Quality of Life, Exercise Capacity and
Comorbidity in Old Patients with Permanent Atrial Fibrillation
Inger Ariansena, Knut Gjesdala, Michael Abdelnoorb, Elisabeth Edvardsenc, Steve Engerd, Arnljot Tveitd
Department of Cardiology, Ullevål University Hospital, Oslo, Norway, Center for Clinical Research, Ullevål University Hospital, Oslo, Norway, cepartment of Pulmonary Medicine, Ullevål University Hospital, Oslo, Norway, dDepartment of Internal Medicine, Asker & Bærum Hospital, Rud, Norway.
The impact of atrial fibrillation (AF) on quality of life (QoL) differs with the AF population studied and is influenced by comorbidity. In hospital-based studies younger and highly symptomatic patients may be overrepresented. We performed an observational cross sectional study in two municipalities, comparing 75 year-old patients with and without permanent atrial fibrillation, with respect to health-related QoL and exercise capacity, with adjustment for the effects of confounders.
Maximal treadmill exercise testing provided peak oxygen uptake (VO2 peak). Health-related QoL was assessed by self-completed SF-36 questionnaires. The lowest quartile identified poor outcomes. Results: 27 subjects with permanent AF and 71 subjects in sinus rhythm participated. AF patients had higher prevalence of compensated chronic heart failure (p < 0.001), valvular heart disease (p < 0.001), lower mean VO2 peak (22.7 ± 5.5 vs. 28.6 ± 6.3 ml/kg/min; p < 0.001), and more often poor VO2 peak; crude OR 5.3 (95%CI 1.8, 15.3), adjusted OR 7.5 (2.0, 28.3). Median Physical Component Summary score (with 25th and 75th percentile) was 41 (31, 51) in AF vs. 52 (45, 55) in controls (p < 0.001). Furthermore, the AF group had higher odds for poor physical QoL scores; crude OR 5.0 (1.8, 13.7), adjusted OR 4.3 (1.5, 12.4). Median Mental Component Summary score was 56 (42, 61) in the AF group vs. 57 (51, 60) in controls (p=0.565). The AF group had non-significantly increased odds for poor mental QoL scores; crude OR 2.3 (0.8, 6.2), adjusted OR 2.8 (1.0, 8.4).
Also after adjustment for confounders, older patients with permanent AF had higher odds for poor exercise capacity and poor physical QoL compared to subjects in sinus rhythm.
Correspondence to: Inger Ariansen, MD, Arrhythmia Center, Department of Cardiology, Ullevål University Hospital, 0407 Oslo, Norway.
The prevalence of atrial fibrillation (AF) is high and increases exponentially with age, from 0.7% in the age group 55-60 years, to 17.8% in those aged 85 years and older.1 The number of AF patients is estimated to increase 2.5 fold during the next 50 years.2,3 The hospitalization rate for AF is increasing4 and AF patients have an excess mortality.5
To plan health services for old people with AF, data are needed not only on the prevalence of AF, but also on the impact of AF on their QoL. Neither hospital-based studies nor randomized studies, for instance on drug treatment or on rate versus rhythm control, are suitable for assessing the quantitative dimension of the health service programs for old patients with AF. In hospital-based studies younger and highly symptomatic patients may be overrepresented. Since cardiovascular and other diseases predispose to AF, epidemiologic data on AF should be adjusted for the confounding effects of comorbidity. The aim of the present study was to investigate the impact of AF on exercise capacity and QoL in a 75 year-old out-of-hospital population.
The study was approved by the Regional Ethics Committee in Health Region East Norway. All patients provided written informed consent in accordance with the revised Declaration of Helsinki before enrolment.
The design of the study was cross sectional with exposed (atrial fibrillation, AF+) and non-exposed (sinus rhythm, AF-) subjects. The endpoints were peak oxygen uptake (VO2 peak), and physical and mental QoL. Patients with AF+ and controls with AF- were recruited from the same source population. The lowest quartiles of the total study population identified poor outcomes. This report follows the epidemiologic guidelines for reporting observational studies.6
The source population comprised all citizens born in 1930 in two Norwegian municipalities, who were invited to ECG screening in the Asker and Bærum Atrial Fibrillation study, ABAF.7 Subjects with permanent AF and a control group in sinus rhythm were invited to perform cardiopulmonary exercise testing (CPET), a 24h ECG, and to fill in self-assessed health-related QoL questionnaires. Exclusion criteria were paroxysmal AF, atrial flutter, AF in a patient with a pacemaker that stimulated >30% of the time, or mental inadequacy. The data were collected from June to October 2005 at Ullevål University Hospital.
Cardiopulmonary Exercise Testing
The participants performed a maximal treadmill exercise test, measuring peak oxygen uptake (VO2 peak). A warm-up phase was followed by a progressive one-minute step protocol with equal energy steps. The test aimed at achieving near maximum exhaustion corresponding to the Borg scale8,9 (range 6-20).
The Medical Outcomes Study Short Form-36 (SF-36)
The standard (four weeks recall) Norwegian version of Medical Outcomes Study Short Form-36 (SF-36)9was mailed to the participants. The US general population means, standard deviations and factor score coefficients were used in the norm based aggregation of the eight scales into two components: The Physical Component Summary score (PCS) and the Mental Component Summary score (MCS).10 The SF -36 Norwegian normative data11 were similarly transformed into PCS and MCS scores. Quality control of the data was performed according to the SF 36 manual.12
A clinical diagnosis was either reported by the participants or revealed by test results during the study. Hypertension was defined as a history of treated hypertension or BP ≥ 160/100. Coronary artery disease (CAD) was defined as a history of CAD or a positive coronary angiography. Valvular heart disease was defined as mitral and/or aortic valve pathology ≥ grade 2 on echocardiography. A history of chronic pulmonary disease or FEV1/FVC<65% defined chronic pulmonary disease.13 Charlson Comorbidity Index was scored.14
Comparisons between groups were performed by the Students t-test, Mann-Whitney test or Chi square test where appropriate. We performed a stratification analysis using the Mantel-Haenszel method to pinpoint effect modification by the Breslow-Day test of homogeneity and to quantify confounders.15,16 Adjustment for multi-confounders was performed by the logistic model; a backward elimination procedure was used taking in consideration the concept validity and precision.15 The data were analyzed using the SPSS version 15.0 (SPSS Inc., Chicago, Illinois USA).
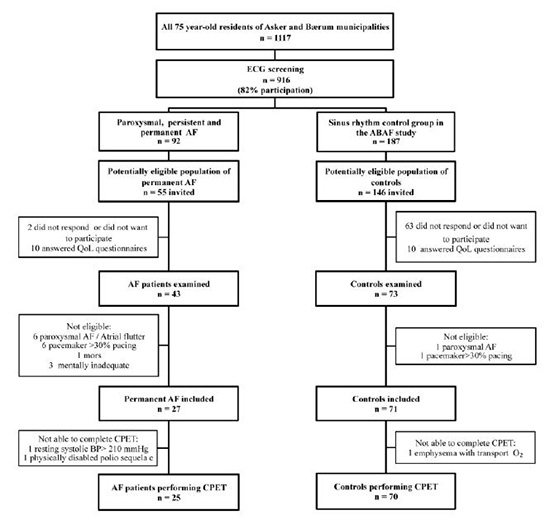
The main features of the Asker and Bærum Atrial Fibrillation study have been reported elsewhere.7 Briefly, 916 out of all subjects (n=1117) aged 75 in two municipalities in Eastern Norway participated in a prevalence study of AF. 55 patients had permanent AF, and 27 AF patients and 71 controls participated in the present study (Figure 1]).
Figure 1. Flowchart of inclusion of study participants
Median AF duration was 5 years (range 0.6-25 years). AF patients had a higher prevalence of compensated chronic heart failure (p < 0.001) and valvular heart disease (p < 0.001) compared to controls without AF (Table 1). Furthermore, AF patients had a higher number of medications compared to controls (p < 0.001).
Table 1. Clinical characteristics, n (%).
|
Atrial fibrillation |
p-values |
|
Yes
n 27
|
No
n 71
|
|
| Female gender |
7 (26) |
20 (28) |
0.824 |
| Body mass index (kg/m²)* |
25.3 ± 3.5 |
25.8 ± 3.1 |
0.495 |
| Systolic blood pressure (mmHg)* |
151 ± 26 |
158 ± 24 |
0.206 |
| Resting heart rate (beats/min)** |
68 (60, 84) |
65 (60, 72) |
0.052 |
| Mean 24 hour heart rate** |
73 (63, 77) |
68 (64, 74) |
0.099 |
| Coronary artery disease |
10 (37.0) |
13 (18.3) |
0.051 |
| Chronic heart failure |
7 (26) |
0 (0) |
<0.001 |
| Valvular disease |
7 (26) |
1 (1) |
<0.001 |
| Hypertension grade II |
17 (63) |
30 (42) |
0.067 |
| Stroke |
2 (7) |
2 (3) |
0.649 |
| Pulmonary disease |
7 (26) |
14 (19.7) |
0.503 |
| Diabetes |
3 (11) |
4 (6) |
0.616 |
| Anxiety/depression |
5 (19) |
4 (6) |
0.121 |
| Number of medications** |
5 (4, 8) |
2 (1, 4) |
<0.001 |
| Charlson Comorbidity Index* |
1.0 ± 1.1 |
0.6 ± 0.8 |
0.079 |
| Education after primary school (years)* |
6.2 ± 3.6 |
6.4 ± 3.5 |
0.803 |
| Still employed |
3 (11) |
9 (13) |
0.998 |
| Physically very active (bicycling, swimming, running, skiing) |
6 (22) |
20 (28) |
0.551 |
| Receiving help from housekeeper funded from the municipality |
1 (4) |
2 (3) |
1.000 |
*Mean ± SD. ** Median (25th, 75th percentile).
Definition of Poor Outcome
The lowest quartiles of the study population had VO2 peak less than 22 ml/kg/min, PCS less than 41 for physical QoL, and MCS less than 49 for mental QoL.
No adverse events were seen during or after the exercise testing. AF patients had lower mean VO2 peak than the controls; 22.7±5.5 vs. 28.6 ± 6.3 ml/kg/min; p < 0.001 (Table 2). The VO2 results include maximal as well as submaximal tests, and reflect the average exercise capacity in this out-of-hospital population. A history of stroke was found to be an effect modifier, and for this reason two AF patients and two controls with a history of stroke were left out of the analysis for poor VO2 peak. AF patients more often had poor VO2 peak; OR 7.5 (2.0, 28.3) after adjustment for the effects of CAD, diabetes and gender (Table 3).
Table 2. Exercise capacity, mental QoL and physical QoL in patients with and without atrial fibrillation
|
Atrial fibrillation |
Control |
p-value |
| VO₂* |
22.7 ± 5.5
|
28.6 ± 6.3 |
<0.001 |
| PCS** |
41 (31,51) |
52 (45, 55)
|
<0.001 |
| MCS** |
56 (42, 61)
|
57 (51, 60) |
0.565 |
VO₂ peak = peak oxygen uptake, PCS = SF-36 Physical Component Summary score, MCS = SF-36 Mental Component Summary score. Higher score indicates better QoL (quality of life). *Mean ± SD. **Median (25th, 75th percentile)
Table 3. Effect of atrial fibrillation on poor exercise capacity, poor physical QoL and poor mental QoL, n (%)
|
|
Atrial fibrillation |
ORCrude (95% CI) |
ORAdj (95% CI) |
Confounders |
|
|
Yes |
No |
|
|
|
| Poor VO₂ peak* |
Yes |
11 (48) |
10 (15) |
5.3 (1.8, 15.3) |
7.5 (2.0, 28.3) |
Gender |
|
No |
12 (52) |
58 (85) |
p=0.001 |
p=0.003 |
Coronary artery disease |
|
|
|
|
|
|
Diabetes |
| Poor PCS |
Yes |
12 (48) |
11 (16) |
5.0 (1.8, 13.7) |
4.3 (1.5, 12.4) |
Coronary artery disease |
|
No |
13 (52) |
59 (84) |
p=0.001 |
p=0.007 |
Diabetes |
| Poor MCS |
Yes |
9 (36) |
14 (20) |
2.3 (0.8, 6.1) |
2.8(1.0, 8.3) |
Gender |
|
No |
16 (64) |
56 (80) |
p=0.109 |
p=0.059 |
Chronic pulmonary disease |
|
|
|
|
|
|
Diabetes |
VO2 peak = peak oxygen uptake. MCS = SF-36 Mental Component Summary score. PCS = SF-36 Physical Component Summary score. Higher score indicates better QoL (quality of life). Poor outcome represents the lower quartile vs. the three higher quartiles of the total study population. ORCrude = the OR without adjustment for confounders. ORAdj = the OR adjusted for confounding effect. *The patients with stroke are excluded from the analyses of poor VO2.
Median physical QoL score PCS (25th, 75th percentile) was 41 31, 51 in the AF group vs. 52 45, 55 in controls (p < 0.001) (Table 2). The AF group had higher odds for poor PCS; OR 4.3 (1.5, 12.4) after adjustment for CAD and diabetes (Table 3). Gender was found to be an effect modifier for the relation between AF and poor PCS. There were too few females to permit separate analysis for both genders. We therefore performed separate analyses for the males. However, the odds for poor PCS in AF males compared to male controls (adjusted OR 2.7 (0.7, 10.4) ) was weaker than the odds for poor PCS in AF found for both genders combined. There was little difference in median mental QoL score between the groups; MCS 56 42, 61 in the AF group versus 57 51, 60 in controls (p=0.565) (Table 2). However, the AF group had a trend towards higher odds for poor MCS; adjusted OR 2.8 (1.0, 8.4) adjusting for diabetes, pulmonary disease and gender (Table 3). The distribution of MCS in the AF patients was bimodal; a subgroup with low MCS probably accounting for the increased OR for poor MCS in AF patients. The larger AF subgroup with higher MCS explains the similar median MCS for AF patients vs. controls.
As for the normative Norwegian data for SF-36, the study females scored lower than the males. The controls scored equally or higher for MCS and PCS than their corresponding age group in the Norwegian normative population.11 The AF patients scored equally or somewhat lower than their corresponding normative age group, except for the MCS score where the AF males scored higher than their corresponding normative data.
The confounders CAD and diabetes weakened the relation between AF and poor PCS by 13%. The relation between AF and poor VO2 peak was strengthened by 41% after adjusting for gender, CAD and diabetes. Adjusting for gender, diabetes and chronic pulmonary disease strengthened the relation between AF and poor MCS by 26%. A history of compensated chronic heart failure and of valvular heart disease was not considered as potential confounders because of their close association to AF. Still, for validity reasons we forced the two diagnoses into the multivariate regression model, and found that whereas the odds estimates were strengthened, the confidence intervals widened (data not shown).
In this population-based study on 75 year-old subjects, patients with permanent AF had lower exercise capacity as well as higher odds for poor physical QoL than subjects in sinus rhythm.Also after adjustment for confounders and consideration of effect modifiers, the AF patients had higher adjusted odds for poor exercise capacity and poor physical QoL compared to controls. Thus, AF itself, and not the associated comorbidity, seems to be responsible for the impaired physical QoL and exercise capacity in these old patients. To the best of our knowledge, the present study is the first controlled community-based study to investigate maximal CPET, QoL and comorbidity in old patients with permanent AF compared to controls in sinus rhythm. Albeit the small size of the study, the results appear consistent, presumably due to the homogenous out-of-hospital patient groups, the thorough examination and the use of a control group from the same source population.
Howes et al.17 compared QoL and exercise tolerance in elderly men with permanent AF to a control group without AF. At variance from our observation, they found no significant differences in SF-36 scores or exercise tolerance between the AF and the non-AF groups after adjusting for comorbidity.17 This study, however, differs from ours in several aspects. Females were almost not represented, recruitment was done at an outpatient clinic (hence it was a referred population), and third, the exercise tolerance test did not include VO2 measurement.
Community data are mandatory to assess the need for therapeutic measures. Highly symptomatic elderly patients with permanent AF are occasionally offered palliation through AV-node ablation and pacemaker implantation. Their exercise capacity and QoL then improve dramatically,18 but this population is highly selected. Several studies compare the strategies of rate versus rhythm control.19-22 and report little difference in QoL between the two strategies. These studies, however, suffer from several limitations with respect to exercise capacity and QoL. The groups are not compared to a control group without AF. The patients recruited to such studies are the ones who were willing to accept randomization to a rate-control group, and therefore the patients with more troublesome symptoms might not participate. Patients who were unable to achieve sinus rhythm before randomization, were excluded, selecting a more healthy study population. Furthermore, the rate-control group in AF was compared with AF patients kept in sinus rhythm by drugs that often are accompanied by side effects that reduce QoL. Some observational studies on QoL in outpatients with paroxysmal or newly diagnosed AF report impaired QoL in AF compared to controls without AF.23-25 Paroxysmal or newly diagnosed AF is probably more symptomatic than permanent AF,26 thus the results are not applicable for patients with permanent AF.
The populations in the municipalities of Asker and Bærum have a high socio-economic level. They rank among the top three municipalities as regards education for Norwegians born in 1930.27 Nearly one fourth of these 75 year-olds were bicycling, running, swimming or skiing, reflecting a very active old population. Our results, however, must be interpreted as observations from a best-case population, both nationally and internationally.
The AF patients had a significantly lower VO2 peak than the controls in sinus rhythm. The difference in VO2 peak is probably of clinical significance; the magnitude corresponds to the difference in mean VO2 peak between 55-59 year-olds and 75-79 year-olds in a Canadian normative population,28 and another study comparing AF patients to a normal control group showed similar results.29
The recommended reference values for VO2 peak are based on studies including patients up to 74 years,30 and only one study provides normative data for the older Canadian population based on an incremental maximal exercise test.28 This illustrates that maximal exercise testing in older patients may be controversial. No adverse events occurred during the present exercise testing, and we have found no evidence documenting that age or AF are contraindications to maximal exercise testing.31
The distribution of the mental QoL within the AF group was bimodal, identifying two different AF subgroups. This suggests also a psychological approach to the AF patients with most complaints. There were significantly increased odds for poor physical QoL in AF patients compared to the controls without AF. The median physical QoL score was 11.5 points lower in AF patients compared to controls, and this corresponds to the gender-matched difference in mean PCS between Norwegian 30-39 year olds and 70-80 year olds.11 This illustrates the clinical relevance of the lower physical QoL score in AF patients, even though the comparison within normative age groups is confounded by the different expectations various age groups have to their physical QoL. When stratifying PCS into males versus both genders combined, the odds changed markedly, reflecting that female AF patients report much poorer physical QoL than their controls, compatible with previous reports of impaired QoL in women with AF.32,33
The AF patients used more medication than the controls, even when assuming that AF per se justified one anticoagulant and one rate-controlling drug. A history of compensated chronic heart failure and/or valvular heart disease was found almost exclusively in AF patients. The poorer physical QoL and VO2 peak in AF patients could be partly explained by their increased comorbidity. However, taking into consideration the substantial confounding effects, the adjusted odds for poor outcomes for the AF patients compared to non-AF controls were considerably increased. Even when adjusting for the diagnoses closely associated with AF; a history of chronic heart failure and valvular heart disease, the adjusted odds estimates were strengthened, emphasizing that AF is responsible for impaired physical QoL and reduced exercise capacity.
The main limitation of the present study is the low number of patients. This is in part compensated for by the fairly high participation rate from the eligible subjects and the homogeneity of the population addressed. We have no indication of non-responder bias, neither in the AF, nor in the control group. However, the conclusions may be valid only for well-situated 75 year-old citizens in a society offering good health care services. AF patients living under poorer conditions presumably fare worse.
In this out-of hospital-population patients with permanent AF had lower exercise capacity and higher odds for poor physical QoL compared to controls without AF, also after adjusting for confounders. The AF per se, and not comorbidity, seems to be responsible for this. The majority of the AF patients had a fair score for mental QoL. The bimodal distribution of mental QoL in AF patients, however, suggests that a minority of the AF population have considerably reduced mental QoL.