Prognostic Value of Atrial Fibrillation Inducibility in Patients Without History of Clinical Atrial Fibrillation
Jonathan Marquardt1, Kira Marquardt1, Christian Scheckenbach2, Wenzhong Zhang3, Fabian Stimpfle1, Martin Duckheim1, Carole Maleck1, Peter Seizer1, Meinrad Gawaz1, Jürgen Schreieck1, Michael Gramlich1
1Department of Cardiology and Cardiovascular Diseases, Eberhard Karls University, Tübingen, Germany.2Department of Paediatric Cardiology, Pulmology and Paediatric Intensive Care Medicine, University Children's Hospital, Tübingen, Germany.3Department of Cardiology, Affiliated Hospital of Qingdao University, Qingdao, Shandong 266003, China.
During invasive electrophysiological studies (EPS), atrial fibrillation (AF) can be induced in patients without a history of AF. However, the prognostic value is not well evaluated in this population. Our aim was to investigate whether AF inducibility in those patients is associated with future clinical episodes of AF; whether non-inducibility is predictive of freedom from new-onset AF and finally, to examine clinical factors associated with inducibility.
Medical records from patients undergoing EPS between the years 2011 and 2014 were analysed retrospectively with 62 patients matching our inclusion criteria. Patients were divided into subgroups according to their inducibility status and underwent follow-up. Patients were assessed by a structured telephone interview, data from the further treating physicians and ECG recordings.
AF was inducible in 19 patients („induction group“) and not inducible in the remaining 43 („control group“). Inducibility was associated with a higher age (p=0.002), lower GFR (p=0.002), higher CHAD2S2-VASc score (p=0.004) and diagnosis of mitral (p=0.014), tricuspid (p=0.017) and pulmonary (p=0.026) valve insufficiency. Three months after EPS, 89.5% of all inducible patients were free of diagnosed AF, in contrast to 100% of those without inducibility (p=0.031). At three years, no significant difference was left (p=0.162).
AF inducibility was found more often in an older population with cardiac comorbidities. While inducibility was associated with an increased rate of diagnosed new-onset clinical AF in the months after testing, non-inducibility seemed to be associated with freedom from AF at least in the short to medium term. However, there was no significant difference in the long term follow-up.
Key Words : Atrial Fibrillation, Inducibility, Follow-up, Prognostic Value.
Correspondence to: Dr. Michael Gramlich, Department of Cardiology and Cardiovascular Diseases, Eberhard Karls University, Otfried-Müller-Str.10, 72076 Tübingen, Germany
Within the last decade, the burden of atrial fibrillation (AF) has almost doubled in Europe, affecting between 1.9% and 2.9% of the general population and, according to estimates, more than 33.5 million people worldwide in the year 2010[1,2]. Data derived from the Framingham Heart Study even suggest a lifetime risk of 1 in 6 patients without structural heart disease for the development of atrial fibrillation or atrial flutter[3]. Undetected and –treated, AF bears a significant risk for the development of tachycardiomyopathy and stroke[4],[5]. It is well established that prolonged episodes of atrial fibrillation can induce various pathways that stabilize and fuel the disease[6]. According to a widely accepted model, paroxysmal atrial fibrillation is thought to be the result of rapid triggering by ectopic foci or a single re-entry mechanism in the area around the pulmonary veins, while the more persistent or permanent forms are based on multiple functional or structural re-entry mechanisms, partly caused by remodelling processes provoked by the arrhythmia itself (i.e. altered ion channel functions that lead to a shortening of the atrial refractory time and thus to the further stabilization of the condition) and by structural remodelling of the atria with development of atrial fibrosis[5,7,8]. Those findings are reflected in current treatment guidelines, i.e. the use of RAS inhibitors and other medications for the prevention of further proliferation of proarrhythmogenic fibrotic tissue, also known as upstream therapy[9], as they have also sparked inventions in the field of interventional electrophysiology, with Haïssaguerre et al being the first to demonstrate that radio-frequency ablation of the tissue around the pulmonary veins could cure the disease at least in certain patients[10]. Yet, there is still a good deal of unsettled questions left, not only regarding different modes of therapy but also regarding novel strategies for the detection of atrial fibrillation. Identifying risk factors that predispose patients to develop AF might help to reduce subsequent disabilities.
During invasive electrophysiological studies (EPS), AF can be induced via high rate atrial burst pacing, sometimes also in patients without a history of the disease. However, the prognostic value of this test is largely unknown. In this study, we hypothesised that inducibility of AF during EPS is associated with a higher risk to develop clinical AF and that noninducibility is a valid predictor of freedom from new-onset atrial fibrillation.
Medical records from patients that underwent EPS from 2011 to 2014 at the University hospital of Tuebingen, Germany were screened for attempted AF induction by high rate atrial burst pacing and divided into two group according to their inducibility status. Indications for EPS (multiple nominations possible) in the final cohort were: suspected paroxysmal supraventricular or ventricular tachycardia (42.0%), risk stratification in patients with cardiomyopathy or reduced left ventricular ejection fraction (40.4%), unclear syncope (33.9%) and others (16.0%). Patients were excluded if a structured interview via telephone was not feasible. Other exclusion criteria were: previous episodes of AF, atrial flutter or atrial tachycardia; congenital heart defects with corrective surgery, history of valve surgery or other major heart operations; cryptogenic stroke; history of catheter ablation in the atria other than ablation due to AVRT/AVNRT; successful induction after the previous administration of a beta-adrenergic agent (i.e. Orciprenalin).
All patients were legally competent and gave their informed consent. The study was approved by the local ethics commission. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
As the study was designed retrospective, the setting and performance of the EPS was dependant on the indication that lead to the examination and also on the responsible physician. However, according to the operating protocol of the cardiological department of Tuebingen University Hospital, patients are usually called to stop their medication before undergoing EPS if treated with beta blocking agents or other drugs potentially interacting with the electrical vulnerability of the heart within at least 24-48 hours before testing. For AF induction, a decapolar CS catheter, spacing 2-5-2 mm, is then placed into the coronary vein sinus, the proximal pair positioned at the CS ostium enabling single site pacing. Burst stimulation is usually performed at double pacing threshold or at least 5 mA and 3 ms pulse width, 3 seconds per burst with a pause of 3000 ms between, starting from CL 300 ms and decrementing by 10 ms down to 200 ms or the shortest cycle length that resulted in a 1:1 atrial capture or until AF is induced within that range.
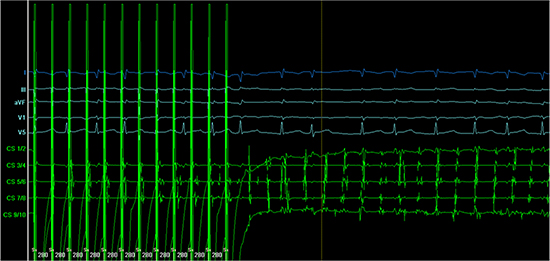
According to literature, fast and irregular atrial activation >2 seconds was defined as non-sustained AF and inducible episodes > 30 seconds as sustained AF[11,12]. Patients get cardioverted after more than 10 minutes of sustained AF. An example of successful AF induction is shown in [Figure 1].
Figure 1. Example of AF induction. High rate atrial burst (CL 280ms) pacing leads to atrial instability with a subsequent development of atrial fibrillation.
Patients were contacted and questioned in a structured telephone interview about their current health status, recent (cardiological) examinations or tests, newly diagnosed heart diseases with a special focus on heart rhythm disorders, newly started medications with a special focus on antiarrhythmic and anticoagulant drugs and about having experienced certain symptoms of TIA or stroke. The patients were briefed to consult a healthcare provider if experiencing symptoms pointing to arrhythmias and were asked for permission to contact the further treating physicians (primary care and private-practice cardiologists) later on for further information regarding their post-EPS state of health. If available, data from the emergency department, the cardiological outpatient department and inpatient ward that were gained in the meantime after EPS were also analysed. The mean follow-up time was 32.5 months in the induction group and 26.7 months in the control group, showing no statistically relevant difference (p = 0.134). 52.6% of the patients in the induction group and 48.8% of the patients in the control group received one or more examinations via Holter monitoring or ICD/ pacemaker/ event recorder interrogation and further 42.1% of the patients in the induction group and 37.2% in the control group had at least one (or more) 12 channel ECGs performed on them during the course of follow-up.
Statistical analysis was performed using the Chi-Squared test or the Fisher’s exact test. The categorical variables were treated as binary. For inter-group comparisons, testing for Gaussian distribution was performed using the Shapiro-Wilk test. Parametric data were then analysed using mean value, standard distribution, the Levene test and t-test, non-parametric data were analysed using the median value and the Mann-Whitney-U test. A Kaplan-Meier analysis was performed to estimate the AF-free survival rate in both groups, with a log-rank test used to test for possible statistically significant differences. Statistical significance was defined as p < 0.05.
Induction of Atrial Fibrillation During EPS
62 patients matched our inclusion criteria. Of those, 19 were defined as AF inducible (“induction group”, 18/19 respectively 94.7% with sustained AF, 1/19 with non-sustained AF) and 43 as AF non-inducible (“control group”). One member of the induction group died during the course of follow-up from a non-cardiac cause (cancer of unknown primary).
The clinical characteristics of our patient populations are given in [Table 1]. The induction group consisted of 8 male and 11 female patients (42.1% vs. 57.9%). In the control group, 28 patients were male and 15 were female (65.1% vs. 34.9%). The differences were not statistically significant (p=0.09). The members of the induction group were significantly older than their counterparts (median age 69 years vs. 48 years, p=0.002). No differences were observed in the patients’ body-mass indexes (induction group 27.7 kg/m² with SD 5.0 vs. control group 26.7 kg/m² with SD 6.2, p=0.541).
Table 1. Baseline data and clinical assessment stratified by inducibility status.
|
Positive AF Inducibility |
Negative AF Inducibility |
P-value |
| Sex |
|
|
|
| Total Number |
19 |
43 |
|
| Male |
42.1% (8/19) |
65.1% (28/43) |
p=0.090 |
| Female |
57.9% (11/19) |
34.9% (15/43) |
|
| Age |
|
|
|
| Median Age (years) |
69 |
48 |
p=0.002 |
| Interval 1 (< 29 years) |
0.0% (0/ 19) |
27.9% (12/43) |
|
| Interval 2 (30-59 years) |
31.6% (6/ 19) |
53.5% (23/43) |
|
| Interval 3 (60-99 years) |
68.4% (13/19) |
18.6% (8/43) |
|
| Body-Mass Index |
|
|
|
| BMI Mean Value (in kg/m²) |
27.7 |
26.7 |
p=0.541 |
| Standard Deviation |
5.0 |
6.2 |
|
| Cardiovascular Risk Factors |
|
|
|
| Hypertension |
63.2% (12/19) |
39.5% (17/43) |
p=0.086 |
| Dyslipidemia |
47.4% (9/19) |
23.3% (10/43) |
p=0.058 |
| Nicotine Abuse |
26.3% (5/19) |
14.0% (6/43) |
p=0.288 |
| Diabetes Mellitus |
15.8% (3/19) |
11.6% (5/43) |
p=0.692 |
| Fam. Predisposition |
31.6% (6/19) |
18.6% (8/43) |
p=0.327 |
| Median Count |
2 |
1 |
p=0.054 |
| Comorbidities |
|
|
|
| CAD |
42.1% (8/19) |
23.3% (10/43) |
p=0.132 |
| CMP |
10.5% (2/19) |
23.3% (10/43) |
p=0.313 |
| LBBB |
21.1% (4/19) |
11.6% (5/43) |
p=0.437 |
| Myocarditis |
5.3% (1/19) |
7.0% (3/43) |
p=1.000 |
| Myocardial Infarction |
15.8% (3/19) |
14.0% (6/43) |
p=1.000 |
| SVT |
21.1% (4/19) |
14.0% (6/43) |
p=0.479 |
| VT |
10.5% (2/19) |
16.3% (7/43) |
p=0.709 |
| Syncope |
42.1% (8/19) |
37.2% (16/43) |
p=0.715 |
| Hyperthyreoid Disorder |
21.1% (4/19) |
7.0% (3/43) |
p=0.187 |
| Hypothyreoid Disorder |
10.5% (2/19) |
7.0% (3/43) |
p=0.638 |
| Renal Insufficiency |
0.0% (0/19) |
4.7% (2/43) |
p=1.000 |
| Depression |
10.5% (2/19) |
4.7% (2/43) |
p=0.580 |
| Sleep Apnoea Syndrom |
5.3% (1/19) |
2.3% (1/43) |
p=0.522 |
| Laboratory Results |
|
|
|
| Potassium Mean Value (in mmol/l) |
4.2 (SD 0.4) |
4.3 (SD 0,4) |
p=0.456 |
| GFR Mean Value (in ml/min/1,73m²) |
80.0 (SD 14.0) |
101.0 (SD 25.0) |
p=0.002 |
| Creatinine Median (in mg/dl) |
0.9 |
0.8 |
p=0.346 |
| TSH Median (in mU/l) |
1.2 |
1.4 |
p=0.768 |
| Echocardiographic Data |
|
|
|
| Median LVEF |
60.0% |
60.0% |
p=0.684 |
| ED Mean Value (in mm) |
48.3 |
52.0 |
p=0.324 |
| Standard Deviation |
9.5 |
9.2 |
|
| ES Median (in mm) |
35.0 |
32.5 |
p=0.603 |
| Septal Thickness Median (in mm) |
12.0 |
12.0 |
p=0.921 |
| Atrium Parasternal Mean Range (in mm) |
37.9 |
39.1 |
p=0.649 |
| Standard Deviation |
6.1 |
6.8 |
|
| Atrium Apical Mean Range (in mm) |
20.7 |
20.8 |
p=0.977 |
| Standard Deviation |
6.1 |
5.6 |
|
| Mitral Insufficiency |
69.2% (9/13) |
24.1% (7/29) |
p=0.014 |
| Aortic Insufficiency |
33.3% (4/12) |
13.3% (4/30) |
p=0.195 |
| Pulmonary Insufficiency |
50.0% (4/8) |
8.7% (2/23) |
p=0.026 |
| Tricuspid Insufficiency |
75.0% (9/12) |
32.3% (10/31) |
p=0.017 |
| CHAD2S2-VASc Score |
|
|
|
| CHAD2S2-VASc Score Median |
2 |
1 |
p=0.004 |
| CHAD2S2-VASc 0 |
10.5% (2/19) |
41.9% (18/43) |
|
| CHAD2S2-VASc 1 |
10.5% (2/19) |
16.3% (7/43) |
|
| CHAD2S2-VASc >=2 |
78.9% (15/19) |
41.9% (18/43) |
|
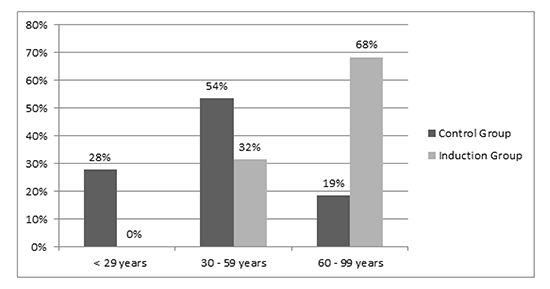
Remarkably, atrial fibrillation was not inducible in any patient younger than 30 years. The age distribution in each group is demonstrated in [Figure 2].
Figure 2. Age distribution stratified by inducibility status and age intervals.
Clinical Assessment - Risk Factors, Comorbidities, Laboratory Results and Echocardiographic Data
No statistically significant differences between both groups were found regarding the documented patients’ cardiac risk factors (hypertension, dyslipidemia, nicotine abuse, diabetes mellitus and familiar predisposition) and the pre-diagnosed cardiac and medical comorbidities in the study population (CAD, cardiomyopathy, left bundle branch block, myocarditis, myocardial infarction, supraventricular or ventricular tachycardia, syncope, thyroid disorders, renal insufficiency, depression and sleep apnoea) at the time of EPS. Although the glomerular filtration rate (MDRD – GFR) was significantly lower in in the induction group (mean value 80.0 ml/min/1.73m² vs. 101.0 ml/min/1.73m², p=0.002), there was no significant difference regarding the patients’ potassium, creatinine and TSH levels. However, statistical significance was found regarding mitral, tricuspid and pulmonary valve insufficiencies of any degree. Mitral valve insufficiency was found to be present in 69.2% of the induction group and in 24.1% of the control group (p=0.014), tricuspid valve insufficiency was found in 75.0% of the induction group vs. 32.3% of the control group (p=0.017) and pulmonary valve insufficiency was found in 50.0% of the induction group and in 8.7% of the control group (p=0.026). There were no significant differences between groups concerning aortic valve insufficiency, left ventricular ejection fraction, atrial diameters and septal thickness. Finally, there was also a significant difference between the median CHAD2S2-VASc scores, with the median score of 2 in the induction group and a score of 1 in the control group (p=0.04). A detailed summary can be found in [Table 1].
Development of Atrial Fibrillation During the Course of Follow-up
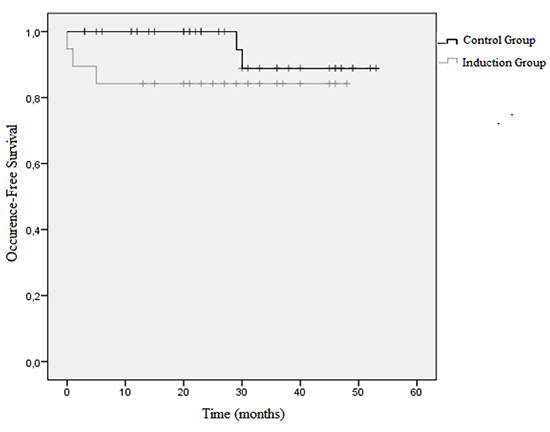
Surprisingly, only 5 out of 62 patients were diagnosed with newly onset atrial fibrillation during the total course of follow-up (2 patients with EPS-induced sustained AF, 1 patient with EPS-induced non-sustained AF, 2 patients without previously inducible AF). No single patient experienced symptoms pointing to stroke or TIA. After 3 months, 89.5% (17/19) of the patients with positive AF inducibility were free of atrial fibrillation in contrast to 100% (43/43) of those with a negative inducibility status (p=0.031). At 3 years, the Kaplan-Meier analysis estimated an event-free survival rate of 84.2% in the induction group and 88.9% in the control group, clearly missing statistical significance (p=0.162, [Figure 2]).
Our results show that AF inducibility in patients without a history of AF is more likely in an older population as well as in those patients who have a lower glomerular filtration rate, who suffer of mitral, tricuspid an pulmonary valve insufficiencies of any degree and finally in patients who have a CHAD2S2-VASc score of 2 or more. Furthermore, the study suggests that patients with a positive AF inducibility status are more often diagnosed with symptomatic atrial fibrillation within the first months after EPS, while those with a negative inducibility seemed to remain free of new-onset atrial fibrillation for up to 2.5 years after testing. The loss of a statistically significant difference between both groups in the long term could possibly be explained by a temporarily limited value of the results generated by electrophysiological testing, since all patients who were affected in the induction group developed atrial fibrillation within a very short time after being tested (up to 5 months), while the individuals of the control group who developed AF showed the first episodes more than 2.5 years after their EPS. We hypothesize that this could be explained by a gradual development of pathways capable of supporting AF in those patients who were initially non-inducible, possibly due to the lack of such pathways or fibrotic tissue, but were affected by remodelling processes in the meantime. Interestingly, in patients with positive inducibility, the duration of EPS-induced atrial fibrillation (non-sustained AF vs. sustained AF) respectively the time to conversion back to sinus rhythm was not necessarily associated with outcome. Studies with more participants are needed to evaluate whether there are other distinctive clinical features that are shared by those patients with a positive inducibility status and a subsequent development of symptomatic atrial fibrillation but are non-existent in those with a previous positive inducibility and ongoing freedom from the disease.
This study is also the first to our knowledge investigating the prognostic value of AF inducibility in a representative sample of cardiovascular patients, including also the chronically ill and those with structural heart disease, yet featuring only patients without pre-diagnosed atrial fibrillation and atrial flutter at the time of undergoing EPS, as previous studies were conducted to evaluate either whether the inducibility status following pulmonary vein isolation or isthmus ablation was predictive of the outcome (meaning that most patients were already diagnosed with atrial fibrillation in the first place) or included only overall healthy patients without structural heart disease. Essebag et al were amongst that first group and demonstrated in that context, that 82% of all patients with a negative inducibility via atrial burst stimulation (with or without the administration of isoproterenol) immediately after pulmonary vein isolation were free of atrial fibrillation 6 months later, in contrast to only 59% of patients with a positive inducibility status (72% vs 53% after 12 months) [13]. Haïssaguerre et al compared the efficiency of pulmonary vein isolation and linear ablation and additionally if noninducibility afterwards was a predictive factor. After 7±3 months, reoccurrence of arrhythmia was detected in 38% of the inducible and in 13% of the noninducible patients, showing statistical significance[14]. Oral et al also performed left atrial radiofrequency circumferential PV ablation with additional ablation lines in the posterior left atrium and the mitral isthmus and tested the inducibility status afterwards, with patients with a positive inducibility despite the preceding procedure undergoing either further catheter ablation (left anterior septum/ roof/ anterior wall, guided by fractionated electrograms) or no therapy. Of those patients who were noninducible after the initial procedure or underwent further ablation because of a positive inducibility, 85% were free of atrial fibrillation at the point of 6 months, compared to 67% of those who still had spontaneous or inducible episodes of atrial fibrillation[15].
In contrast, Kumar et al were amongst the second group and investigated the inducibility of atrial fibrillation in 44 mainly healthy patients without pre-known AF, yet also without structural heart disease. Induction was performed via high rate atrial pacing/ decremental pacing, with 10 successive repetitions in each patient, provoking atrial fibrillation of at least 1 minute duration in 49.5% of all patients and of more than 5 minutes in 29.5%, with the risk increasing with each repetition. In their study, neither was EPS-induced atrial fibrillation (sustained more than 5 minutes) linked to any clinical feature (besides male gender), nor did a single patient develop clinical episodes of atrial fibrillation or any other tachycardia affecting the atrium during a median follow-up time of 23 months, though the exact modalities of follow-up were not explicitly listed[16]. Joza et al published a study regarding the prognostic value of AF induction in patients who underwent right atrial flutter ablation before. Around the onset of follow-up, a subgroup of 93 patients was without a history of atrial fibrillation (yet still with a history of atrial flutter). Burst stimulation was performed over 5 seconds at first from the anterolateral right atrium and subsequently from the coronary sinus, with positive inducibility defined as sustained atrial fibrillation over the course of 30 seconds. 20 patients were counted as inducible, 73 as not inducible. During the course of follow-up, 14 out of 20 patients with positive inducibility developed atrial fibrillation in contrast to 5 out of 73 with negative inducibility (crude Hazard Ratio = 13.74)[17]. Finally, Leong-Sit et al investigated the prognostic value of the induction of atrial fibrillation and atrial flutter after pulmonary vein isolation as well, but focused also on factors associated with positive inducibility. During their follow-up, 49.1% of the patients with negative inducibility and 49.4% of those with positive inducibility had a relapse, contradicting the quintessence of the majority of other studies conducted regarding this topic and clearly missing statistical significance. Positive inducibility was in consistence with our results significantly associated with age (per decade, OR 2.10). A history of hypertension (OR 4.15) was also identified as a positive predictor, whereas diabetes mellitus was a negative predictor of inducibility (OR 0.06), probably being caused by a type I error according to the authors[18].
Since our study was conducted retrospectively, it is subject to the characteristic corresponding disadvantages. With only about half of the members of both groups receiving Holter ECGs or interrogations of ICDs/ pacemakers/ event recorders and most of the remaining patients only routine 12 channel ECGs, patients could have been left undiagnosed, as the study design enabled only the reliable detection of persistent or symptomatic atrial fibrillation in contrast to the currently intensely debated asymptomatic paroxysmal atrial fibrillation, though on the other hand the significance of asymptomatic atrial fibrillation is still not ultimately ascertained[19]. In addition, since a positive inducibility status was associated with a higher age and certain comorbidities, it is possibile that AF inducibility during EPS is not an independent predictor, but merely a marker for older patients or such with a degrading health status, who then again are known to be at higher risk for developing atrial fibrillation subsequently. Further analysis addressing that issue was not feasible due to the small number of patients included. Due to this underpowering, a final statement regarding the prospective value of EPS-induced AF cannot be made at this point.
Another perhaps more fundamental problem in comparing various studies investigating the prognostic value of induced atrial fibrillation is the lack of a broadly accepted (and adhered to) standard protocol regarding the invasive procedure. Some of the differences between various studies could thereby be possibly explained by different pacing protocols (e.g. time, minimum CL, repetitions, use of catecholamines) and different definitions of the term inducible (especially the required time for being classified as such, varying from multiple minutes to only a few seconds).
Inducibility of atrial fibrillation via burst pacing during EPS in patients without a documented history of AF and atrial flutter seems to be associated with a subsequent higher risk of clinical atrial fibrillation. The prognostic value seems short-termed, since 2.5 years after testing the first members of the control group were also diagnosed with AF. Three years after testing, no statistically significant difference was left between both groups. Patients with a positive inducibility status were found to have a significantly higher age, a lower GFR, a higher rate of various valve insufficiencies and, more generally, a higher CHAD2S2-VASc score than their counterparts. As the numbers are too small and the current state of knowledge is not sufficient for discussing possible further consequences for patients with a positive inducibility status (e.g. prophylactic anticoagulation), we emphasize the so far more impressive and potentially clinically useful negative predictive value of the test, since all of our patients with a negative inducibility were free of diagnosed atrial fibrillation up to 2.5 years after testing. As our study was designed as an exploratory study, subsequent studies could also be performed in a prospective setting, employing patients with a planned implantation of a DDD-pacemaker, as most pacemakers would enable standardised atrial burst pacing (ideally during the implantation process) as well as a continuous follow up.
Figure 3. Kaplan-Meyer estimation, illustrating the event-free survival during the maximum course of follow-up, stratified by inducibility status.