not been tested on human CPVT-iPSC-CMs.38
The inhibition of Ca2+/calmodulin-dependent serine–threonine protein kinase II (CaMKII), which phosphorylates main components of calcium handling machinery, has been shown to prevent β adrenergic-induced arrhythmias. KN-93 (2-[N- (2-hydroxyethyl)]-N-(4methoxybenzenesulfonyl)]-amino-N-(4-chlorocinnamyl)-N-methylbenzylamine), a CaMKII inhibitor has prevented arrhythmogenic features in CPVT-iPSC-CMs.6 It has eliminated isoproterenol-induced DADs and has restored normal calcium handling within cardiomyocytes. In 3D contracting EBs of CPVT-iPSC-CMs multiple sites have been observed for the initiation of calcium transients that, later on, have collided during propagation. KN-93 treatment has resulted in a single initiation site similarly to healthy control-iPSC-CMs.6
iPSC-CMs generated from CPVT patients recapitulate the disease specific phenotypes and by this, act as an applicable model for the investigation of key feature phenotypes as well as for the disease mechanism. The most promising ability of this model is with screening and developing of new modalities for patient specific personalized pharmacological treatments. We believe that in the following future, research of iPSC-CMs from CPVT patient, taking the advantages of this well-established model, will give new meaning for the bench to bed-side transition. Using patient specific iPSC-CMs the screening of existing alongside to newly developed pharmacological-agents will spare unnecessary exhausting and risky exploration within the patient’s body. The most prominent drugs to be screened are those previously proven effective in CPVT-mice models such as: ranolazine and propafenone.61 The currently most used therapeutic treatments including pharmacological β-blockers, implantable cardioverter-defibrillators (ICD) and left cardiac sympathetic denervation must be improved by the developing of new modalities in order to minimize the events of ICD-firing, resuscitation and mortality in CPVT patients.