A Simplified Trans-Septal Puncture Technique using a Needle Free Approach for Cryoablation of Atrial Fibrillation
Adam J Graham, Shohreh Honarbakhsh, Ben O’Brien, Richard J Schilling
This author takes responsibility for all aspects of the reliability and freedom from bias of the data presented and their discussed interpretation.
Trans-septal puncture (TSP) is routinely performed during treatment of atrial fibrillation (AF) and other electrophysiology procedures. The purpose of this retrospective observational study was the analysis of a novel needle free technique employed to gain access to the left atrium (LA).
The SafeSept Needle Free guidewire was delivered, using no needle, to the interatrial septum via a standard cryoablation sheath and dilator under transoesophageal guidance. The wire was then advanced into the LA with position confirmed by fluoroscopy. All cases were performed under general anaeasthetic (GA).
The novel procedure was performed in 43 patients (38 paroxysmal AF (88.4%) and 5 persistent AF (11.4%)) with 100% success rate in accessing the LA. The procedure times (51.70 ±18.18) and fluoroscopy times (2.75 ± 3.35) were recorded. There were no complications seen in the cohort.
Using SafeSept Needle Free wire for TSP had a high success rate and resulted in no complications, with the potential to reduce procedure and fluoroscopy times.
Key Words : Atrial Fibrillation, Cryoablation, Trans-septal puncture, Needle-Free, Safe-Sept.
Correspondence to: Adam J. Graham, MBBS, MRCP, BSc. Barts Heart Centre Flat 29 Highbury Gardens 52 Holloway Rd Islington N7 8BU
The origins of trans-septal puncture (TSP) lie in its use for left heart catheterization. However, studies for the evaluation of valve disease or percutaneous mitral balloon valvuloplasty indicate that it is now more commonly performed to access into the left atrium (LA) for catheter ablation of arrhythmia[1][2]. The original technique first described by Ross et al. in 1960[3] has evolved over the subsequent years. This means that while the use of ultrasound imaging has increased, the techniques and technologies used are not specifically designed for the purpose they are being put to today[4]. An increase in atrial fibrillation ablation procedures facilitated the development of specific techniques and the adoption of new technologies to assist TSP such as the RF needle[5]. However, it is well known that TSP is related to some life-threatening complications. This is especially true in the presence of challenging interatrial septal anatomy[2]. We sought to investigate whether a novel TSP puncture wire, the SafeSept Needle Free guidewire (SafeSeptTM Pressure Products, San Pedro, CA, USA), could be used through a cryoablation sheath to reduce procedural steps such as sheath and wire exchanges.
In this retrospective observational study, a total of 43 consecutive patients undergoing pulmonary vein isolation using cryoballoon were analysed. TheTSP procedures were performed under general anesthetic using the SafeSept Needle Free guide wire (SafeSeptTM Pressure Products, San Pedro, CA, USA) with Transoesophageal (TOE) guidance without interrupting oral anticoagulation therapies.
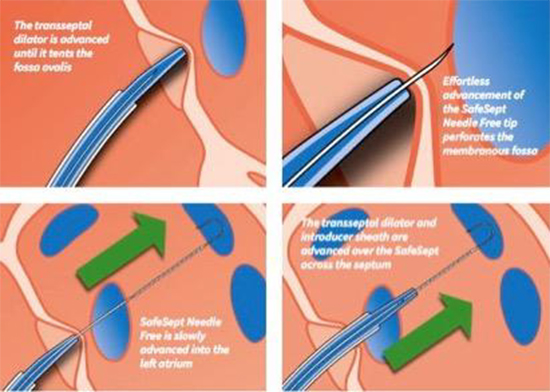
Seldinger technique was used to gain femoral venous access and introduce a cryoablation sheath (Flexcath AdvanceTM Steerable Sheath, Medtronic, Minneapolis, USA) with the tip placed in the SVC under TOE guidance (no fluoroscopy was used for this part of the procedure). No problems were encountered advancing the sheath with the support of the guidewire. A second 7F sheath was used to introduce a pacing wire into the SVC to pace the phrenic nerve during right pulmonary vein freezes. The guide wire was withdrawn from the cryoablation sheath and a SafeSept wire advanced to the mid portion of the sheath and dilator. The SafeSept wire is a 150cm, 0.0315” nitinol guidewire with a sharp tip and a radio-opaque distal coil. When unsupported by sheath and dilator it has a pre-formed J-shaped tip, a feature designed to render it atraumatic when inside thevasculature [Figure 1]. A bend of 300 was placed on the cryoablation sheath and dilator and they were then slowly withdrawninferiorly under TOE guidance. When the tip of the dilator was seen to drop into the fossa ovalis the SafeSept wire was advanced and used to puncture the septum [Figure 2]. Heparin was given as per local protocol at this juncture. The position of the wire was confirmed on fluoroscopy as being in the left upper pulmonary vein. The sheath and dilator were then advanced through the septum under fluoroscopic guidance and the needle and dilator removed. The cryoablation procedure proceeded as described before[6].
Figure 1. Schematic view of the use of the Needle Free SafeSept wire to cross the atrial septum
Procedure time was defined as time from initial venous puncture to removal of sheaths and measured in minutes. Duration of fluoroscopy was also measured in minutes. Patients were monitored overnight and followed up in clinic 3 months post procedure. They were assessed for standard major and minor complications of AF ablation during these times.
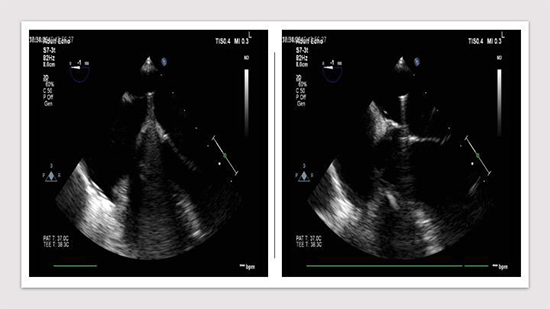
Figure 2. Transoesophageal echocardiography views demonstratetenting of the inter-atrial septum (left) and subsequent advancement into the left atrium (right)
Normal left ventricular function was defined as an ejection fraction above 55%; with normal valvular function defined as no pathological stenosis or regurgitation. Out of those with abnormal LV function all were mildly impaired.
From July 2015 to April 2016 the SafeSept Needle Free guidewire was used to perform TSP in 43 consecutive patients. Baseline characteristics are demonstrated in [Table 1].
Table 1. Demonstrates the baseline characteristics
|
SafeSept Needle Free |
| Age y, mean ± SD |
59.5 ±10.8 |
| Sex M (%) |
34 (79) |
| Hypertension, n (%) |
13 (30) |
| IHD^, n (%) |
2 (4.7) |
| Diabetes, n (%) |
2 (4.7) |
| Echocardiography |
|
| Normal LV function n (%) |
40 (93) |
| Normal valvular function n (%) |
41 (95.3) |
| ^Ischaemic heart disease |
|
^Ischaemic heart disease
The majority of patients in the cohort were undergoing ablation for paroxysmal atrial fibrillation (PAF); 38 PAF, 88.4% and 5 early persistent AF, 11.6% [Table 2]. None had had a prior TSP performed. Most patients had preserved left ventricular systolic function (40/43, 93%; [Table 2]).
Table 2. Demonstrates the indication for catheter ablation, extra procedures performed and the echocardiographic features
| Indications |
SafeSept Needle Free |
| Persistent AF, n (%) |
5 (11.6) |
| Paroxysmal AF n (%) |
38 (81.4) |
| Extra Procedures |
|
| CTI^ Line n (%) |
11 (25.6) |
| EPS* n (%) |
2 (4.7) |
| ^Cavotricuspid isthmus |
|
| *Electrophysiology study |
|
ˆCavotricuspid isthmus *Electrophysiology study
In all patients, the TSP was successful with no complications. Procedure data is shown in [Table 3].
Table 3. Demonstrates the procedural data
|
SafeSept Needle Free |
| Successful TSP n (%) |
43 (100) |
| Procedure time min ± SD |
51.70 ±18.18 |
| Fluoroscopy time min ± SD |
2.75 ± 3.35 |
| Complications n (%) |
0 |
Given the expansion in electrophysiology procedures a variety of techniques designed to improve efficacy and safety of the TSP have been employed[7]. Radio frequency delivery to the inter-atrial septum has been applied with success in cases in which standard techniques have failed [8][5]. A recent study has demonstrated a benefit to deep inspiratory maneuvers[2].
Our study demonstrates for the first time that a specifically designed trans-septal wire can be used without a trans-septal needle to successfully perform TSP; with LA access achieved in all patients. The use of a SafeSept guide wire has been previously described [9],[10], with the larger of these cohorts consisting of 210 patients. These groups’ technique differs from that employed here, using a different model of the guide wire that requires introduction via the lumen of a standard Brockenbrough needle. Successful performance of the TSP occurred in 97.6% the larger cohort and in all 19 patients in the smaller study.
In this cohort of patients, we experienced no complications and this indicates the technique to be safe in this group. Lower fluoroscopy times when compared to those reported in other studies[6], could be due to no fluoroscopy being used until the LA is accessed. This improvement also applied to total procedure time[6], with the simpler work-flow, avoiding the need to exchange sheaths and wires making the procedure more efficient. It may also improve safety, as sheath exchange is one point in the procedure where there is the potential to produce air embolism or lose position of the wires/sheaths.
This study is limited due to it being a retrospective analysis. A larger randomized controlled study would be necessary to conclusively evaluate its validity. Furthermore, we have measured fluoroscopy time and procedure time, which are influenced by the length of the procedure post TSP. Any further evaluation of this technique should focus on fluoroscopy time and procedure duration from RFV sheath insertion to TSP.
Our technique, whilst requiring further evaluation, offers promise of streamlining the trans-septal puncture and potentially reducing procedure and fluoroscopy times with no obvious compromise to safety.