Beating-heart Thoracoscopic Left Atrial Appendage Exclusion in a Patient with Left atrial Thrombus
Ali Khoynezhad1
1Director of Cardiovascular Surgery, MemorialCare Long Beach Medical Center, Clinical Professor of Surgery, David Geffen School of Medicine at UCLA, Los Angeles, CA..
Stroke remains a major complication of atrial fibrillation and third leading cause of death in Western Countries. [1] While Coumadin and novel oral anticoagulants have been efficient in reducing the stoke risk in patients with atrial fibrillation; there is a subset of patients who are not candidates for anticoagulation.[2] The management of these patients is clinical challenge.We describe a patient with history of permanent atrial fibrillation with contra-indication to anticoagulation presenting with and left atrial thrombus. She was treated with novel generation of epicardial left atrial appendage exclusion device.
Key Words : atrial fibrillation, left atrial thrombus, left atrial appendage exclusion, left atrial occlusion.
Correspondence to: Ali Khoynezhad, M.D., Ph.D., FHRS
Co-Director, Atrial Fibrillation Program
Professor of Cardiovascular Surgery
Cedars-Sinai Medical Center
Los Angeles, CA.
Management of left atrial thrombus in patients with significant gastrointestinal bleeding is a challenge for treating clinician.European guidelines recommend left atrial appendage exclusion for patients with an absolute or relative contraindication for oral anticoagulation.[3] The presence of a thrombus in the left atrial appendage is considered as a contraindication to percutaneous exclusion, as manipulation of catheters, guide wires, sheaths or devices in the left atrial appendage may lead to systemic embolization.
A 66-year-old female was presented with history of hypertension, ischemic cardiomyopathy with left ventricular ejection fraction of 29%, s/p PCI and Biventricular ICD implantation and permanent atrial fibrillation for 15 years, s/p atrioventricular node ablation. Her CHADSVASC score was 6 and her HASBLED score was 5. She was taken off dabigatranetexilate six months earlier due to two episodes of lower gastrointestinal bleeding requiring hospitalization and two united packed blood cells transfusion. Her workup by the gastroenterology was negative for any tumor, vascular anomalies or other sources of gastrointestinal bleeding. Subsequently, she was presented with left embolic stroke four months ago with right lower extremity paresis. Another trial of anticoagulation – this time with Coumadin – led to repeat hospitalization and lower gastrointestinal bleeding a month later, and therefore the Coumadin was stopped. Now, she is once again presented with recurrent left frontal embolic stroke and evidence of significant clot burden in left atrial appendage and computer tomography scan and transesophageal echocardiography [Figure 1],[Figure 2].
Figure 1. This figure illustrates presence of thrombus in the left atrial appendage on the preoperative cardiac computer tomography angiogram.
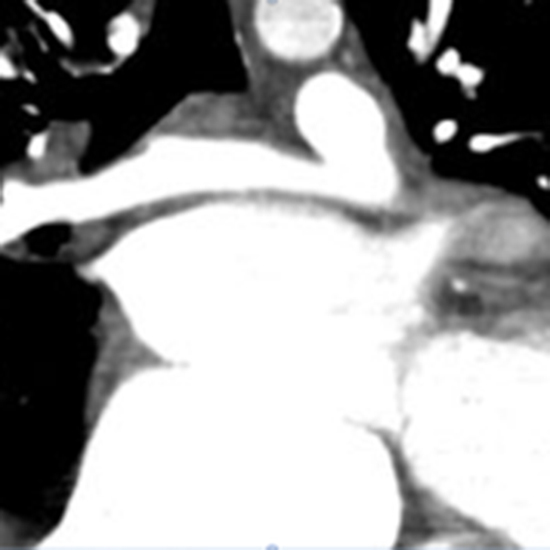
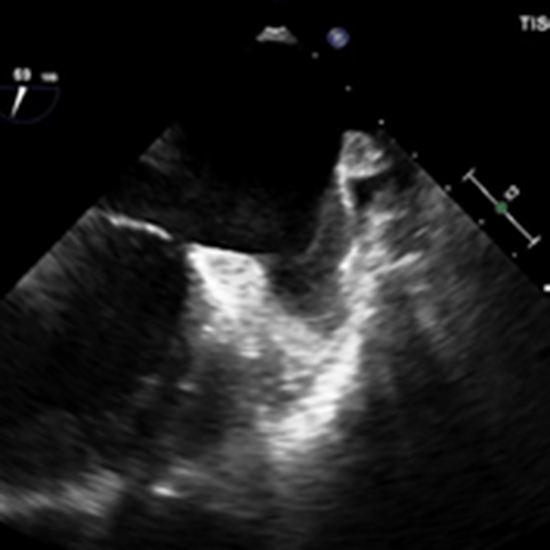
Figure 2. This figure confirms a large thrombus in the left atrial appendage on the intraoperative transesophageal echocardiography.
This patient was discussed in the multi-disciplinary conference.She was felt not to be a candidate for any endocardial or epicardial left atrial appendage exclusion by the interventional cardiology and electrophysiology team due to concerns of intra-procedural dislodgement of left atrial clot and recurrent episode of gastrointestinal bleeding. The only brainstorm adoption was to use thoracoscopic beating-heart approach using a hoopless open-ended surgical exclusion device. Everyone agreed that there is still significant risk of embolization of left atrial appendage thrombus during this procedure, and that risk of recurrent stroke without exclusion of the left atrial appendage is even higher. After discussing the risks and benefits with the patient as part of an informed consent, she decided to proceed.
The procedure was performed in the operating room under general anesthesia and double-lumen intubation. Two five mm ports and a twelve mm port was placed in left axillary line after the left lung was deflated and CO2 insufflation
The pericardium was opened two cm under the phrenic nerve and the entire left atrial appendage was exposed. Using atraumatic grasper the tip of the appendage was gently grabbed, the basis was sized to be 40mm.Through the12mm port, a 40mm AtriClip Pro-V (AtriCure, Mason,OH) was introduced and placed across the basis of the left atrial appendage with minimal manipulation, effectively exclude blood flow into the left atrial appendage. Under transesophageal echocardiography, complete exclusion of the left atrial appendage from circulation was confirmed. [Figure 3] All the instruments and ports were removed and the port skin incisions were closed under Valsalva maneuver. The patient tolerated the 25-minute procedure well, was extubated and transferred to postoperative care unit with no new neurologic findings, and discharged home two days later.
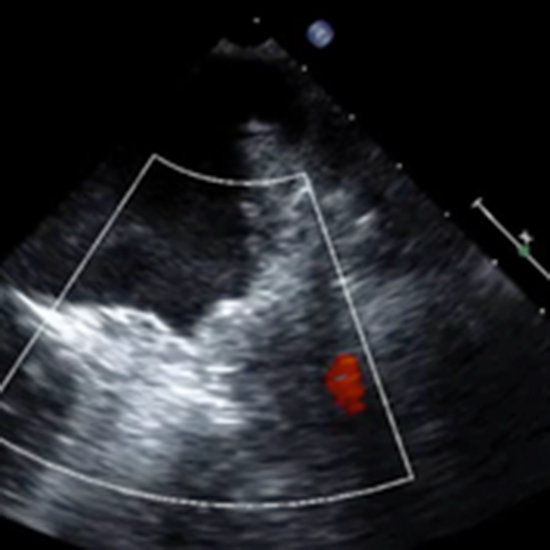
Figure 3. This image depicts postoperative transesophageal echocardiography images after placement of the AtriClip PRO-V.
Patients with high CHADSVASC score have a significant stroke risk without effective systemic anticoagulation.[2] These patients should be considered for endocardial exclusion of left atrial appendage. Management of patients with significant thrombus burden in the left atrial appendage and contraindication to anticoagulation is a challenging clinical condition. These patients are typically not candidates for any endocardial or epicardial closure techniques due to the risk of dislodgement and embolization. AtriClip has been evaluated and FDA-approved after the multi-center prospective EXCLUDE clinical trial (Exclusion of Left Atrial Appendage with AtriClip Exclusion Device in Patients Undergoing Concomitant Cardiac Surgery) assessed the safety and efficacy of left atrial exclusion.[4] In this patient, a novel version of AtriClip was used to exclude the appendage. This device is designed without a hoop end effector and the clip is also open-ended, allowing for minimal manipulation of the left atrial appendage during deployment. Given recent release, the experience with AtriClip Pro-V in this clinical setting is limited. There are recent reports of transcatheter exclusion of left atrial appendage in setting of left atrial clot using cerebral embolic protection. [5]-[6]
Although the use of cerebral protection systems is reasonable in this context, this type of device was not in this case for several reasons. Firstly, the use of such devices needs arterial vascular access and catheter and device manipulation in the aortic arch, and extends the duration of the procedure, which may increase the risk of perioperative complications and aorta-embolic stroke in this fragile patient. Secondly, embolic events can occur despite the use of the embolic protection devices.[7]
The rate of stroke in patients with left atrial thrombus is unknown. This case report, to our knowledge, is the first published report of the utility of an epicardial device in a patient with left atrial thrombus and absolute contraindication to anticoagulation, where there are no great alternatives.
Author is national prince investigator and consultant for AtriCure. No funding was received for this manuscript.