Giant Left Atrial Appendage Aneurysm Mimicking Mediastinal Mass and Associated with Incessant Atrial Arrhythmias
Joëlle Morin, Luce Cantin, Sergio Pasian, François Philippon, Jonathan Beaudoin
Institut universitaire de cardiologie et de pneumologie de Québec, Quebec, Canada.
Left atrial appendage aneurysm (LAAA) is a rare entity. Clinical manifestations include arrhythmias and systemic embolization. We show here an example of a large and ectopic LAAA mimicking a mediastinal mass on chest X-ray and presenting with incessant atrial arrhythmias. Subsequent investigations leading to the correct diagnosis are described.
Key Words : Left atrial appendage, Atrial arrhythmias, Mediastinal Mass.
Correspondence to: Jonathan Beaudoin, MD Cardiology division, Institut universitaire de cardiologie et de pneumologie de Québec 2725, chemin Sainte-Foy, Québec (Quebec), Canada G1V 4G5 Phone: 1-418-656-8711 ; Fax: 1-418-656-4581 jonathan.beaudoin@criucpq.ulaval.ca
A 50-year-old man was transferred to our institution with a diagnosis of incessant supraventricular tachycardia (SVT) not responding to medical treatment. Past medical history included pericarditis at age 23 and paroxysmal atrial fibrillation (AF) at age 42. He described progressive shortness of breath over the preceding two months (NYHA class III/IV at presentation), orthopnea and paroxysmal nocturnal dyspnea. Physical exam revealed regular tachycardia, elevated central venous pressure and positive Kussmaul sign. Electrocardiogram showed regular SVT at 150 beats per minute [Figure 1]. Intravenous amiodarone was started, with subsequent return in sinus rhythm. The admission chest X-ray demonstrated a well-defined mediastinal enlargement at the aortopulmonary window [Figure 2], and was also notable for pericardial calcifications. Transthoracic echocardiogram was performed but limited due to poor echogenicity. There was mild biventricular dysfunction, without significant valvular disease.
Figure 1. Initial ECG showing narrow complex tachycardia. The visible P wave (long RP tachycardia) is suggestive of either a reciprocating tachycardia using a retrograde accessory pathway or an atrial tachycardia.
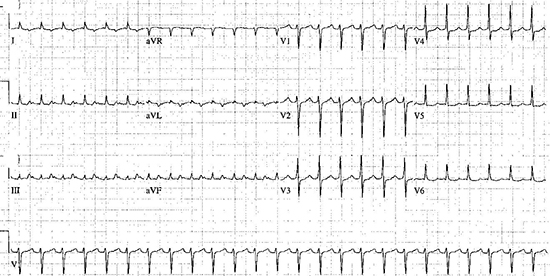
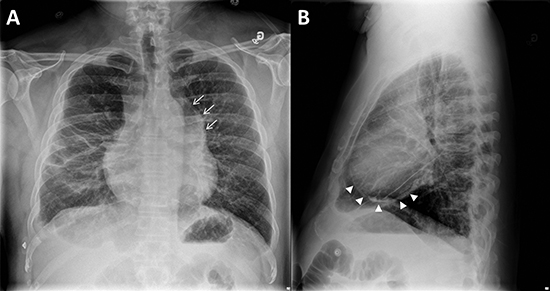
Figure 2. Chest X-Ray showing enlarged mediastinum at the aortopulmonary window due to left atrial appendage aneurysm LAAA (A, arrows), and curvilinear pericardial calcifications (B, arrow heads) inferiorly .
Chest CT scan was performed and showed a dilated left atrial appendage extending in the anterior mediastinum [Figure 3]. There were also important pericardial calcifications. A cardiac MRI demonstrated low normal left ventricular ejection fraction (53%). A giant and ectopic left atrial appendage aneurysm (LAAA) was confirmed, measuring 8 cm and travelling upward into the superior mediastinum, with suspected herniation through a partial pericardial agenesis [Figure 4] and Movie 1 and 2. No thrombus was seen.
Figure 3. Contrast-enhanced chest CT in sagittal (A), and coronal (B)maximum intensity projections (MIP) showing the left atrium and left atrial appendage aneurysm (arrows). Panel A also shows inferior pericardial calcifications. (C) 3D volume rendering reconstruction showing the LAAA in relation to other cardiac structures. Ao: aorta; PA: pulmonary artery.
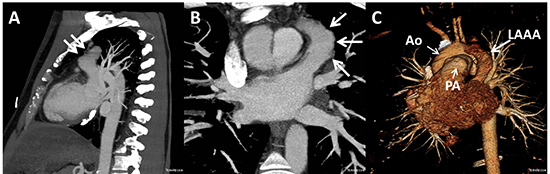
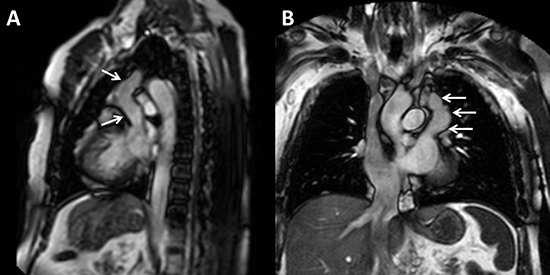
Figure 4. Cardiac MRI balanced steady-state free precession (b-SSFP) sequence in left two-chamber (A) and coronal (B) views showing the left atrial appendage aneurysm (arrows) extending upward in the anterior and superior mediastinum, causing the abnormal cardiac contour seen on chest x-ray.
Electrophysiological study showed an eccentric retrograde conduction demonstrated with isoproterenol infusion, but only non-sustained tachycardia was induced. A left anterolateral concealed accessory pathway with poor conduction capacity was suspected, for which catheter ablation was performed through a retrograde approach. Despite early success from the ablation procedure, early recurrence of SVT mandated the resumption of antiarrhythmic drugs (flecainide and diltiazem) with subsequent good control and the patient was discharged home 3 days later. Follow-up visits are planned before considering a second ablation procedure by transseptal approach if required.
LAAA is a rare entity. It can be congenital or acquired, usually as a consequence of mitral valve disease with elevated intra-atrial pressure. Congenital LAAA can be intrapericardial or extrapericardial when the left appendage herniates through a congenital defect of the pericardium. In most cases, only surgery or autopsy can confirm the integrity of the pericardium. In our case, suspected herniation through a partial pericardial agenesis is supported by the extra-anatomical location of the LAAA in the superior mediastinum. The reported clinical LAAA manifestations are systemic embolization (18%) and supraventricular arrhythmias (60%)[1]. Surgical resection of the LAAA is usually the preferred treatment, as it eradicates the potential embolic source as well as most atrial arrhythmias. Some authors favor surgery even in asymptomatic patients to prevent the potentially morbid and fatal complications associated with AF and systemic embolization[2]. Surgery was not performed in the current case since electrophysiological study has identified another mechanism for the atrial arrhythmias, which were subsequently controlled with antiarrhythmic drugs.