Impact of Yoga on Cardiac Autonomic Function and Arrhythmias
Krishna Akella1, Sri Harsha Kanuri1, Ghulam Murtaza1, Domenico G. Della Rocca3, Naresh Kodwani4, Mohit K. Turagam7, Jayaprakash Shenthar8, Deepak Padmanabhan8, Indranill Basu Ray9, Andrea Natale6, Rakesh Gopinathannair5, Dhanunjaya Lakkireddy2
1Arrhythmia Research Fellow, Kansas City Heart Rhythm Institute (KCHRI), Overland Park, KS, USA.2Executive Medical Director, KCHRI, Overland Park, KS, USA.3Fellow, Texas Heart Rhythm Institute, Austin, TX, USA.4Internal Medicine Program Director, Overland Park Regional Medical Center, Overland Park, KS, USA.5Cardiac Electrophysiology Laboratory Director, KCHRI, Overland Park, KS, USA.6Executive Medical Director, Texas Heart Rhythm Institute, Austin, TX, US.7Icahn School of Medicine at Mount Sinai, New York, NY.8Sri Jayadeva Institute of Cardiovascular Sciences and Research , Bangalore , Karnataka, India.9The University of Memphis, Memphis, TN, USA; Visiting Professor and Head of Integrative Cardiology, AIIMS, Rishikesh, UK, India.
With the expanding integration of complementary and alternative medicine (CAM) practices in conjunction with modern medicine, yoga has quickly risen to being one of the most common CAM practices across the world. Despite widespread use of yoga, limited studies are available, particularly in the setting of dysrhythmia. Preliminary studies demonstrate promising results from integration of yoga as an adjunct to medical therapy for management of dysrhythmias. In this review, we discuss the role of autonomic nervous system in cardiac arrhythmia,interaction of yoga with autonomic tone and its subsequent impact on these disease states. The role of yoga in specific disease states, and potential future direction for studies assessing the role of yoga in dysrhythmia.
Key Words : Dysrhythmia, Atrial fibrillation, Ventricular arrhythmia, Neurocardiogenic syncope, Yoga.
Correspondence to: Dhanunjaya Lakkireddy, MD, FACC, FHRS
Executive Medical Director
The Kansas City Heart Rhythm Institute (KCHRI) @ HCA MidWest
Professor of Medicine, University of Missouri - Columbia
12200, W 106th street, Overland Park Regional Medical Center
Overland Park, KS 66215
Yoga is an ancient practice utilizing diverse postures and movements in conjunction with breathing methods geared towards facilitating a meditative state. While the practice of yoga is speculated to have existed since the 5000 BC, only more recently has clinical application of yoga and other similar alternative practices been evaluated within the context of modern medicine. Yoga is the most common alternative practice in America with an estimated 20.4 million people currently practicing - a dramatic increase (29%) from 2008 where 15.8 million people practiced 1. There is growing body of evidence that shows the beneficial effects of yoga as an adjunct to conventional treatments for various disease conditions including – chronic pain, orthopedic issues, heart failure, atrial fibrillation and many more. Autonomic nervous system (ANS) plays an important role in the initiation and maintenance of atrial arrhythmias. In this manuscript, we try to shed some light on the unique interaction between cardiac autonomic system and yoga.
Yoga is a philosophy and a way of life formalized by Patanjali 2000 years ago. This practice aimed to balance mind, body and spirit leading to calmness of mind and alleviation of psychological distress using eight foundational principles: yama (morality/restraint), niyama (duties), asana (posture – examples in Figure 1), pranayama (breathing technique), pratyahara (sense withdrawal), dharana (focused concentration), dhyana (meditative absorption), samadhi (enlightenment). Since development, yoga is broadly categorized into four major types with multiple styles. The four major traditional types of yoga include: Bhakti, Gnana (pronounced as ñana), Karma, and Kriya (with Hatha, Tantra, and Kundalini yoga subtypes). There are many particular styles of yoga practice as well Table 1,2.
Figure 1. Examples of Yoga Postures (Asanas).

Top row (left to right): Downward Dog, Mountain, Plough, Goddess, Tree Middle row: Lord of Dance, Plank, Lotus, Side Plank, Scorpion Bottom Row: Crescent, Wheel, Dancing Shiva, Lord of Fishes, Sundial
Table 1. Yoga Types and Styles
|
Yoga Types
|
Styles
|
|
Bhakti
|
Iyengar
|
|
Gnana
|
Vinyasa
|
|
Karma
|
Hot
|
|
Kriya(Hatha,Tantra,and Kundalini subtypes)
|
Ashtanga
|
| |
Sivananda
|
| |
Yin
|
| |
Restorative
|
| |
Anusara
|
| |
Prenatal
|
| |
Jivamukti
|
| |
Bikram
|
It is based on the premise that a central consciousness regulates the bodily function through flow of energy through Chakras distributed along the spinal column inwards and outwards. A Chakra is a powerhouse in the way it generates and stores energy, with the energy from cosmos pulled in more strongly at these points. The nadis – Ida (sympathetic) and Pingala (parasympathetic) run along the spinal column in a curved path and cross one another several times joining the Shushumna (central nervous system) at the top of the spinal column. At the points of intersection, they form strong energy centers known as chakras (spinal plexi) Figure 1.
Simply knowing the many different styles of yoga, one can begin to appreciate the difficulty in evaluating such a practice with uniformity. A major limitation to consider within the growing body of yoga research is the wide variability in what is considered yoga. As a result of heterogeneity (such as differences in yoga style, length of study, amount of time yoga is used, baseline population difference), identification of potential mechanisms of outcome improvement and ideal patient population can potentially be problematic as studies would ideally have replicable and cohesive findings that can be applied incrementally. Consequently, it can be difficult to make any generalizable statements about yoga and major studies should be individually assessed 3. Among available evidence for styles of yoga studied, no individual practice has been found to demonstrate significant superiority 4.
Impact of yoga on autonomic function and neurohormonal modulation
Yoga offers many beneficial effects on autonomic nervous system through modulation of rate, depth and pattern of breathing 5. Previously studies have shown that, yogic breathing can exert its positive effects through increasing heart rate variability, improving sympatho-vagal balance and promoting stress resilience 6-8. It was hypothesized that, yogic breathing causes activation of stretch receptors in the respiratory system to relay information through vagal afferents to central nervous system (CNS) areas to positively influence cognition, emotion, perception, behavior and somatic expression6,7. It is believed that, yoga practices modulate the stress related imbalances through increasing parasympathetic system, and γ-aminobutyric acid (GABA) system while decreasing hypothalamic – pituitary –adrenal axis 5. Additionally, yoga exercise was shown to positive role in reducing stress, anxiety and depression in young women and can be utilized as a complimentary medicine 9. The other positive effects of yoga exercise includes decrease in heart rate and blood pressure (systolic, diastolic and mean arterial) 10. The ancient Om mantra which is routinely used with yoga is associated with decreased vagal tone, physiological relaxation and limbic system deactivation 11,12. Yoga therapy has been demonstrated to reduce the systemic inflammatory response (Cortisol, CRP and IL-6), attenuate endothelial dysfunction and allosteric load 13,14.
Patients with 4 months of transcendental meditation therapy demonstrated attenuation of levels of stress hormones such as cortisol, testosterone, growth hormone and thyroid stimulating hormone as compared to control group emphasizing its importance in reversing the effects of chronic stress that can contribute to disease 15. In a randomized control trial, yoga therapy results in improvement of parameters of heart rate variability (HRV) especially those related to vagal tone such as SDNNi and rMSSD 16. Deep breathing exercises and relaxation leads to 50% reduction in premature ventricular contractions (PVC) burden through effects on cardiac ANS and purkinje system along with QT dispersion 17. In patients with neurocardiogenic syncope, yoga therapy has been shown to be improve the symptoms of syncope and presyncope 18. In the patients with cardiac arrhythmias, pranayama yoga therapy has been shown to reduce the ventricular repolarization dispersion thereby lowering the risk of developing malignant ventricular arrhythmias and sudden cardiac death 19. In heart failure patients, yoga therapy resulted in reduction in heart rate and blood pressure due to improved HRV, increased vagal tone and decreased sympathetic tone 20.
Emotional stress and cardiac arrhythmias
It is widely believed that, different emotions in humans are processed in different parts of forebrain. Positive emotions are processed in the left hemisphere whereas negative emotions were processed in the right hemisphere. Accordingly, positive emotions activate sympathetic neurons from the right hemisphere whereas negative emotions activate parasympathetic neurons from the left hemisphere. Right sided nerves innervate anterior aspect (right ventricle) whereas left sided nerves innervate postero-lateral aspect (left ventricle) resulting in lateralized innervation of heart. This lateralized emotional processing in the cortex along with lateralized innervation of the heart results in asymmetrical stimulation of heart, generation of repolarization heterogenecity, electrical instability resulting in facilitation of reentrant arrhythmias 21-23
Psychiatric disorders such as anxiety, depression and emotional stress were considered as common triggering pointsfor cardiac arrhythmias such as atrial fibrillation (AF). Following an episode of anger or negative emotions, the likelihood of developing AF will be increased to 5 fold whereas risk is decreased with episode of happiness 24,25. It is important to note that, anxiety associated with impatience, competitiveness and job involvement significantly increases the risk of developing AF 24,26. There is no direct relationship between emotional disorders and cardiac arrhythmias, but researchers proposed various pathological mechanisms thereby strengthening the causative relationship between these two clinical entities. Emotional stress and anxiety can lead to pathological consequences on neuroendocrine, coagulative, microcirculatory, immune systems ultimately resulting in cardiac arrhythmias 27.
ATTICA study had demonstrated that, anxiety is associated with upreglation of inflammatory markers such as C-reactive protein, interleukin-6, homocycteine and fibrinogen levels 28. Accordingly, systemic inflammatory response and hypercoagulation state associated with anxiety can predispose to development of cardiac arrhythmias. Moreover, inflammatory state of anxiety can attributed to excess activation of hypothalamic-pituitary adrenal axis with cortisol overproduction and associated imbalance of dopaminergic, serotoninergic and non-adrenergic neurons 29. Additionally, activation of sympathetic system with catecholamine overload can lead to extracellular matrix production, upregulation of collagen production, tumor growth factor (TGF)-beta, mononuclear infiltration, reactive oxygen species production resulting in negative atrial remodeling and atrial fibrosis 27,30-35. Lastly, anxiety can lead to activation of rennin angiotensin system (RAS) and over production of angiotension II leading to atrial fibrosis, left ventricular hypertrophy, increased atrial pressure/stretch which ultimately results in AF 27,35. Emotional disorders commonly activate the autonomous ganglia to initiate ectopic impulses in myocardial cells in pulmonary veins near their connection with left atrium and predispose to development of AF36.
Although most studies are small with limitations making it difficult to draw definitive conclusions given data quality, evidence exists to suggest that regular practice of yoga results in increased resting vagal tone. This conclusion is discerned based on markers of autonomic activity such as heart rate (HR)/HRV, baroreflex sensitivity, cognitive ability and emotional regulation. In certain disease states (such as diabetes, psychiatric conditions, pain and hypertension), yoga has demonstrated some benefit as an adjunct therapy 37-42. Despite individual study findings, definitive conclusions are controversial and will require further investigation 43,44.
Autonomic etiology of dysrhythmias and impact of Yoga
Syncope is loss of consciousness resulting from transient global cerebral hypo-perfusion typically due to neuroendocrine, orthostatic, arrhythmogenic and structural cardiopulmonary etiology. Reflex syncope collectively describes: neurocardiogenic (vasovagal) syncope, situational syncope (cough, micturition etc.), and carotid sinus syndrome 45-47.
The most common type of reflex syncope is neuro-cardiogenic and is commonly associated with reduced blood volume, dehydration, and elevated sympathetic tone 48,49. Ventricular stimulation in response to excess catecholamines triggers ventricular mechanoreceptors carrying signal to the medulla via the vagus nerve. The resulting efferent response creates a paradoxical attenuation in sympathetic tone with concurrent heightening of vagal tone. The consequence of this Bezold-Jarisch reflex is hypotension, and bradycardia (due to the sinoatrial impulse suppression in conjunction with reduction in the atrioventricular nodal conduction). Conservative measures consist of: trigger (prolonged standing, dehydration, temperature extreme) avoidance, counterpressure maneuvers (handgrip, squat, leg crossing), adequate hydration, salt intake, compression stockings, and tilt training46,47,50-54. Potential medications used include beta blockers, midodrine, fludrocortisone, selective serotonin reuptake inhibitors (SSRIs), and ivabradine. More invasive procedures with limited evidence include ganglionated plexus cardio-neuroablation and pacemaker implantation 55.
In 2015, Gunda et al 42 published a pilot study on the role of yoga as an adjunct therapy for neuro-cardiogenic syncope. This was a multicenter observational study which enrolled 44 patients with neuro-cardiogenic syncope in 2 arms -- a control arm (23 patients) and an intervention (yoga) arm (21 patients). The control arm monitored via log of syncopal and presyncopal episodes experienced over a six-month period. The intervention group had a 60-minute yoga video they were asked to participate in 3 times weekly for 3 months. All patients had a baseline history and physical examination, syncope functional questionnaire score (SFSQS), and head up tilt test (HUTT). At the end of the study, only the intervention group had a repeat HUTT and SFSQS. A positive HUTT was defined by the presence of bradycardia (HR under 40 for > 10 seconds or asystole for >3 seconds) and/or vasodepressor response (symptomatic hypotension or systolic blood pressure (BP) reduction below 60 mmHg). The study found a significant difference between the control and intervention group in mean syncopal episodes (4.0 + 1.0 vs. 1.3 + 0.7, p < 0.001), mean pre-syncopal episodes (4.7 + 1.5 vs. 1.5 + 0.5, p < 0.001), and reduction in SFSQS (67 + 7.8 vs. 29.8 + 4.6, p < 0.001) Figure 2 and Figure 3. Additionally, within the intervention group it was noted that all patients began with a positive HUTT but at the conclusion of the study, only 28% (6 patients) had a positive HUTT. Findings from the study demonstrate the clinical efficacy of yoga as an adjunct therapy in management of patients with neuro-cardiogenic syncope via accelerating blood volume return to the heart (similar to counter-pressure maneuvers previously mentioned) in conjunction with autonomic modulation Figure 4,18.
Figure 2. Impact on of Yoga on Syncopal and Presyncopal Episodes.
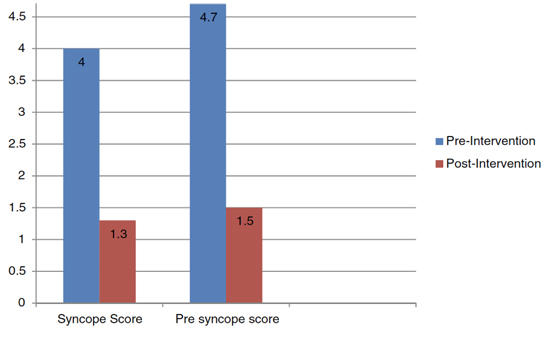
Copied with permission from Gunda et. al. 2015
42
Figure 3. Impact on of Yoga on Syncopal Functional Status Questionnaire Score (SFSQS).
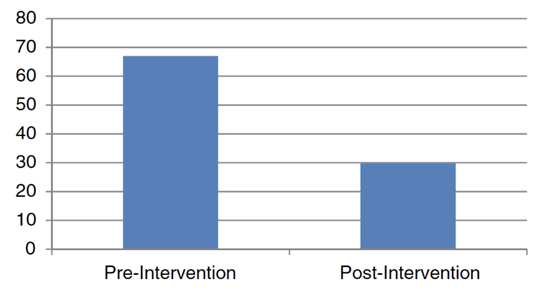
Copied with permission from Gunda et. al. 2015
42
Figure 4. Role of Yoga in Neurocardiogenic Syncope.
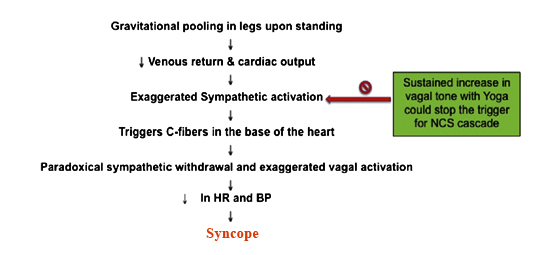
Copied with permission from Gunda et. al. 2015
42
AF has a well-established connection with the ANS. Heightened sympathetic tone with subsequent vagal overcompensation results in a milieu of shortened refractory period in conjunction with premature atrial beats, resulting in AF 56,57.Sympathetic activation can help propagate AF via beta-adrenergic receptor activation. The following vagal hyperactivity results in shortening of the refractory period as well as action potential duration 58.This, in conjunction with more recent evidence suggesting involvement of local cardiac ANS, specifically the modulatory effect of ganglionic plexi (GP), represents the current model for the underlying mechanism of AF 59. There is evidence to show that in some paroxysms of AF there is a significant surge in sympathetic tone preceding an AF episode which is triggered by a sudden withdrawal of the same and increase in parasympathetic tone. These types of sudden variations in cardiac autonomic tone form the patho-physiologic platform for many other types of arrhythmia substrates as well.
In 2013, The YOGA My Heart Study by our group assessed the clinical impact of yoga in patients with atrial fibrillation 60. The YOGA My Heart Study was a single center, self-controlled, cohort study conducted over a period of 6 months total (3 months with no yoga vs. 3 months with yoga). Baseline quality of life, depression and anxiety scores, hemodynamic parameters (HR and BP), and atrial fibrillation AF burden (using event monitor and self-reporting of symptoms) were used to evaluate at baseline (day 0), end of the control period (day 90) and end of the yoga intervention period (day 180). Patients were recommended to record at least one event on monitor per day even if asymptomatic. Yoga performed was structured Iyengar yoga occurring twice weekly with an instructor leading the class for approximately 60 minutes. Data from a total of 49 patients were used to assess comparative outcomes.
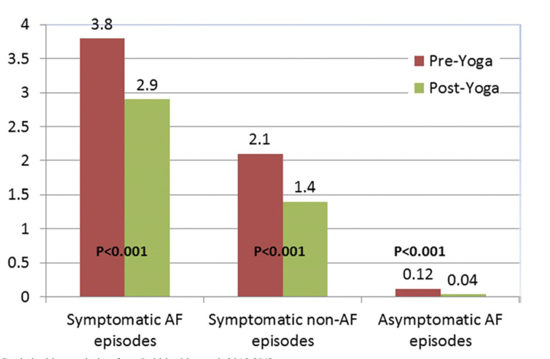
Event monitor recorded episodes were categorized into symptomatic AF, symptomatic non-AF, and asymptomatic AF. In all categories, regular practice of yoga was found to improve outcomes (Shown in Figure 5):
Figure 5. In all Categories, regular practice of yoga was found to improve outcomes.
Copied with permission from Lakkireddy et. al. 2013
54
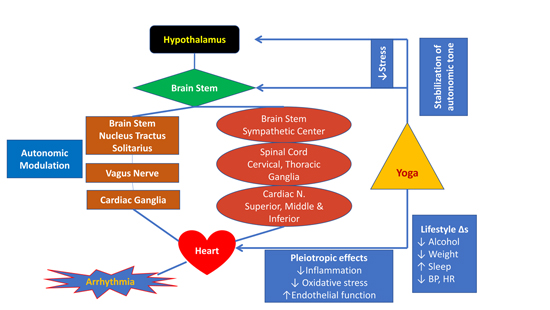
Figure 6. Shows the multipronged impact of Yoga on human body and reduction of cardiac arrhythmias.
. Reduction in mean number of symptomatic AF episodes: from 3.8+3 to 2.1+ 2.6 (p < 0.001).
. Reduction in mean number of symptomatic non-AF episodes: from 2.9+3.4 to 1.4+ 2.0 (p < 0.001).
. Reduction in mean number of asymptomatic AF episodes: from 0.12+0.44 to 0.04+ 0.20 (p < 0.001).
Of the patients with documented AF during the control phase, 22% did not have any observed episodes during the intervention phase. Aside from proof of concept regarding AF burden reduction, regular practice of yoga was demonstrated to reduce baseline heart rate as well as systolic and diastolic blood pressure. Other parameters measured including depression, anxiety, and quality of life scores improved as well. Notably, reduction in AF burden did not seem to correlate with change in hemodynamic parameters. The authors went to explain the improvement in depression, anxiety and quality of life by mentioning the effect of yoga on attenuation of stress response. They additionally hypothesized a plausible mechanism for AF prevention through regular practice of yoga: increased baseline parasympathetic tone, reduction in ANS fluctuations, and reduction in progression of AF through prevention or limiting of atrial remodeling 60.
Ventricular arrhythmia and sudden cardiac death
Within the heart, parasympathetic PANS and sympathetic SANS have a high degree of variability in distribution. Parasympathetic PANS has a much more focal spread than sympathetic SANS and is localized primarily in the sinoatrial (SA) node, the atrioventricular (AV) node and ganglionic plexi GPs embedded in atrial fat pads. Increased parasympathetic tone decreases rate of firing from the sinoatrial node SA and the atrioventricular AV nodal conduction velocity. This same effect is very much limited within ventricular muscle where sympathetic innervation plays a primary role. Although it appears that sympathetic and parasympathetic systems have opposite function, it should be noted that both systems work synchronously.
Myocardial infarction with resultant nerve and muscle necrosis creates a focus with a relative absence of sympathetic regulation - a functional denervation. In conjunction with surrounding tissue hypersensitivity, denervation (with resulting reduction in vagal tone) and tissue non-uniformity results in variable tissue refractory period resulting in ventricular ectopy.
Nerve sprouting in subsequent Wallerian degeneration is propagated by neural growth factor (NGF). This sprouting results in sympathetic hyperactivity - working in conjunction with factors mentioned above to enhance sympathetic ANS activation 61. Enhanced sympathetic activation is a known cause (based on animal models) for ventricular arrhythmia (VA) and sudden cardiac death (SCD) 62-64. In chronic catecholamine elevation, a situation commonly observed in heart failure, sympathetic neural dysfunction is observed similar to denervation in myocardial infarction. As a result, management which entails mortality benefit in heart failure typically entails use of medication that attenuates sympathetic activation. Medications commonly used for this includes angiotensin-converting enzyme inhibitors, beta blockers and spironolactone 61. More recently studies focusing on interventions geared towards sympathetic modulation have shown promising results on management of VA 65.
In a similar way, the heightened parasympathetic tone which goes hand in hand with the sympathetic attenuation with regular practice of yoga may be helpful as an adjunctive therapy in such a setting. Of the three major components common in all styles of yoga (pranayama, asana, and dhyana), each component is thought to modulate arrhythmogenesis with slightly different mechanisms Table 2,3. Among the three components, pranayama (breath control) has a significant body of supportive literature. Using different breath control techniques, variable impact on autonomic modulation can be achieved. Individual components of technique have been described including breath awareness (shown to independently reduce BP), slow breathing, and fast breathing Table 3. Overall, pranayama is thought to reset ANS using slow deep breathing resulting in stretch induced inhibitory signaling. During inspiration, lung stretch activation of fibroblast slowly adapting stretch receptors results in inhibitory signaling and hyperpolarization of neural and non-neural tissue. This synchronizes neural elements of the heart, lungs, limbic system and cortex. The resulting autonomic modulation and decrease in metabolic activity suggests a parasympathetic augmentation. Another supported hypothesis suggests that, stretch receptor activation above tidal volume results in sympathetic tone withdrawal in peripheral blood vessels via Hering-Bruer reflex 66. Future studies will need to better discern the benefit of yoga in the setting of ventricular ectopy.
Table 2. General Physiologic Mechanisms of Major Yoga Components
| Posture (Asana) |
Breath Control (Pranayama) |
Meditation (Dhyana) |
| Acrobic Exercise
. Autonomic Modulation
. Underlying risk factor improvement (obesity,blood pressure control etc.)
. Psychological Stress Reduction |
Pulmonary Stretch
. Autonomic modulation
. Heart Rate/Blood Pressure Control |
Psychological Stress Reduction
. Limbic/Autonomic attenuation |
| Isometric Resistance
. Muscle Strength
. Psychological Stress Reduction |
Psychological Stress Reduction
. Limbic/Autonomic attenuation
. HPA Modulation |
Improved Self Control
. Urge improvement and reduction of preventable risk factors |
Table 3. Physiologic Impact of Breath Control (Pranayama) Techniques
|
Slow Breathing
|
Fast Breathing
|
|
Nadi Shodhana
|
Savitri
|
Pranava
|
Kapalabhati
|
Bhastrika
|
Kukkuriya
|
|
Psychological Stress Reduction
|
Psychological Stress Reduction
|
Psychological Stress Reduction
|
Psychological Stress Reduction
|
Psychological Stress Reduction
|
Psychological Stress Reduction
|
|
Variable effects
|
|
Decreased HR
|
Decreased Baroreflex Sensitivity
|
Decreased HRV
|
|
| |
|
Decreased BP and PP
|
Decreased RR
|
Decreased BP
|
|
| |
|
Increased Baroreflex Sensitivity
|
Increased SBP
|
|
|
| |
|
Increased endogenous nitric oxide production
|
|
|
|
HR: Heart Rate; BP: Blood Pressure; PP: Pulse Pressure; HRV: Heart Rate Variability NadiShodhana: Alternate Nostril Breathing. Savitri: Controlled, slow, deep breathing. Pranava: Deep, meditative, slow breathing. Kapalbhati: Passive inspiration with forceful expiration. Bhastrika: Single nostril inspiration, breath holding and forced expiration using alternate nostril. Kukkuriya: Fast mouth breathing.
Conclusion and Future Directions
Yoga is an old complementary and alternative medicine (CAM) practice utilizing different movements, postures, and breathing techniques in conjunction with meditation. Early assessment of this practice as an adjunct to modern medical therapy has so far yielded promising results. The increase in vagal tone and reduction in autonomic fluctuation is the likely mechanism of how yoga reduces arrhythmia burden, improves hemodynamic parameters (such as resting HR and BP), and reduces symptoms. While future studies may attempt to differentiate styles of yoga or compare with similar CAM practices, yoga should be assessed in a variety of different dysrhythmias to improve our understanding of how and when this complementary practice should be used.
-
Yoga Journal Releases 2012 Yoga in America Market Study, in Yoga Journal. 2012.
- Patanjali, C.H., The Yoga-Sutra of Patanjali: A New Translation with Commentary (Shambhala Classics) 2003: Shambhala; Shambhala Classics edition (April 1, 2003).
- Howard, A.P., Improved Autonomic Function as a Physiological Mechanism Underlying the Reported Effects of Ashtanga Yoga:Feasibility and Initial Effectiveness Study. 2018, University of Windsor. p. 159.
- Cramer, H., et al., Is one yoga style better than another? A systematic review of associations of yoga style and conclusions in randomized yoga trials. Complementary Therapies in Medicine, 2016. 25: p. 178-187.
- Streeter, C.C., et al., Effects of yoga on the autonomic nervous system, gamma-aminobutyric-acid, and allostasis in epilepsy, depression, and post-traumatic stress disorder. Med Hypotheses, 2012. 78(5): p. 571-9.
- Brown, R.P. and P.L. Gerbarg, Sudarshan Kriya Yogic breathing in the treatment of stress, anxiety, and depression. Part II--clinical applications and guidelines. J Altern Complement Med, 2005. 11(4): p. 711-7.
- Brown, R.P. and P.L. Gerbarg, Yoga breathing, meditation, and longevity. Ann N Y Acad Sci, 2009. 1172: p. 54-62.
- Bernardi, L., et al., Slow breathing reduces chemoreflex response to hypoxia and hypercapnia, and increases baroreflex sensitivity. J Hypertens, 2001. 19(12): p. 2221-9.
- Shohani, M., et al., The Effect of Yoga on Stress, Anxiety, and Depression in Women. International journal of preventive medicine, 2018. 9: p. 21-21.
- Murugesan, M. and A.G. Taylor. Effect of Yoga on the Autonomic Nervous System : Clinical Implications in the Management of Atrial Fibrillation. 2017.
- Saper, R.B., et al., Yoga for chronic low back pain in a predominantly minority population: a pilot randomized controlled trial. Alternative therapies in health and medicine, 2009. 15(6): p. 18-27.
- Telles, S., R. Nagarathna, and H.R. Nagendra, Autonomic changes during "OM" meditation. Indian J Physiol Pharmacol, 1995. 39(4): p. 418-20.
- Kiecolt-Glaser, J.K., et al., Stress, inflammation, and yoga practice. Psychosom Med, 2010. 72(2): p. 113-21.
- Cheng, T.O., Effect of Tai Chi on endothelial function. Clin Cardiol, 2007. 30(3): p. 150.
- MacLean, C.R., et al., Effects of the Transcendental Meditation program on adaptive mechanisms: changes in hormone levels and responses to stress after 4 months of practice. Psychoneuroendocrinology, 1997. 22(4): p. 277-95.
- Khattab, K., et al., Iyengar yoga increases cardiac parasympathetic nervous modulation among healthy yoga practitioners. Evid Based Complement Alternat Med, 2007. 4(4): p. 511-7.
- Yetkin, E., et al., Beneficial effect of deep breathing on premature ventricular complexes: Can it be related to the decrease in QT dispersion? International Journal of Cardiology, 2006. 113(3): p. 417-418.
- Gunda, S., et al., Role of yoga as an adjunctive therapy in patients with neurocardiogenic syncope: a pilot study. J Interv Card Electrophysiol, 2015. 43(2): p. 105-10.
- Dabhade, A.M., et al., Effect of pranayama (breathing exercise) on arrhythmias in the human heart. Explore (NY), 2012. 8(1): p. 12-5.
- Krishna, B.H., et al., Effect of yoga therapy on heart rate, blood pressure and cardiac autonomic function in heart failure. Journal of clinical and diagnostic research : JCDR, 2014. 8(1): p. 14-16.
- Lane, R.D. and J.R. Jennings. Hemispheric asymmetry, autonomic asymmetry, and the problem of sudden cardiac death. The MIT Press 1995.
- Taggart, P., Brain-heart interactions and cardiac ventricular arrhythmias. Neth Heart J, 2013. 21(2): p. 78-81.
- Fransson, E.I., et al., The Association between Job Strain and Atrial Fibrillation: Results from the Swedish WOLF Study. BioMed research international, 2015. 2015: p. 371905-371905.
- Shusterman, V. and R. Lampert, Role of Stress in Cardiac Arrhythmias. Journal of atrial fibrillation, 2013. 5(6): p. 834-834.
- Lampert, R., et al., Triggering of symptomatic atrial fibrillation by negative emotion. J Am Coll Cardiol, 2014. 64(14): p. 1533-4.
- Sterndorff, B. and D.F. Smith, Normal values for Type A behaviour patterns in Danish men and women and in potential high-risk groups. Scand J Psychol, 1990. 31(1): p. 49-54.
- Severino, P., et al., Triggers for Atrial Fibrillation: The Role of Anxiety. Cardiol Res Pract, 2019. 2019: p. 1208505.
- Pitsavos, C., et al., Anxiety in relation to inflammation and coagulation markers, among healthy adults: the ATTICA study. Atherosclerosis, 2006. 185(2): p. 320-6.
- Pasquini, M., I. Berardelli, and M. Biondi, Ethiopathogenesis of depressive disorders. Clinical practice and epidemiology in mental health : CP & EMH, 2014. 10: p. 166-171.
- Nef, H.M., et al., Expression profiling of cardiac genes in Tako-Tsubo cardiomyopathy: insight into a new cardiac entity. J Mol Cell Cardiol, 2008. 44(2): p. 395-404.
- A., A., Anxiety and atrial fibrillation: an interesting bidirectional association. Curr Trend Cardiol., 2017. 1(1): p. 15-18.
- Carney, R.M., K.E. Freedland, and R.C. Veith, Depression, the Autonomic Nervous System, and Coronary Heart Disease. Psychosomatic Medicine, 2005. 67.
- Lefer D.J., G.D.N., Oxidative stress and cardiac disease. American Journal of Medicine, 2000. 109(4): p. 315-323.
- Mlinarevic, D., et al., Pathophysiological mechanisms of Takotsubo cardiomyopathy-a systematic review. 2017.
- Szardien, S., et al., Mechanisms of stress (takotsubo) cardiomyopathy. Heart Failure Clinics, 2013. 9(2): p. 197-205.
- Mahida, S., et al., Science Linking Pulmonary Veins and Atrial Fibrillation. Arrhythmia & electrophysiology review, 2015. 4(1): p. 40-43.
- Hagins, M., et al., Effectiveness of yoga for hypertension: systematic review and meta-analysis. Evid Based Complement Alternat Med, 2013. 2013: p. 649836.
- Innes, K.E., C. Bourguignon, and A.G. Taylor, Risk indices associated with the insulin resistance syndrome, cardiovascular disease, and possible protection with yoga: a systematic review. J Am Board Fam Pract, 2005. 18(6): p. 491-519.
- Li, A.W. and C.A. Goldsmith, The effects of yoga on anxiety and stress. Altern Med Rev, 2012. 17(1): p. 21-35.
- McCall, M.C., et al., Overview of Systematic Reviews: Yoga as a Therapeutic Intervention for Adults with Acute and Chronic Health Conditions. Evidence-Based Complementary and Alternative Medicine, 2013. 2013: p. 945895.
- Pilkington, K., et al., Yoga for depression: the research evidence. J Affect Disord, 2005. 89(1-3): p. 13-24.
- Tyagi, A. and M. Cohen, Yoga and hypertension: a systematic review. Altern Ther Health Med, 2014. 20(2): p. 32-59.
- Posadzki, P., et al., Yoga for Heart Rate Variability: A Systematic Review and Meta-analysis of Randomized Clinical Trials. Appl Psychophysiol Biofeedback, 2015. 40(3): p. 239-49.
- Tyagi, A. and M. Cohen, Yoga and heart rate variability: A comprehensive review of the literature. International journal of yoga, 2016. 9(2): p. 97-113.
- Bartoletti, A., et al., Hospital admission of patients referred to the Emergency Department for syncope: a single-hospital prospective study based on the application of the European Society of Cardiology Guidelines on syncope. Eur Heart J, 2006. 27(1): p. 83-8.
- Sutton, R., Reflex syncope: Diagnosis and treatment. Journal of arrhythmia, 2017. 33(6): p. 545-552.
- Task Force for the, D., et al., Guidelines for the diagnosis and management of syncope (version 2009). European heart journal, 2009. 30(21): p. 2631-2671.
- Alboni, P. and M. Alboni, Typical vasovagal syncope as a "defense mechanism" for the heart by contrasting sympathetic overactivity. Clin Auton Res, 2017. 27(4): p. 253-261.
- da Silva, R.M.F.L., Syncope: epidemiology, etiology, and prognosis. Frontiers in physiology, 2014. 5: p. 471-471.
- Brignole, M., et al., Isometric arm counter-pressure maneuvers to abort impending vasovagal syncope. J Am Coll Cardiol, 2002. 40(11): p. 2053-9.
- Krediet, C.T., et al., Management of vasovagal syncope: controlling or aborting faints by leg crossing and muscle tensing. Circulation, 2002. 106(13): p. 1684-9.
- Lee, A.K.Y. and A.D. Krahn, Evaluation of syncope: focus on diagnosis and treatment of neurally mediated syncope. Expert Review of Cardiovascular Therapy, 2016. 14(6): p. 725-736.
- Shen, W.-K., et al., 2017 ACC/AHA/HRS Guideline for the Evaluation and Management of Patients With Syncope: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines and the Heart Rhythm Society. Circulation, 2017. 136(5): p. e60-e122.
- van Dijk, N., et al., Effectiveness of physical counterpressure maneuvers in preventing vasovagal syncope: the Physical Counterpressure Manoeuvres Trial (PC-Trial). J Am Coll Cardiol, 2006. 48(8): p. 1652-7.
- Rocha, B.M.L., et al., Diagnostic and therapeutic approach to cardioinhibitory reflex syncope: A complex and controversial issue. Revista Portuguesa de Cardiologia (English Edition), 2019. 38(9): p. 661-673.
- Hoff, H.E. and L.A. Geddes, Cholinergic Factor in Auricular Fibrillation. Journal of Applied Physiology, 1955. 8(2): p. 177-192.
- Lewis, T., A. Drury, and H. Bulger, Observations upon atrial flutter and fibrillation. VI. Refractory period and rate of propagation in the auricle: their relation to block in the auricular walls and to flutter etc. Heart, 1921. 8: p. 84-134.
- Xi, Y. and J. Cheng, Dysfunction of the autonomic nervous system in atrial fibrillation. Journal of thoracic disease, 2015. 7(2): p. 193-198.
- He, B., et al., The intrinsic autonomic nervous system in atrial fibrillation: a review. ISRN cardiology, 2012. 2012: p. 490674-490674.
- Lakkireddy, D., et al., Effect of yoga on arrhythmia burden, anxiety, depression, and quality of life in paroxysmal atrial fibrillation: the YOGA My Heart Study. J Am Coll Cardiol, 2013. 61(11): p. 1177-82.
- Vaseghi, M. and K. Shivkumar, The role of the autonomic nervous system in sudden cardiac death. Prog Cardiovasc Dis, 2008. 50(6): p. 404-19.
- Han, J., P. Garciadejalon, and G.K. Moe, ADRENERGIC EFFECTS ON VENTRICULAR VULNERABILITY. Circulation research, 1964. 14: p. 516-524.
- Shen, M.J., et al., 40 - Neural Activity and Atrial Tachyarrhythmias, in Cardiac Electrophysiology: From Cell to Bedside (Seventh Edition), D.P. Zipes, J. Jalife, and W.G. Stevenson, Editors. 2018, Elsevier. p. 375-386.
- Stavrakis, S., et al., 44 - Role of the Autonomic Nervous System in Atrial Fibrillation, in Cardiac Electrophysiology: From Cell to Bedside (Seventh Edition), D.P. Zipes, J. Jalife, and W.G. Stevenson, Editors. 2018, Elsevier. p. 419-425.
- Bourke, T., et al., Neuraxial modulation for refractory ventricular arrhythmias: value of thoracic epidural anesthesia and surgical left cardiac sympathetic denervation. Circulation, 2010. 121(21): p. 2255-2262.
- Nivethitha, L., A. Mooventhan, and N.K. Manjunath, Effects of Various Prāṇāyāma on Cardiovascular and Autonomic Variables. Ancient science of life, 2016. 36(2): p. 72-77.