Intraluminal Esophageal Temperature Monitoring Using the Circa S-Cath™ Temperature Probe to Guide Left Atrial Ablation in Patients with Atrial Fibrillation
Sapan Bhuta, Jonathan Hsu, Kurt S. Hoffmayer, Michael Mello, Thomas Savides, Malek Bashti, Jessica Hunter, Kathryn Lewis, Gregory K. Feld
Division of Cardiology, Cardiac Electrophysiology Program, and the Division of Gastroenterology, UCSD Health System, University of California, San Diego.
Radiofrequency catheter ablation is a common treatment for atrial fibrillation (AF), during which thermal esophageal injury may rarely occur and lead to an atrio-esophageal fistula. Therefore, we studied the utility of the Circa S-Cath™ multi-sensor luminal esophageal temperature (LET) probe to prevent esophageal thermal injury.
Thirty-six patients, enrolled prospectively, underwent circumferential or segmental pulmonary vein isolation for treatment of AF. A maximum ablation electrode temperature of 42ºC was programmed for automatic power delivery cutoff. In addition, energy delivery was manually discontinued when the maximum LET on any sensor of the probe rose abruptly (i.e. ˃0.2ºC) or exceeded 39º C. Esophagoscopy was performed immediately after ablation in 18 patients (with the temperature probe still in place) and at approximately 24 hours after ablation in 18 patients. Esophageal lesions were classified as likely traumatic or thermally related. Of the 36 patients enrolled in the study, 21 had persistent and 15 had paroxysmal AF, average LVEF 57±16% and CHA2DS2VASc score 1.6±1.2 (range 0-4). Average maximum LET was 37.8±1.4ºC, power delivery 31.1±8 watts and ablation electrode temperature 36.4±4.1ºC. Average maximum contact force was 44.5±20.5 grams where measured. Only 1 patient (<3%) had an esophageal lesion that could potentially represent thermal injury and 4 patients (11.1%) had minor traumatic mechanical injury.
LET guided titration of power and duration of energy application, using an insulated multi-sensor esophageal temperature probe, is associated with a low risk of esophageal thermal injury during AF ablation. In only rare cases, LET monitoring resulted in the need to manipulate the esophagus to avoid unacceptable temperature rises, that could not be achieved by adjustment of power and duration of energy application.
Key Words : Atrial fibrillation, Ablation, Esophagus, Esophageal temperature probe, Atrio-esophageal fistula.
Gregory K. Feld, MD
9444 Medical Center Dr.
La Jolla, CA 92037
Radiofrequency catheter ablation (RFCA) to electrically isolate the pulmonary veins from the left atrium (LA) has become a first-line treatment for symptomatic atrial fibrillation (AF).1 However, damage to the esophagus, may occur during ablation of the posterior LA wall, leading to the potentially fatal complication of atrio-esophageal (AE) fistula.2,3,4 Esophagoscopy (EG) following AF ablation has revealed an incidence of thermal injury up to 47% following RFCA for AF.5-11. Fortunately, AE fistula is a rare complication of AF ablation, with a reported incidence of only 0.03–0.2%.12-14 The mortality rate from AE fistula is very high, and thus preventing its occurrence is critically important.
Several strategies have been implemented to decrease the risk of esophageal injury, including limitation of power in the posterior LA wall, perpetual motion of the ablation catheter, identifying the anatomic location of the esophagus during RFCA and avoiding it entirely, displacement of the esophagus away from the ablation catheter, and intra-luminal cooling of the esophagus.15-18 Luminal esophageal temperature (LET) monitoring to limit power and duration of ablation in proximity to the esophagus, and to indicate the need for esophageal manipulation to avoid LET rises, is another alternative approach available during AF ablation procedures. Monitoring LET with a single sensor temperature probe, may be ineffective and inconvenient due the need to continually move the temperature probe relative to a rapidly moving ablation catheter. Furthermore, even with the use of a single sensor LET monitor, esophageal ulceration has still been reported.7-9,11 Therefore, a new, multi-sensor esophageal probe [Figure 1], which monitors LET at 12 insulated temperature sensors placed uniformly along the length and width of probe, eliminating the need to continuously move the probe once in place, has been developed by Circa Scientific, LLC (Circa Scientific, Inc., Englewood, CO, USA).
Figure 1. AP fluoroscopic image of Circa temperature probe (Circa S-Cath™) in the esophagus during AF ablation procedure, with a steerable deca-polar catheter in the coronary sinus (CS).
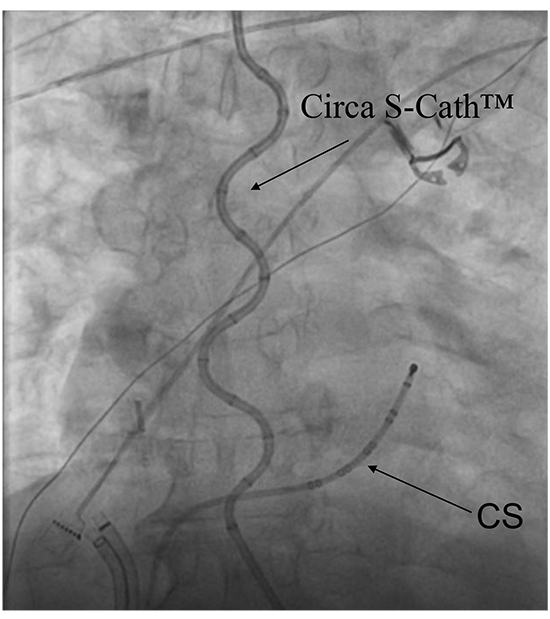
Although we currently use the Circa S-Cath™ esophageal temperature probe to monitor esophageal position and LET in all of our AF ablation cases, this study was designed to evaluate the ability of the Circa S-Cath™ multi-sensor LET probe to prevent esophageal thermal lesions, as observed by esophagoscopy, in a prospective series of patients undergoing RFCA for AF.
Thirty-six patients undergoing RFCA for symptomatic, drug-refractory AF, were enrolled in this study. Ablations were performed by three experienced electrophysiologists, with two electrophysiologists performing primarily wide area circumferential pulmonary vein (WACA) ablation and one electrophysiologist performing both segmental ostial PV isolation (SPVI) and WACA. Consequently, 3 patients underwent SPVI and 33 patients underwent WACA.
For LET monitoring a Circa S-Cath™ esophageal temperature probe with 12 sensors (Circa Scientific, Inc., Englewood, CO, USA) was used to continuously record the intraluminal esophageal temperature [Figure 1]. The probe was inserted orally by the anesthesiologist, under fluoroscopic guidance and advanced into the esophagus, after general anesthesia and endotracheal intubation. The probe was advanced with its stylet in place to straighten the probe, until the temperature sensors spanned the left atrium from the cranial to caudal direction (approximately from the left main-stem bronchus to the coronary sinus), and then the stylet was removed and the probe visualized fluoroscopically to ensure adequate positioning. The probe has a sinusoidal shape, which may be variably distorted by esophageal pressure, but is usually retained after placement [Figure 1]. The accuracy of the thermistor is reported by the manufacturer to be ± 0.3ºC. The 12 temperature sensors are 2.5 mm in length and separated by approximately 10 mm when deployed. The multi-sensor probe was connected to the Circa Temperature Monitoring System (CS-1000 Circa Temperature Monitoring System, Circa Scientific, Inc., Englewood, CO, USA) with continuous maximum temperature displayed.
All patients in this study underwent general anesthesia prior to ablation. Anticoagulation was administered prior to ablation in a standard manner.Via the left femoral vein a steerable decapolar catheter (Webster CS catheter, Biosense Webster, Inc, Diamond Bar, CA, USA or Polaris catheter, St. Jude, St. Paul, MN, USA) was placed in the coronary sinus for pacing and recording, and an intracardiac ultrasound (ICE) catheter (AccuNav, Siemens, Mountain View, CA, USA) was positioned in the right atrium to guide the trans-septal puncture.Via the right femoral veintwo trans-septal sheaths were positioned in the LA. Intravenous heparin was administered prior to trans-septal puncture followed by a continuous infusion, to maintain an activated clotting time of 300–350 seconds. Using a circular mapping catheter (Lasso™, Biosense Webster, Inc., Diamond Bar, CA, USA) electroanatomical maps and a 3D geometry were created using the Carto (Biosense Webster, Inc., Diamond Bar, CA, USA), Ensite Velocity or Precision systems (St. Jude Medical, St. Paul, MN, USA). An externally irrigated ablation catheter (Thermocool SmartTouch™ or ST/SF™, Biosense Webster, Inc., Diamond Bar, CA, USA or TactiCath™, St. Jude Medical, St. Paul, MN, USA) was used for ablation. The PVs were isolated by delivery of RF applications circumferentially or segmentally to the antral or ostial regions of the PVs, respectively, as required to produce a minimum of entrance block for at least 30 minutes, confirmed during isoproterenol infusion at 20 mcg/min. Either a Stockert™ generator (Biosense Webster, Inc.™, Diamond Bar, CA, USA) or CoolPath™ generator (St. Jude Medical, Inc., St. Paul, MN, USA) was used to deliver RF energy, depending on the type of ablation catheter used. Catheter tip temperature, power, and impedance were recorded for each RF energy application. The power delivered to the posterior LA wall during each ablation was varied according to the LET measured by the Circa S-Cath™ esophageal temperature probe, with a maximum power of 30-40 watts (30 watts for Thermocool ST/SF™ catheters) and maximum electrode-tissue interface temperature of 42ºC. Energy delivery was discontinued immediately in all cases when the maximum LET on any sensor of the Circa S-Cath™ temperature probe rose abruptly (i.e. by ˃0.2ºC/sec, due to manufacturer stated device accuracy of ±0.3ºC) or exceeded 39º C. These parameters were used due to the fact that, in our clinical experience prior to this study, if the LET rose abruptly or approached 39º C, it would typically continue to rise and often exceed these limits for several seconds after energy delivery was interrupted. If energy delivery was interrupted due to the LET exceeding these parameters during initial ablation at any location, ablation was resumed at the same area after LET returned to baseline measurement, but at a lower power (i.e usually in increments of 10 watts lower than initial power). If LET then again rose above the limits stated above, ablation was terminated immediately, and the esophagus manipulated away from the ablation catheter (using the same endoscope subsequently used to evaluate the esophagus for any lesions created during the ablation procedure as described in the next paragraph) in order to avoid further LET rises and complete the pulmonary vein isolation (PVI) procedure. Esophageal manipulation was only required however in two patients in the entire study (as noted below). When LET rises were not observed during the procedure, ablation energy was delivered for up to 30 seconds at each location until there was complete PVI.
Esophagoscopy was performed in all patients by a trained interventional endoscopist, either immediately after the ablation with the temperature monitoring probe still in place (18 patients) or the day after ablation (18 patients). Lesions were identified, photographed, and classified by the endoscopist performing the esophagoscopy immediately after the study. Any esophageal lesions observed were classified as pre-existing diagnostic abnormalities, or either traumatic or thermally related to the procedure.
After discharge, as part of our standard-of-care, patients were seen in the outpatient arrhythmia clinic at 1, 6, 12 and 24 months for any possible procedure related complications, and to assess for any AF recurrence (not reported in this study).
Continuous variables have been expressed as the mean ± one standard deviation, and statistical significance was calculated using the Student’s t-test. Categorical variables have been expressed as absolute numbers or percentages, and statistical significance was calculated using the Chi-squared test. A statistically significant difference between variables required a p value ≤0.05. All statistical analysis was performed using Microsoft Excel 2010.
Participation in the study was entirely voluntarily and all participants provided written informed consent prior to enrollment. The study was approved by the UCSD Institutional Review Board and registered with ClinicalTrials.Gov (IRB#150018, CT.GOV#NCT02467166).
Thirty-six patients, 31 males and 5 females, average age 64.2±9.8years, with an average LVEF of 56.5±16.17% and an average CHA2DS2VASc score of 1.6±1.2 (range 0-4), undergoing RFCA for symptomatic, drug-refractory AF, were enrolled in this study. There were 21 patients with persistent AF (i.e. >7 days in duration) and 15 with paroxysmal AF (i.e. <7 days in duration). The patient demographics and clinical characteristics are summarized in [Table 1].
Table 1. Baseline Characteristics
| Patients |
36 |
| Age |
64.2 ± 9.8 years |
| Gender (Male) |
31 Male / 5 Female |
| LVEF |
56.5 ± 16.2% |
| CHA2DS2VASc Score |
1.6 ± 1.2 |
| Female Gender |
5 pts |
| Age >=65 & <=74 |
15 pts |
| Age >75 |
5 pts |
| CHF |
7 pts |
| HTN |
23 pts |
| DM |
5 pts |
| CVA/TIA/TE |
2 pts |
| Vascular Disease |
1 pts |
Esophageal Temperature Monitoring
In our clinical experience, an abrupt increase in LET above baseline was typically observed only when ablation was performed with the ablation electrode visually estimated to be within 10 mm from the Circa S-Cath™ temperature probe on the posterior wall of the LA. Thus, only ablations performed on the posterior LA wall, within a visually estimated 10 mm of the temperature probe where significant LET rises were typically observed, were included for analysis in this study. Using the Circa S-Cath™ temperature probe’s maximum temperature reading function to adjust and limit power delivery during ablation, the average maximum LET observed in all patients was 37.8±1.42ºC (range 36.90-39.50ºC). During ablation, the average maximum power delivered was 31.08±8.02 watts and the average maximum ablation electrode temperature was 36.4±4.10ºC. Contact force was recorded in 29 patients when using a contact force measuring catheter (i.e. Thermocool SmartTouch™ or ST/SF™, Biosense Webster, Diamond Bar, CA, USA), and in these patients the average maximum contact force was 44.5±20.5 grams (average average contact force of 24±7.9 grams and minimum average contact force of 11.1±5.5 grams). Esophageal manipulation with the endoscope to move the esophagus away from the ablation electrode, was required in only two patients in this study (#12 and 20) in order to avoid study defined LET rises. In neither of these patients was any esophageal thermal or traumatic injury noted during esophagoscopy. These procedural data are summarized in [Table 2].
Table 2. Procedure Data
| Pt |
Ablation Type |
Catheter Type |
Circa Temp Maximum (C) |
Catheter Temp Maximum (C) |
Catheter Power Maximum (W) |
Contact Force Maximum (g) |
| 1 |
SVPI |
ST |
38.00 |
41.00 |
40.00 |
66.00 |
| 2 |
WACA |
ST |
38.90 |
36.00 |
35.00 |
32.00 |
| 3 |
WACA |
ST |
38.40 |
40.00 |
36.00 |
42.00 |
| 4 |
WACA |
ST |
37.70 |
42.00 |
50.00 |
45.00 |
| 5 |
WACA |
ST |
36.90 |
40.00 |
40.00 |
69.00 |
| 6 |
WACA |
ST |
38.20 |
40.00 |
25.00 |
47.00 |
| 7 |
WACA |
ST |
37.00 |
41.00 |
44.00 |
39.00 |
| 8 |
WACA |
ST |
38.10 |
37.00 |
30.00 |
47.00 |
| 9 |
WACA |
TactiCath |
38.10 |
36.00 |
20.00 |
NA |
| 10 |
WACA |
ST |
37.10 |
38.00 |
30.00 |
NA |
| 11 |
WACA |
ST |
38.30 |
37.00 |
25.00 |
NA |
| 12 |
WACA |
ST |
38.50 |
41.00 |
40.00 |
NA |
| 13 |
WACA |
ST |
38.20 |
38.10 |
41.00 |
73.00 |
| 14 |
WACA |
ST |
37.40 |
39.00 |
30.00 |
59.00 |
| 15 |
WACA |
ST |
37.90 |
39.00 |
40.00 |
NA |
| 16 |
WACA |
ST |
39.00 |
32.80 |
21.00 |
NA |
| 17 |
WACA |
ST |
37.70 |
39.00 |
30.00 |
NA |
| 18 |
WACA |
ST |
37.20 |
36.00 |
25.00 |
67.00 |
| 19 |
WACA |
ST |
38.20 |
35.50 |
36.00 |
43.00 |
| 20 |
WACA |
ST |
37.40 |
42.00 |
42.00 |
24.00 |
| 21 |
WACA |
ST |
37.90 |
39.10 |
36.00 |
23.00 |
| 22 |
WACA |
ST |
38.20 |
28.80 |
25.00 |
39.00 |
| 23 |
WACA |
TactiCath |
38.50 |
38.00 |
25.00 |
13.00 |
| 24 |
WACA |
TactiCath |
37.50 |
33.00 |
40.00 |
32.00 |
| 25 |
WACA |
TactiCath |
38.50 |
37.90 |
20.00 |
v |
| 26 |
WACA |
TactiCath |
37.80 |
38.00 |
30.00 |
20.00 |
| 27 |
SVPI |
TactiCath |
37.30 |
37.70 |
30.00 |
46.00 |
| 28 |
WACA |
ST |
38.00 |
30.90 |
30.00 |
53.00 |
| 29 |
WACA |
ST |
30.40 |
37.70 |
20.00 |
55.00 |
| 30 |
WACA |
ST |
39.50 |
30.50 |
15.00 |
24.00 |
| 31 |
WACA |
ST |
37.50 |
24.00 |
25.00 |
20.00 |
| 32 |
WACA |
ST |
38.00 |
32.80 |
31.00 |
67.00 |
| 33 |
WACA |
ST |
39.00 |
32.90 |
26.00 |
98.00 |
| 34 |
WACA |
TactiCath |
39.40 |
34.00 |
30.00 |
36.00 |
| 35 |
WACA |
ST |
37.60 |
31.40 |
31.00 |
68.00 |
| 36 |
SPVI |
TactiCath |
37.90 |
32.00 |
25.00 |
21.00 |
| Avg |
|
|
37.81 |
36.36 |
31.08 |
44.48 |
| SD |
|
|
1.42 |
4.10 |
8.02 |
20.46 |
All values represent the average of the maximum observed during each ablation, for each patient. WACA = wide area circumferential pulmonary vein ablation, SPVI = semgmental pulmonary vein isolation, NA = not available, Safire™ = 8 mm solid tip ablation catheter from St. Jude, Inc., ST = SmartTouch, gms = grams, TactiCath™ = Irrigated force sensing catheter from St. Jude, Inc., Temp = Temperature in degrees centigrade
Among the 36 patients in this study, only 1 lesion was observed in a region of the esophagus near where ablation may have been performed (i.e. described as a 3 mm edematous mucosal lesion at 32 cm from the incisors) that could possibly be related to thermal injury to the esophagus [Figure 2]. Among the 18 patients undergoing esophagoscopy immediately after ablation, one had a small 3 mm linear erosion of the mucosa and one had a small area of linear erythema both thought to be possibly due to mechanical trauma. Among the 18 patients undergoing esophagoscopy one day after ablation two were observed to have small 3 mm superficial mucosal erosions also thought to be possibly due to mechanical trauma, and one had a 3 mm focus of edematous mucosa without erosion, which was thought to be possibly due to ablation (i.e. a thermal injury lesion). Although there were no statistically significant differences in average LET, catheter temperature, power or contact force between this patient with a possible esophageal thermal injury and those who did not have any thermal injury, this particular patient did have the highest maximum transient LET observed of any in either group at 39.5 ºC. There were no ulcerations observed in any patients. Other incidental findings, also observed during esophagoscopy, included a small inlet pouch in 2 patients, Barrett’s esophagus in 3 patients, mild to moderate erosive esophagitis in 3 patients, and a hiatal hernia in 2 patients. No patients in this study developed evidence of an atrio-esophageal fistula during follow-up.
Figure 2. Esophagoscopy image showing a 3 mm edematous mucosal lesion at 32 cm from the incisors that could possibly be related to thermal injury to the esophagus.
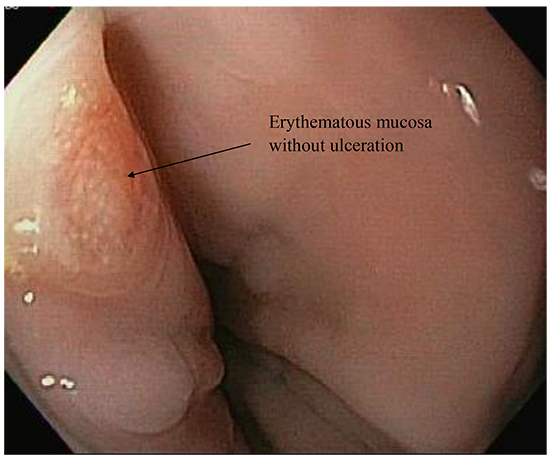
This study shows that when ablation power and duration of energy application are guided by the LET determined using an insulated multi-sensor esophageal temperature monitoring probe, there will be very little esophageal thermal injury during AF ablation, as confirmed by esophagoscopy in this study.
Limitation of Esophageal Injury during AF Ablation by LET Monitoring
Monitoring LET during AF ablation may limit esophageal thermal injury, especially when ablation is performed in close proximity (<1 cm) to the esophagus, by forcing the operator to reduce power delivery or duration of energy application, in order to maintain maximum LET at or below 39 ºC and average maximum LET below 38ºC. Previously reported data suggests that a correlation exists between LET and esophageal thermal injury6,9,11,21, and that monitoring LET to guide ablation, including both power and duration of energy application, has been shown to reduce the risk of esophageal ulceration5,11. Thus, an ablation strategy guided by LET temperature monitoring seems logical, but there may be some limitations in this approach too, considering that LET may underestimate the surface temperature of the esophagus during ablation, as noted in previous studies22.
In this study, we used stringent limitations on power and duration of energy application guided by LET monitoring and demonstrated a near complete elimination of thermal esophageal injury (only 1 lesions was observed in 1 patient in this study or 2.8% that might possibly have been related to thermal injury) during pulmonary vein isolation. Importantly, limitation of power and duration of energy application to prevent LET rises did not compromise the ability to isolate the pulmonary veins acutely, as all veins were successfully isolated based on standard current criteria for success.
The mere presence of a LET temperature monitoring probe during ablation or the type of LET monitoring probe used, are factors that have been considered potential causes of increased risk of thermal injury with their use in the past18,19,20. However, it appears that the use of uninsulated metallic electrodes on the esophageal temperature monitoring probe may produce the increased risk of thermal injury, rather than the presence of the monitoring probe itself producing displacement of the esophagus towards the left atrium19,20,23. The use of an insulated probe (Circa S-Cath™ LET monitoring probe), as done in this study, was not associated with an increased risk of esophageal thermal lesions, compared to that previously reported in the literature.
Our study was not randomized but was prospective. For this study, esophagoscopy was performed by a single trained interventional endoscopist, who was also familiar with our techniques, which should have minimized the risk of missing significant esophageal lesions. In addition, several unrelated esophageal abnormalities were observed by the endoscopist, suggesting that it would be unlikely that thermal lesions would have also been missed. There was also no control group of patients undergoing ablation in this study using a standard single sensor temperature probe to compare the frequency of lesion detection during esophagoscopy, however this has been reported extensively in the literature and the development of potential thermal lesions was much higher than observed in this study. Another potential limitation of this study arises from the initial design of this study wherein the first 18 patients underwent EGD immediately after ablation and the second 18 patients underwent EGD approximately 24 hours after ablation. This could have allowed any potential thermal lesions to mature and become more visible to the endoscopist. Therefore, it is possible that the early EGD could have missed lesions that would have otherwise become evident if allowed to mature for 24 hours. Lastly, this study was not powered to determine if ablation guided by esophageal temperature monitoring had any effect on long-term outcome of AF recurrence, after PV isolation.
Monitoring LET, as done in this study using an insulated multi-sensor temperature probe (Circa S-Cath™), allowed the operator performing AF ablation to adjust radiofrequency power output and energy application duration, to prevent LET rises above a critical level thought to be responsible for thermal esophageal injury, which may be related to subsequent development of atrio-esophageal fistula. In only rare cases, was adjustment of power and duration of energy delivery unsuccessful in minimizing LET rises within study limits, so as to avoid esophageal manipulation. Furthermore, this ablation strategy did not compromise success in achieving pulmonary vein isolation acutely.