Which Factors Influence Resident Physicians to Prescribe NOACs to Patients with Non-Valvular Atrial Fibrillation?
Zardasht Oqab, MD FRCPC1, William F. McIntyre MD, FRCPC2,3, Wilma M. Hopman MA4, Adrian Baranchuk, MD FACC FRCP5
1Department of Cardiac Sciences, University of Calgary, Libin Cardiovascular Institute of Alberta, Calgary, Alberta, Canada.2Section of Cardiology, Department of Internal Medicine, University of Manitoba, Winnipeg, Manitoba, Canada.3Department of Medicine and Population Health Research Institute, Hamilton Health Sciences and McMaster University, Hamilton, Ontario, Canada.4Department of Public Health Sciences, Queen’s University.5Department of Medicine, Queen’s University, Kingston, Ontario, Canada.
The Canadian Cardiovascular Society and the European Society of Cardiology recommend the use of non-vitamin K antagonists (NOAC) in preference to warfarin for stroke prevention in most patients with non-valvular atrial fibrillation (AF). The aim of this study was to identify factors that predict selection of a NOAC by resident physicians when faced with patients with non-valvular AF. A web-based survey was distributed to residents across Canada to learn the attitudes and behaviours regarding stroke, bleeding risk and choices of therapy in different clinical scenarios involving the same patient and one additional co-morbidity. There were a total of 1014 respondents. In an uncomplicated patient with a new diagnosis of AF, self-reported comfort level was the strongest positive predictor for selecting a NOAC (odds ratio (OR) 2.51; 95% confident interval (CI) 1.79-3.54). Residents’ desire for the availability of a reversal agent was a negative predictor (OR 0.55; 95%CI 0.39-0.77). In a patient with a prior gastrointestinal bleed, each additional year of training was associated with a choosing a NOAC (OR 1.3; 95%CI 1.1-1.5). In the same patient, the desire for the availability of a reversal agent was a negative predictor of selecting a NOAC (OR 0.42; 95%CI 0.32-0.56). The most consistent predictor for prescribing a NOAC in all clinical scenarios was self-reported comfort level. Fear of adverse events, cost of agents and dosing convenience were not significant predictors. This study found that resident physicians’ adherence to guideline-preferred management of AF with regards to stroke prevention is strongly associated with self-reported comfort level, training year and the desire for the presence of a reversal agent.
Key Words : Atrial Fibrillation, Resident Physicians, Predictors, Warfarin, NOAC, Guideline Adherence.
Correspondence to: Zardasht Oqab, Adult Cardiology Resident, University of Calgary, Health Research and Innovation Centre, GAC 82-3280 Hospital Drive NW, Calgary, AB, Canada, T2N 4Z6.
Atrial fibrillation (AF) is the most common cardiac arrhythmia and is associated with an increased risk of stroke.1 In 2010, the global burden of patients with AF was 33.5 million, of which 20.9 million were men and 12.6 million women.2 These numbers are expected to rise due to aging population and longer life expectancies. Stroke prevention using oral anticoagulants (OAC) remains the cornerstone of AF management.
The Canadian Cardiovascular Society’s (CCS) Atrial Fibrillation guidelines recommend oral anticoagulation for all AF patients ≥65 years of age or who have any one of the traditional CHADS2 risk factors of stroke or transient ischemic attack, hypertension, congestive heart failure, or diabetes mellitus. When an OAC is indicated, it is recommended to use non-vitamin K antagonists (NOAC) including dabigatran, rivaroxaban, apixaban and edoxaban (when approved in Canada) in preference to warfarin.3 The use of NOACs in preference to warfarin in non-valvular AF is consistent with the European Society of Cardiology’s AF guidelines.4 The American College of Cardiology/American Heart Association AF guidelines do not give preference to NOACs over warfarin however do recommend to use a NOAC in patients with labile international normalized ratio (INR).5
Resident physicians frequently diagnose new AF or manage patients with known AF diagnosis. We have previously shown that resident physicians’, from different specialties and training years, choices for anticoagulation may not be congruent with guidelines due to presence of a knowledge gap and personal preferences.6-8 Not much is known about what the factors are that influence their decisions when choosing an anticoagulant agent. The aim of this study was to identify factors that predict selection of a NOAC by resident physicians when faced with patients with non-valvular AF.
We invited 1844 residents from 44 programs across 11 Canadian academic centers from internal medicine, family medicine, emergency medicine and adult cardiology to participate. A web-based survey consisting of 16 multiple choice questions was distributed using SurveyMonkey (Palo Alto, CA). The survey had different clinical scenarios involving the same patient: 76-year-old male with CHADS2 score of 3, and a medical history of congestive heart failure and hypertension. One additional characteristic was added to each subsequent scenario:
-
A history of gastrointestinal bleed 1-year prior during acetylsalicylic acid (ASA) treatment.
-
Stable stage 3 chronic kidney disease (eGFR 30-59 ml/min/1.73 m2).
-
Low risk intracranial hemorrhage 1-year prior and 4) a labile INR during warfarin treatment.
We looked at residents’ training year from PGY 1 though to PGY6 as a continuous variable. The number of prescriptions of OAC (either independently or with the help of an attending physician) in the preceding three months was coded as a 3-level variable of 0-5, 6-10 and greater than 11. Residents were also asked to rank from 1 (least important) to 5 (most important) characteristics related to anticoagulation such as availability of a reversal agent, fear of adverse events, cost to patient, personal familiarity with the agents and convenience of dosing to patients. These were subsequently coded as 0 (combining the three lower ratings of importance) and 1 (combining the two higher ratings) for inclusion in multivariable modelling. Comfort level was a self-reported measure with options of very comfortable, somewhat comfortable, neither, somewhat uncomfortable, very uncomfortable. To make it comparable to the characteristics of anticoagulation, this was also coded as 0 (the three lower ratings of comfort) and 1 (the two higher ratings) for the multivariable modeling.
The response options in the survey for the clinical scenarios were: no anticoagulation, ASA, warfarin, dabigatran, rivaroxaban, apixaban, and do not know. Scenario 5 omitted ASA as an option. Respondents were permitted to select multiple potential options based on their likings in each scenario. In this manner, there was no preference given to a specific therapy. The outcome variable was the selection of any one or more of the NOACs which was coded as 1=Yes and any other combination was coded 0=No for multivariable logistic modelling.
Data were collected within the SurveyMonkey Web site, exported in an Excel (Microsoft, Redmond, WA) format, and imported into IBM SPSS (version 22.0 for Windows, Armonk, NY) for statistical analysis. Following a descriptive analysis, a multivariate logistic regression was used to identify the demographics and values associated with selection of a guideline-preferred agent (i.e. NOAC). Since the number of variables to include in a model was not large, and the sample size was sufficiently robust, all potential covariates were entered into model rather than selecting them on the basis of a preliminary univariate analysis. This would allow us to see the respective contributions of each covariate while controlling for the others.
There were 33 programs that participated, constituting a total of 1014 respondents. This included 570 internal medicine, 247 family medicine, 137 emergency medicine, and 60 adult cardiology residents. The level of training ranged from PGY1 to PGY6. The response rate was 55% and the margin of error was 2.7% at a 95% confidence level (CI). For further demographic details of the participants and a full description of the survey and clinical scenarios referenced, see our previous publication and supplementary materials.6
For a patient with a new diagnosis of AF, self-reported comfort level was the strongest positive predictor of choosing a NOAC (odds ratio (OR) 2.51; 95% CI 1.79-3.54), followed by training level (OR 1.51; 95%CI 1.31-1.83) and familiarity with the agents (OR 1.51; 95%CI 1.03-2.17) (see Figure 1). Residents that ranked the desire for availability of a reversal agent highly were less likely to choose a NOAC (OR 0.55; 95%CI 0.39-0.77). In a patient with a history of a low risk gastrointestinal bleed while on ASA; both self-reported comfort level (OR 1.4; 95%CI 1.01-1.91) and each additional year of training level were associated with selecting a NOAC (OR 1.31; 95%CI 1.12-1.53). In the same scenario, residents that ranked the desire for availability of a reversal agent highly were less likely to choose a NOAC (OR 0.42; 95%CI 0.32-0.56).
Figure 1. Predictors of prescribing a NOAC in different clinical scenarios. Scenario 1 had a 76-year-old male with CHADS2 of 3 (history of congestive heart failure and hypertension) and new diagnosis of atrial fibrillation (AF). Each additional scenario, included same patient with one other co-morbidity. Scenario 2 added a history of low risk gastrointestinal bleed(GIB) while on ASA. Scenario 3 added a history of low risk intracranial hemorrhage (ICH). Scenario 4 added stable stage 3 CKD (eGFR 30-59 ml/min/1.73m2). Scenario 5 added a patient on warfarin with labile INRs
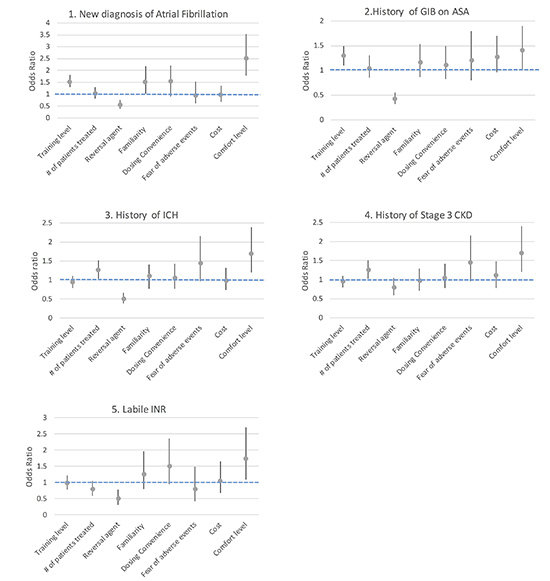
Scenario 3 involved a patient with a history of intracranial hemorrhage 1-year prior deemed low risk to re-bleed by a neurosurgical specialist. In this scenario, comfort level (OR 1.69; 95%CI 1.19-2.39) and number of patients treated over a 3-month period (OR 1.25; 95%CI 1.03-1.51) were associated with choosing a NOAC. Furthermore, residents that ranked the desire for availability of a reversal agent highly were less likely to choose a NOAC (OR 0.50; 95%CI 0.38-0.67). For a patient with stable stage 3 chronic kidney disease, comfort level (OR 1.69; 95%CI 1.21-2.44) and the number of prescriptions over a 3-month period (OR 1.24; 95%CI 1.03-1.48) were associated with selecting a NOAC. In a patient on warfarin with labile INRs, self-reported comfort level was the only positive predictor associated with picking NOACs (OR 1.71; 95%CI 1.08-2.74). The desire for availability of a reversal agent was a strong negative predictor (OR 0.48; 95%CI 0.31-0.77).
Our study looked at factors that resident physicians value when deciding on oral anticoagulation for their patients with atrial fibrillation. We found that self-reported comfort level with anticoagulation is the most consistent predictor in choosing a guideline preferred OAC across all training years, residency types and clinical scenarios. This study is, to the best of our knowledge, the first of its kind to explore this contemporary topic.
Although resident physicians frequently provide care to patients with AF either independently or with the help of attending physicians, the factors influencing their decisions maybe different. A prior study found that attending physicians are less likely to prescribe anticoagulants if any of their patients have experienced serious bleeding. Interestingly, the same physician survey also found that physicians were more likely to feel ‘responsible’ for a stroke occurring while not on OAC than a hemorrhage occurring while on OAC.9 In our study, the fear of adverse events was not a significant predictor of choice of agent in any of the clinical scenarios. This could be due to residents’ inexperience of seeing bleeding complications in their patients resulting from a lack of continuity of care during residency training. It can also be due to accumulation of knowledge playing a role in changing attending physician values and preferences over time. Our findings are in contrast to a recent study involving attending physicians that found the risk of major bleeding to be the most important attribute when prescribing OAC. Interestingly in the same study, patients were also asked to rank their preferences and the risk of major bleeding was rated low, a finding that was consistent with the behavior of residents in our study.10
Lack of reversal agents for the NOACs remains one of the major barriers to their use.11 We found that the residents who ranked the desire for a reversal agent highly were about 50% less likely to choose a guideline-preferred OAC in all clinical scenarios except the patient with stable stage 3 chronic kidney disease in which it was not a significant factor. There are now many studies and meta-analyses showing NOACs having a favourable risk-benefit profile compared with warfarin, with a significant reduction in rates of stroke, intracranial hemorrhage, mortality and with a major bleeding risk profile similar to warfarin.12-15 In our prior study, we found that about two thirds of resident physicians would switch from warfarin to a NOAC should a reversal agent became available.6 This finding is in contrast to survey assessing attending physicians’ factors that found presence of an antidote to be a less important attribute when prescribing OAC.10 Interestingly, our findings are more congruent with patient preferences in that study, as they rated the availability of an antidote as an important attribute.10 Idarucizumab, a monoclonal antibody fragment, was recently approved in the United States for the reversal of direct thrombin inhibitor dabigatran.16 Idarucizumab completely reverses the anticoagulant effect of dabigatran within minutes. Reversal agents for factor Xa inhibitors are currently in various stages of development.17 Nevertheless, it is not yet known whether reversing the effects of NOACs will change patient’s morbidity or mortality. What becomes clear from this analysis is that the existence of a reversal agent increases the level of guideline-preferred practices amongst the residents.
Another interesting and paradoxical finding of this study was that although the desire for the presence of a reversal agent was a strong negative predictor of choosing a NOAC, the fear of adverse events was not. This is in contrast to attendings’ who had the opposite preference in that they valued adverse events much higher than the presence of an antidote.10 This may be due to resident’s misunderstanding the value of reversal and patient outcomes.
Although, the Canadian Cardiovascular Society recommends the use of NOACs in preference to warfarin for stroke prevention in AF, the adoption of these drugs have not been uniformly accepted and this may be, in part, due to a lack of alignment with reimbursement systems.18 Valuing cost consideration was not a significant predictor in any of the clinical scenarios which may reflect the general prescribing patterns of OACs in Canada. As indications for the use of NOACs expand, which now include venous thromboembolism and pulmonary embolisms, more provinces may adopt reimbursement plans that can lead to wider adoption of NOACs.19
Some limitations of our study are worth mentioning. First, our findings are subject to limitations with survey-based designs. Although this was a good method to assess the choices of anticoagulation of a large number of residents, we cannot tell the extent to which the self-report is related to what is done in practice. Second, resident physician roles and responsibilities vary between residency programs and centers and it is unclear the extent of the influence attending physicians have on junior residents’ decisions. However, our findings were consistent uniformly across all training years. It would also be interesting to see how the factors influencing resident decisions may change if other co-morbidities that were barriers to anticoagulation by attending physicians were added to the clinical scenarios such as cognitive impairment, frequent falls and poor patient adherence.20
Factors that increase the likelihood that Canadian residents will select a non-vitamin K oral anti-coagulant for a patient with non-valvular atrial fibrillation have been identified.
-
Self-reported comfort level with oral anticoagulants is the most significant predictor across all patient scenarios.
-
Each additional year of training led to an increased likelihood of prescribing a NOAC.
-
Desire for the presence of a reversal agent was generally a strong negative predictor of choosing a NOAC.
Dr. Baranchuk reports personal fees from Bayer Health Care Canada, Boehringer Ingelheim (Canada) LTD and Pfizer Canada Inc, outside the submitted work. Dr. McIntyre has received salary support from the McMaster Cooper Fellowship and the Canadian Stroke Prevention Intervention Network (C-SPIN) Fellowship.