32-year-old with Paroxysmal Atrial Fibrillation after Traumatic Spinal Cord Injury
Ting-Wei Teo1, Benjamin Yong-Qiang Tan24, Ching-Hui Sia34
1Internal Medicine Residency, National University Health System, Singapore.2Division of Neurology, Department of Medicine, National University Hospital, Singapore.3Department of Cardiology, National University Heart Centre Singapore, Singapore.4Department of Medicine, Yong Loo Lin School of Medicine, National University of Singapore.
A 32-year-old man presented with sudden loss of consciousness after passing urine with resultant trauma to the back of his neck. There were no palpitations prior. Examination revealed flaccid paralysis of all 4 limbs with priapism. Electrocardiogram demonstrated atrial fibrillation with rapid ventricular response. Laboratory showed normal potassium, magnesium, calcium, thyroid stimulating hormone and troponin I levels. Magnetic resonance imaging of the cervical spine demonstrated left C4 facet dislocation with grade 1 spondylolisthesis of C4 over C5, with moderate to severe narrowing of the spinal canal with cord compression and oedema. Transthoracic echocardiogram demonstrated an ejection fraction of 60% and no valvular abnormalities. Left atrium size was normal. The atrial fibrillation subsequently spontaneously reverted to sinus rhythm without treatment. Clinicians should be aware that atrial fibrillation can occur in the context of traumatic spinal cord injury due to disruption of the autonomic pathways in the cervical spine.
Key Words : Dofetilide, Atrial fibrillation, Protocol, Deviation.
Dr Ching-Hui Sia
Department of Cardiology
National University Heart Centre, Singapore
1E Kent Ridge Road, NUHS Tower Block Level 9, Singapore 119228
Traumatic spinal cord injury (SCI) is an under-recognised cause of atrial fibrillation (AF). We present a young man with a structurally normal heart and no secondary risk factors with cervical SCI, cord compression and resultant paroxysmal AF, demonstrating the “heart-brain axis” in the pathogenesis of AF.
A previously well 32-year-old man (CHA2DS2-VASc score 0) had sudden loss of consciousness after micturating and resultant trauma behind his neck. There were no preceding palpitations. He was a non-smoker and not on chronic medications, His pulse rate was irregular at 112 beats per minute with blood pressure of 208/113mmHg. Physical examination revealed flaccid paralysis of four limbs with priapism. Anal tone and perianal sensation were preserved. Electrocardiogram (ECG) demonstrated AF with rapid ventricular response, which subsequently spontaneously reverted to sinus rhythm without medications.
Blood investigations including electrolytes, thyroid panel and cardiac enzymes were unremarkable. Transthoracic echocardiogram revealed 60% ejection fraction and no valvular abnormalities. Left atrium size was normal. Magnetic resonance imaging of the cervical spine suggested anterior cord syndrome due to left C4 facet dislocation (grade 1 spondylolisthesis) with moderate to severe spinal canal narrowing, cord compression and oedema.
He was given intravenous dexamethasone and underwent open reduction of C4/C5 facet joint dislocation, anterior cervical discectomy and fusion. He recovered uneventfully and remained in sinus rhythm in subsequent follow-up.
Figure 1. Cervical spine magnetic resonance imaging (sagittal plane) demonstrating spinal cord compression and oedema at the C4 level (white arrow)
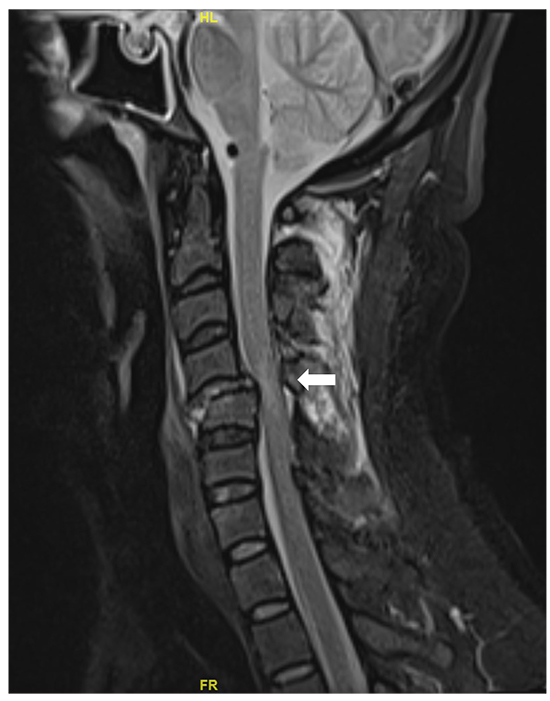
This case highlights the intricate pathophysiological interplay between the cardiovascular and autonomic nervous system in the pathogenesis of AF. High cervical SCI is characterized by disruption of descending spinal sympathetic pathways 1 with preservation of parasympathetic output, causing disordered cardiovascular control like blood pressure derangements and arrhythmias.
Studies commonly discuss bradyarrhythmias in patients with SCI 2. With regard to AF, a recent population-based cohort study in Taiwan showed the long-term risk of AF was higher in patients with SCI 3.
The mechanism behind pathogenesis of AF in SCI is complex and involves dynamic interplay between triggers and substrate abnormalities. Firstly, studies found patients with SCI had higher P-wave dispersion (PWD) values 4, which is a novel predictor in evaluating risk of AF. PWD is affected by autonomic dysfunction 5 in SCI as loss of normal heart sympathetic modulation results in prolonged intra-atrial conduction time and higher PWD values 4. This inhomogenous propagation of sinus impulses in the atria confers a higher risk of AF 6.
Secondly, some believe AF represents early manifestation of autonomic dysreflexia 7. Thirdly, some hypothesize the loss of central control and reflexes of the heart causes spontaneous sympathetic activity, which is reinforced by denervation hypersensitivity and triggers AF 8. Fourthly, secondary myocardium remodelling changes following SCI 9 may result in AF. Next, AF may be triggered by pain from trauma. Lastly, patients may develop AF independent of SCI.
While the exact mechanisms behind AF and SCI remains unclear, our case highlights complex interactions between the cardiovascular and nervous systems. This requires further study for the future treatment and prevention of AF and its complications.