Percutaneous epicardial left atrial appendage (LAA) closure is the newest addition to the rapidly budding science of non pharmacological methods to prevent stoke in patients with Atrial Fibrillation (AF)
Stroke is a major cause of death and low quality of life worldwide. About 20% of ischemic strokes are cardio embolic in origin, with AF being the most common cause. Pharmacological prevention had success mainly with Warfarin but with various limitation including frequent monitoring, risk of major bleeding, drug and dietary interactions. While newer agents had associated toxicity, non pharmacological prevention is rapidly evolving as an alternative approach.
A recent study performed by Friedman et al, demonstrated the technique of percutaneous catheter based approach through the epicardium under the guidance of electrogram in identifying and ligating the Left atrial appendage. The technique was performed in four mongrel dogs, under the approval of Mayo Clinic Animal Care and Use Committee. The system (engineered by Access Point Technologies, Rogers, MN, USA) permits LAA closure in the closed pericardial space with a single sheath puncture. It has 2 components: an appendage grasper and a ligator. The grasper (Fig.1A) has an articulating jaw with specially mounted electrodes to permit navigation and identification of position and tissue captured by means of electrical signals. An atrial electrogram recorded between the 2 jaws identifies the tissue.
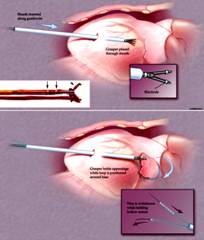
captured as atrial myocardium, thus distinguishing the LAA from epicardial fat and ventricular tissue. The second component of the system is a hollow suture that is preloaded with a 0.012 inch support wire. The wire in the suture provides mechanical support to permit advancement of the loop and fluoroscopic visualization. Once the LAA is controlled by the grasper, a hollow suture loop is advanced over the grasper, around the free margin of the appendage (Fig. 1B) and to its base. In the event of distal loop placement (i.e., the first loop is not at the most basal position possible) or if multiple appendage lobes are present, the system permits use of the first suture as a guide over which subsequent, more proximal sutures can be placed to better close the appendage.
During loop closure, echocardiographic images demonstrated progressive diminution of the LAA orifice until complete closure was seen, analogous to the findings during TEE in successful surgical closure. Associated with the progressive diminution of the LAA cavity was an increasing LAA Doppler derived velocity until full closure, at which time blood flow velocities were abolished. Subsequently, the completeness of the LAA closure was confirmed by open thoracotomy.
The complex anatomy of the LAA led to poor outcomes of usage of previous left atrial occluder devices. This novel technique employing percutaneously delivered epicardial suture with an operator controlled, individually adjustable-size loop aims at overcoming the limitations of previous devices. The validation of successful LAA closure with an open thorocotomy procedure to confirm complete isolation and ligation of LAA without significant limitations and complications is definitely promising for wider adaptation. Before the medical community gets too excited, feasibility, safety and efficacy of this technique in humans are yet to live up to the hope. This technique may allow decreasing the risk of stroke in AF patients without the need for thoracotomy or an endocardially placed prosthetic device. Studies involving the long term follow up with the usage of this technique are necessary to validate the birth of new age procedure adding to rapid advancements in cardiac electrophysiology.
Display Ads on JAFIB to reach Users world wide...
Suggest an Event to get good mileage from Users World wide...