Atrial Fibrillation Triggered By Drug-Induced Bradycardia
Gokhan Altunbas, MD, Suleyman Ercan, MD, Murat Sucu, MD, Vedat Davutoglu, MD
Gaziantep University Faculty of Medicine, Department of Cardiology.
Atrial fibrillation (AF) is the most frequently observed arrhythmia in clinical practice. Many causative factors have been identified from well-known structural heart disease to less understood triggers. Both sympathetic and parasympathetic (vagal) stimuli are able to trigger paroxysms of AF. Vagally mediated AF is especially observed in young healthy subjects and especially during nights when the heart rate is considerably slow. Tachycardia induced AF is demonstrated and the possible mechanisms are explained. However, a case of bradycardia induced AF, thus far, hasn’t been reported. Here we present a case of AF induced by severe bradycardia which was triggered by concomitant use of beta-blockers and diltiazem.
Key Words : Atrial Fibrillation, Bradycardia, Beta Blockers.
Correspondence to: Gokhan Altunbas, Gaziantep University Faculty of Medicine, Department of Cardiology, 27310 Gaziantep, Turkey.
Atrial fibrillation (AF) is the most common arrhythmia encountered in cardiology practice. AF is associated with increased risk of all-cause mortality (approximately twofold) and 4- to 5-fold increase in the risk of stroke.[1] Major risk factors for AF are mainly structural heart disease (hypertensive heart disease, ischemic heart disease, mitral valve disease, cardiomyopathies) and pulmonary hypertension. The most common reversible or temporary causes are hyperthyroidism, cardiothoracic surgery, acute myocardial infarction, myocarditis and pericarditis. AF is sometimes triggered by tachycardia. Especially AV nodal reentrant tachycardia and Wolff-Parkinson-White syndrome are reported to trigger AF. Here, we report an unusual case of bradycardia induced AF, which was triggered by concomitant use of carvedilol and diltiazem and converted to sinus rhythm by atropine.
A 70-year-old man admitted to cardiology clinic with complaints of dizziness and fatigue. Physical examination was normal except for bradyarrhythmic pulse and borderline hypotension; 90/60 mmHg. History revealed concomitant use of carvedilol 6.25 mg and diltiazem 120 mg per day. His prior electrocardiography (ECG) was within normal limits. The admission ECG showed atrial fibrillation with slow ventricular response with a pulse of 45/min (Figure 1). The patient was hospitalized for symptomatic bradycardia, monitorized and soon atropine 1 mg was given intravenously. The patient’s rhythm immediately converted to sinus rhythm with a pulse of 90/min and first-degree atrioventricular block (PR duration of approximately 240 ms) (Figure 2). The patient was monitorized for one day and sinus rhythm persisted. The next day he was discharged and outpatient follow-up visits confirmed the persistency of normal sinus rhythm.
Figure 1. Admission ECG showing atrial fibrillation with a slow ventricular response (heart rate approximately 45 beat per minute)
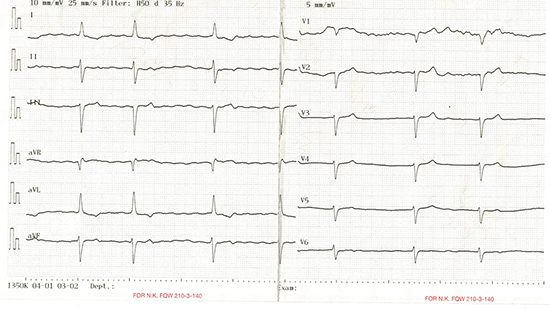
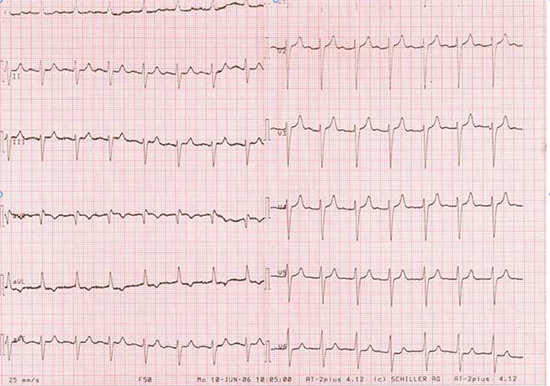
Figure 2. ECG obtained after administering intravenous atropine showing sinus rhythm with first-degree atrioventricular block
Atrial fibrillation is the most common arrhythmia and there are many reports indicating different triggers. Triggering and maintenance mechanisms may differ substantially. Along with well-known structural heart diseases, obesity and obstructive sleep apnea are independent risk factors for incident AF.[2] AF is sometimes triggered by tachycardias. First, the observation that elimination of atrioventricular nodal reentrant tachycardia (AVNRT) and atrioventricular reentrant tachycardia (AVRT) by radiofrequency catheter ablation also eliminates AF in many patients led to the conclusion that AF, at least in these patients, is triggered by tachycardia.[3] Since bradycardia induced AF, according to our search, has not been reported yet, its underlying mechanisms remain unclear. However, it is well known that vagally mediated AF exists in young healthy individuals especially during episodes of bradycardia (e.g. during sleep). Attacks usually start at night, lasts for a few hours and in the morning the rhythm usually converts to sinus rhythm.[4]
In our case, severe bradycardia associated with concomitant use of a beta-blocker with diltiazem can be considered to share common properties with vagally induced AF, which is also observed during episodes of bradycardia. Management is different from adrenergically mediated and other forms of AF. Beta-blockers and digoxin are especially harmful and must be avoided. In our patient, withdrawing the offending agents was enough for maintenance of normal sinus rhythm. Outpatient follow-up confirmed that the patient was on sinus rhythm and free of symptoms.